## Management of SSRI-Resistant OCD **Key Point:** This patient shows inadequate response to SSRI monotherapy (only 19% reduction after 10 weeks at therapeutic dose). The next step is antipsychotic augmentation, not switching SSRIs or escalating psychotherapy alone. ### Definition and Diagnosis of Treatment-Resistant OCD **Treatment-resistant OCD** is defined as: - Inadequate response (< 25–35% Y-BOCS reduction) after 8–12 weeks of SSRI at therapeutic dose (e.g., fluoxetine ≥ 100 mg/day) - Adequate psychotherapy adherence (typically ≥ 8 ERP sessions) This patient meets criteria: 10 weeks on fluoxetine 200 mg + 6 CBT sessions with only 19% reduction. ### Evidence-Based Algorithm for SSRI-Resistant OCD ```mermaid flowchart TD A[OCD on SSRI 8-12 weeks]:::outcome --> B{Adequate response?}:::decision B -->|Yes| C[Continue SSRI + ERP]:::action B -->|No| D{Adequate SSRI dose & ERP adherence?}:::decision D -->|No| E[Optimize SSRI dose & ERP intensity]:::action D -->|Yes| F[SSRI-resistant OCD]:::outcome F --> G{First-line augmentation}:::decision G -->|Antipsychotic| H[Add aripiprazole 5-10 mg or risperidone 2-4 mg]:::action G -->|Alternative| I[Switch to clomipramine or increase SSRI dose further]:::action H --> J[Reassess Y-BOCS at 4-6 weeks]:::decision J -->|Response| K[Continue combination]:::action J -->|No response| L[Consider DBS or other augmentation]:::urgent ``` **High-Yield:** Antipsychotic augmentation is the first-line strategy for SSRI-resistant OCD, not switching to another SSRI or clomipramine. ### Antipsychotic Augmentation: Evidence and Mechanism | Antipsychotic | Dose (OCD) | Evidence | Mechanism | | --- | --- | --- | --- | | **Aripiprazole** | 5–10 mg daily | RCTs show 20–30% additional Y-BOCS reduction | Dopamine partial agonist; modulates glutamatergic/serotonergic circuits | | **Risperidone** | 2–4 mg daily | Similar efficacy to aripiprazole | D2 antagonism; augments SSRI effect | | Quetiapine | 100–300 mg daily | Weaker evidence; second-line | Broad receptor antagonism | **Clinical Pearl:** Aripiprazole is preferred over risperidone in OCD because it has a lower risk of metabolic side effects and tardive dyskinesia, making it safer for long-term use. **Mnemonic: RAMP for SSRI-Resistant OCD** — **R**esist switching SSRIs, **A**ugment with antipsychotic, **M**aintain ERP, **P**atient education on 4–6 week timeline. ### Why NOT Switch to Clomipramine? Although clomipramine is a potent serotonergic agent and FDA-approved for OCD, switching from one serotonergic agent to another after inadequate response is less evidence-based than augmentation. Clomipramine is reserved for: - Patients who cannot tolerate SSRIs - Second-line if augmentation fails - Rarely, as monotherapy in treatment-naive patients **Tip:** In NEET PG, when you see "SSRI 8–12 weeks + inadequate response + good adherence," the answer is almost always **antipsychotic augmentation** (aripiprazole or risperidone), not switching or psychotherapy intensification alone. 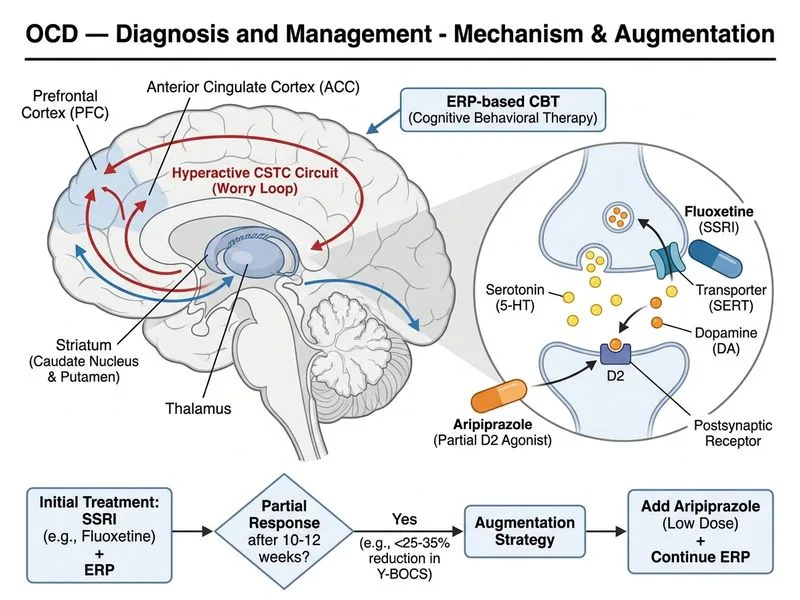
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.