## Differentiation of Open-Angle vs Closed-Angle Glaucoma ### Clinical Context This patient presents with features suggestive of **primary open-angle glaucoma (POAG)**: insidious onset, elevated IOP, characteristic optic disc cupping with vertical elongation, and arcuate visual field loss. The key question asks what MOST helps differentiate this from angle-closure disease. ### Why Anterior Chamber Depth Measurement is Definitive **Key Point:** Anterior chamber depth (ACD) is the single most reliable anatomical parameter that distinguishes open-angle from closed-angle glaucoma at the structural level. - **Open-angle glaucoma**: ACD typically **≥2.5 mm** (often 3–4 mm) - **Closed-angle glaucoma**: ACD typically **<2.5 mm** (often <2 mm), with crowded anterior segment Anterior chamber depth can be measured by: - A-scan ultrasonography (gold standard for ACD measurement) - Optical biometry (IOLMaster) - Anterior segment OCT (AS-OCT) — increasingly used in clinical practice - Slit-lamp estimation (qualitative, less precise) ### Why Other Options Are Insufficient for Differentiation #### Option 0: Superior Arcuate Visual Field Defect - While arcuate defects are **classic for POAG**, they are NOT pathognomonic. - Closed-angle glaucoma can also produce arcuate or other field defects if chronic or after acute episodes with residual optic nerve damage. - Visual field pattern reflects **functional damage** (optic nerve loss), not the **anatomical mechanism** (angle configuration). #### Option 2: Absence of Iris Bombé and Normal Pupillary Reflex - Iris bombé (forward bulging of iris) is seen in **acute angle-closure** with pupillary block, not in chronic or subacute presentations. - Many patients with **chronic angle-closure glaucoma** have normal iris contour and normal pupillary reflexes because the angle closure is **gradual and asymptomatic**. - This finding cannot reliably exclude angle-closure disease. #### Option 3: Elevated IOP with Normal Episcleral Venous Pressure - Both open-angle and closed-angle glaucoma can present with elevated IOP. - Episcleral venous pressure elevation is NOT a distinguishing feature between the two types. - This finding relates to **aqueous humor outflow dynamics** but does not clarify the **anatomical angle status**. ### High-Yield Comparison Table | Feature | Open-Angle Glaucoma | Closed-Angle Glaucoma | |---------|---------------------|----------------------| | **Anterior Chamber Depth** | ≥2.5 mm (wide) | <2.5 mm (shallow) | | **Gonioscopic Angle** | Open, trabecular meshwork visible | Closed, iris touches angle wall | | **Onset** | Insidious, asymptomatic | Acute (pain, redness) or chronic (asymptomatic) | | **Visual Field** | Arcuate, paracentral, nasal step | Variable; may be arcuate in chronic form | | **Optic Disc** | Vertical cup elongation | Variable cupping | | **Iris Bombé** | Absent | Present in acute pupillary block | | **Cornea** | Clear | Hazy/edematous in acute attack | ### Mnemonic for Angle Classification **SHALLOW = CLOSED; WIDE = OPEN** - **S**hallow anterior chamber → angle closure risk - **W**ide anterior chamber → open-angle disease ### Clinical Pearl Gonioscopy is essential for angle assessment, but it is **qualitative and operator-dependent**. Quantitative measurement of anterior chamber depth (by A-scan, optical biometry, or AS-OCT) provides **objective, reproducible data** that definitively characterizes the angle anatomy and distinguishes the two glaucoma types. ### High-Yield Summary **Anterior chamber depth >2.5 mm effectively rules out angle-closure glaucoma as the primary mechanism**, because angle closure requires a structurally shallow anterior segment. This measurement is the most direct, objective, and clinically useful discriminator between the two pathophysiological types. [cite:Khurana 7e Ch 8] 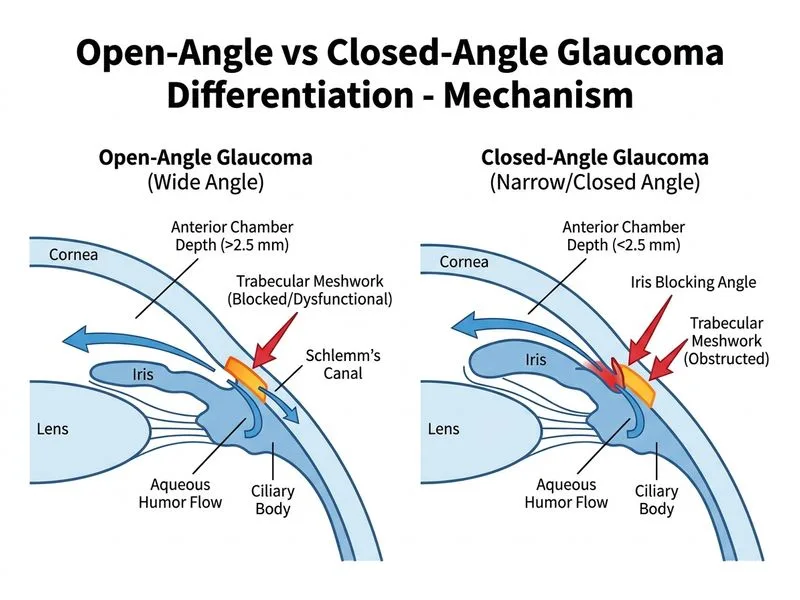
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.