## Prognostic Factors in Oral Cavity Carcinoma **Key Point:** Depth of invasion (tumor thickness) and perineural invasion (PNI) are the strongest independent prognostic factors in oral squamous cell carcinoma, more predictive than TNM stage alone. ### Why Depth of Invasion Matters Tumor thickness (depth of invasion from the surface epithelium to the deepest point of invasion) is a critical determinant of: - Risk of cervical lymph node metastasis - Overall survival and disease-free survival - Local recurrence rates **High-Yield:** Tumors >4 mm depth have significantly worse prognosis compared to those ≤4 mm, with 5-year survival rates dropping from ~80% to <50%. ### Perineural Invasion (PNI) **Clinical Pearl:** PNI is present in 20–40% of oral cavity cancers and is associated with: - Increased risk of cervical nodal metastasis (even in clinically N0 necks) - Higher rates of local and regional recurrence - Worse overall survival independent of stage - Potential for skip lesions along nerve pathways ### Comparative Significance of Other Factors | Factor | Prognostic Value | Notes | | --- | --- | --- | | Depth of invasion & PNI | **Very High** | Independent predictors of survival | | Histological grade | Moderate | Less predictive than depth/PNI | | Tumor size (T stage) | Moderate | Important but less than depth | | Patient age | Low | Not a primary determinant | | Duration of symptoms | Low | Reflects patient delay, not biology | **Warning:** Many clinicians focus on TNM staging, but depth of invasion and PNI often provide better risk stratification and guide adjuvant therapy decisions (e.g., need for neck dissection in N0 disease with PNI). ### Clinical Implications In this case, the presence of a 2 cm lesion with indurated margins and floor of mouth involvement suggests significant depth. If PNI is confirmed on histology, this patient would require: - Elective neck dissection (even if clinically N0) - Consideration of adjuvant radiotherapy or chemoradiotherapy - Closer surveillance for recurrence [cite:Harrison 21e Ch 82] 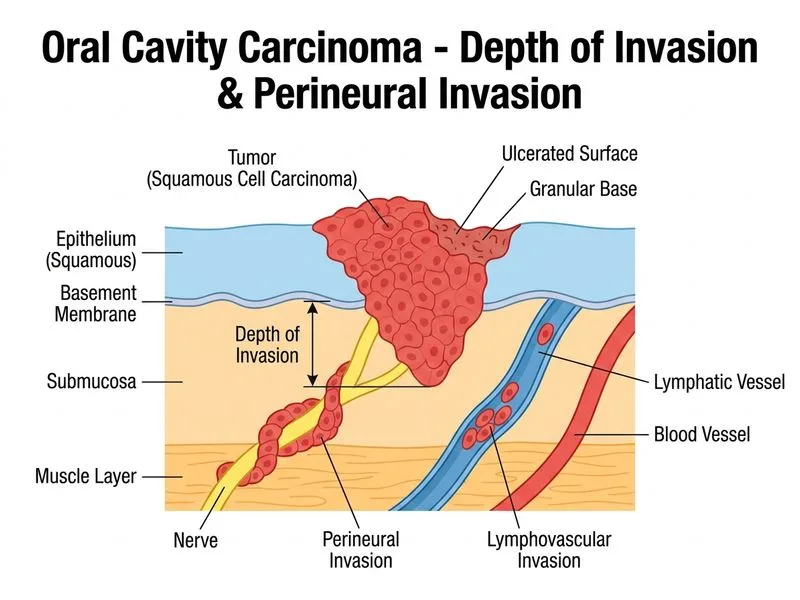
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.