## Management of Hard Palate Carcinoma with Bone Invasion ### Tumor Characteristics & Staging - **Tumor size:** 3.5 cm (T2 lesion) - **Bone invasion:** Indicates **T4a disease** (tumor invading cortical bone of maxilla) - **Regional nodes:** N0 (no cervical lymphadenopathy) - **Overall stage:** T4aN0M0 = **Stage IVA** ### Surgical Considerations **Key Point:** Invasion into maxillary bone mandates **partial or total maxillectomy** rather than simple wide local excision. The bone cannot be adequately cleared by soft tissue surgery alone. **Clinical Pearl:** Hard palate carcinomas have a higher propensity for bone invasion due to the thin mucosa overlying bone. MRI confirmation of bone involvement is the gold standard for surgical planning. ### Treatment Algorithm ```mermaid flowchart TD A[Hard palate SCC with bone invasion]:::outcome --> B{T4a disease?}:::decision B -->|Yes| C[Partial/Total Maxillectomy]:::action C --> D[Reconstruction with flap]:::action D --> E[Adjuvant radiotherapy ± chemotherapy]:::action E --> F[Improved locoregional control]:::outcome B -->|No bone invasion| G[Wide local excision]:::action G --> H[Consider adjuvant RT if high-risk features]:::action ``` ### Why This Option is Correct 1. **Maxillectomy is mandatory** for T4a disease (bone invasion) 2. **Reconstruction** prevents oro-antral fistula and maintains function 3. **Adjuvant radiotherapy** improves locoregional control in Stage IVA disease **High-Yield:** T4a tumors (bone invasion) require surgery + adjuvant RT. T4b tumors (skull base, carotid artery involvement) are often unresectable and treated with concurrent chemoradiotherapy. ### Mnemonic: MAXILLA Invasion Protocol - **M**axillectomy (partial or total) - **A**djuvant radiotherapy - **X**-ray/MRI for staging - **I**nvasion assessment (cortical vs. trabecular) - **L**ocal flap reconstruction - **L**ocoregional control (goal) - **A**ssess for complications (fistula, speech, swallowing) 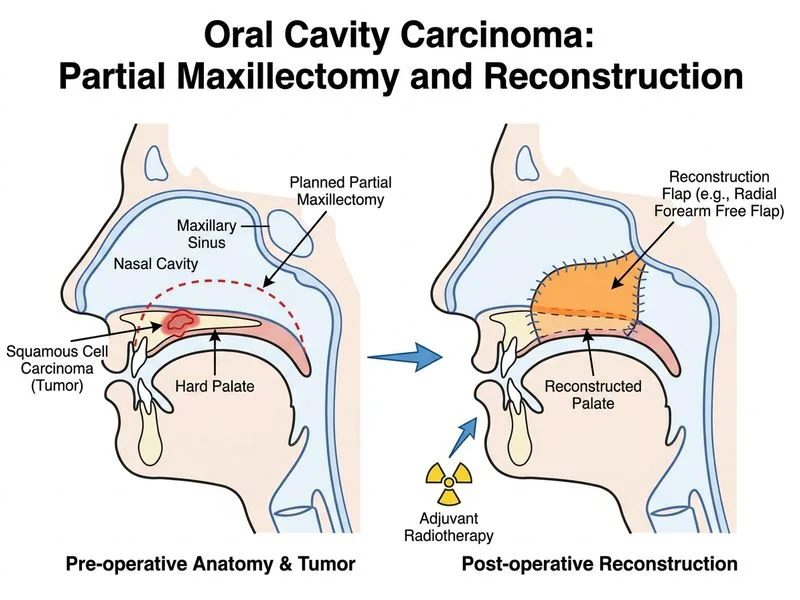
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.