## Prognostic Factors in Oral Cavity Carcinoma **Key Point:** Depth of invasion (tumor thickness) and perineural invasion are the most significant independent prognostic factors in oral squamous cell carcinoma, more predictive than TNM stage alone. ### Why Depth of Invasion Matters **High-Yield:** Tumors with depth of invasion >4 mm have significantly worse prognosis, with increased risk of: - Cervical lymph node metastasis - Distant metastasis - Local recurrence - Reduced 5-year survival ### Perineural Invasion (PNI) **Clinical Pearl:** Presence of PNI indicates aggressive tumor biology and is an independent predictor of: - Higher recurrence rates - Worse overall survival - Need for adjuvant therapy even in early-stage tumors ### Prognostic Factor Hierarchy | Factor | Prognostic Impact | Evidence Level | |--------|------------------|----------------| | Depth of invasion (>4 mm) | Very High | Strong | | Perineural invasion | Very High | Strong | | Lymph node involvement | High | Strong | | Tumor size (T stage) | Moderate | Moderate | | Smoking/betel history | Low (risk factor, not prognostic) | Weak | | Grade of differentiation | Moderate | Moderate | **Warning:** Do not confuse *risk factors* (smoking, betel nut) with *prognostic factors*. Risk factors determine who develops cancer; prognostic factors predict outcome once cancer is present. ### Clinical Implications Patients with depth >4 mm or PNI require: - Wider surgical margins (≥5 mm) - Elective neck dissection even if N0 - Adjuvant radiotherapy ± chemotherapy - Closer follow-up surveillance [cite:Robbins 10e Ch 9] 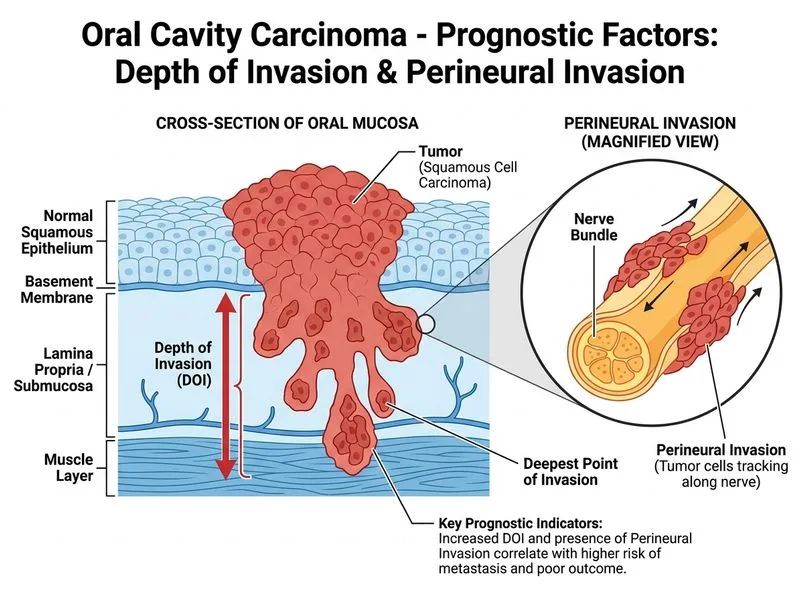
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.