## Prognostic Factors in Oral Cavity Carcinoma ### Depth of Invasion as the Primary Prognostic Factor **Key Point:** Depth of invasion (tumor thickness) is the single most important independent prognostic factor in oral cavity squamous cell carcinoma, more predictive than TNM stage alone. **High-Yield:** Tumors with depth of invasion >4 mm have significantly worse prognosis and higher rates of cervical lymph node metastasis (up to 40%) compared to tumors <4 mm (5–10% metastasis rate). **Clinical Pearl:** Even early-stage (T1–T2) oral cavity cancers with depth >4 mm warrant elective neck dissection due to occult nodal disease risk, whereas superficial tumors may be managed with observation alone. ### Comparison of Prognostic Factors in Oral Cavity Carcinoma | Factor | Impact on Prognosis | Evidence Level | |--------|-------------------|----------------| | **Depth of invasion (>4 mm)** | Most significant; predicts nodal metastasis | Very strong | | Tumor location | Moderate; posterior sites (soft palate, base of tongue) worse | Moderate | | Histologic grade | Moderate; poor differentiation = worse outcome | Moderate | | Lymph node status | Critical for staging; N0 vs N+ changes management | Very strong | | Perineural invasion | Indicates aggressive biology; worsens prognosis | Strong | | Patient age | Minor; age >60 associated with worse outcomes | Weak | | Margin status | Important for recurrence risk | Strong | **Mnemonic:** **DEPTH** — Depth of invasion, Early detection, Perineural invasion, Tumor location, Histologic grade ### Why Depth of Invasion Matters 1. **Occult nodal disease:** Depth >4 mm correlates with 40% risk of cervical lymph node involvement even in clinically N0 neck. 2. **Treatment implications:** Guides decision for elective neck dissection vs. observation. 3. **Survival impact:** 5-year survival drops from ~80% (depth <4 mm) to ~50% (depth >4 mm). 4. **Independent predictor:** Remains significant even after controlling for TNM stage. **Warning:** Do not confuse depth of invasion with T-stage (which is based on tumor size). A small T1 tumor with depth >4 mm has worse prognosis than a larger T2 tumor with depth <3 mm. 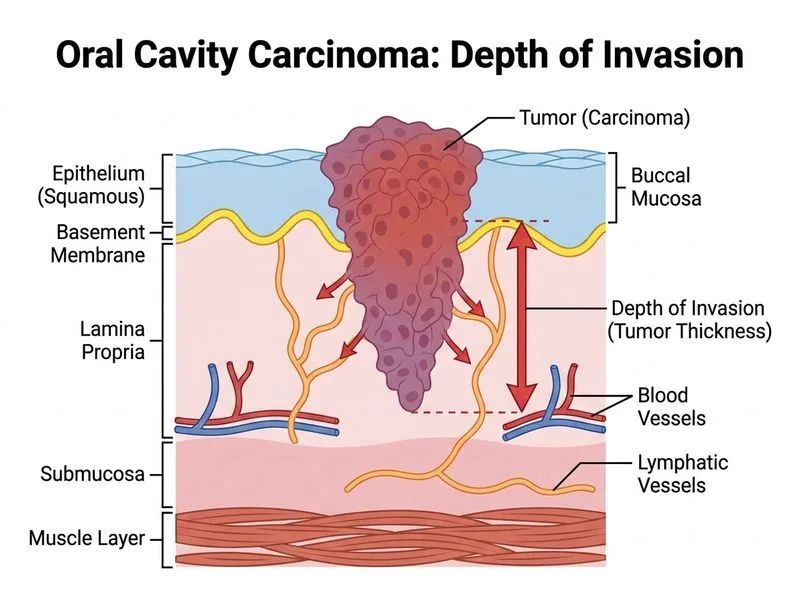
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.