## Clinical Presentation Analysis The patient presents with classic features of oral cavity carcinoma: - Non-healing ulcer persisting >3 weeks - Indurated base with rolled edges (pathognomonic for malignancy) - Granular appearance - Regional lymphadenopathy ## Diagnostic Approach **Key Point:** Any persistent oral ulcer with indurated edges and regional lymphadenopathy must be considered malignant until proven otherwise. Tissue diagnosis is mandatory before any treatment. **High-Yield:** Incision biopsy (not excision biopsy) is the gold standard for suspected oral malignancy because: 1. Provides adequate tissue for histopathological diagnosis 2. Avoids tumor spillage that may occur with excision biopsy 3. Allows assessment of depth of invasion and differentiation grade 4. Guides staging and treatment planning ## Why Incision Biopsy is Correct | Step | Rationale | |------|----------| | **Incision biopsy** | Confirms diagnosis, assesses grade/depth; essential before any treatment | | Timing | Should be done within 1–2 weeks of suspicion | | Site | Multiple sites from ulcer margin and base to avoid necrotic center | **Clinical Pearl:** The rolled edges and indurated base are hallmarks of squamous cell carcinoma (SCC), the most common oral malignancy (>90% of cases). Biopsy confirmation is non-negotiable before staging investigations or treatment. ## Staging After Biopsy Confirmation Once histology confirms malignancy: 1. **Local staging:** CT/MRI of oral cavity and neck 2. **Regional staging:** Neck dissection assessment based on imaging and clinical findings 3. **Distant staging:** Chest X-ray or CT chest to exclude pulmonary metastases 4. **Treatment planning:** Surgery (wide local excision ± neck dissection) ± adjuvant radiotherapy/chemotherapy based on TNM stage **Mnemonic: BIOPSY FIRST** — Before Investigation Or Planned Surgery, Yield Specific diagnosis 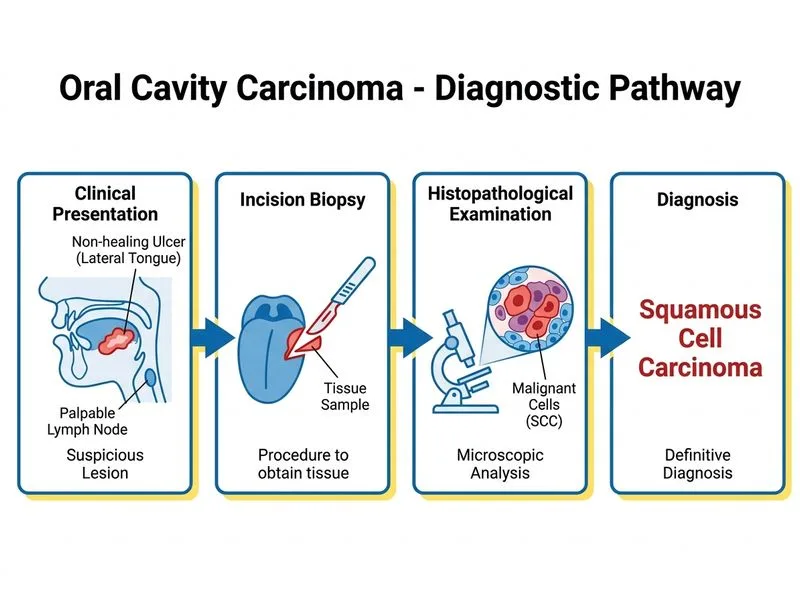
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.