## Clinical Diagnosis: Preseptal Cellulitis **Key Point:** This patient has preseptal (anterior to orbital septum) cellulitis, NOT orbital cellulitis. The absence of ophthalmoplegia, normal fundoscopy, and preserved vision are the critical distinguishing features. ### Differential Diagnosis: Preseptal vs. Orbital Cellulitis | Feature | Preseptal Cellulitis | Orbital Cellulitis | |---------|----------------------|--------------------| | **Location** | Anterior to orbital septum (eyelid) | Deep orbital tissues | | **Eye movements** | Full and painless | Restricted, painful (ophthalmoplegia) | | **Proptosis** | Absent or minimal | Marked | | **Disc edema** | Absent | Present (late sign) | | **Visual acuity** | Normal | Reduced (optic neuropathy) | | **Chemosis** | Mild | Marked | | **Systemic toxicity** | Mild to moderate | Severe (high fever, malaise) | | **Imaging** | Lid swelling, anterior fat stranding | Diffuse orbital infiltration, possible abscess | | **Source** | Skin infection, insect bite, minor trauma | Sinusitis (especially ethmoid), dental, hematogenous | | **Management** | Oral antibiotics, outpatient follow-up | IV antibiotics, hospitalization | **High-Yield:** The **orbital septum** is the anatomical boundary. Preseptal = eyelid problem; orbital = deep space emergency. ### Why This Patient Has Preseptal Cellulitis 1. **Full eye movements** — ophthalmoplegia is the hallmark of orbital involvement; this patient has none. 2. **Normal fundoscopy** — no disc edema or retinal changes; orbital inflammation would compress the optic nerve. 3. **Preserved vision (6/6)** — orbital cellulitis causes vision loss from optic neuropathy or retinal ischemia. 4. **Mild proptosis** — preseptal swelling can cause apparent proptosis; true orbital proptosis is marked and accompanied by ophthalmoplegia. 5. **CT findings** — mild fat stranding around medial rectus (likely from adjacent ethmoid sinusitis) without deep orbital abscess or diffuse infiltration. ### Management Algorithm ```mermaid flowchart TD A[Eyelid swelling + fever]:::outcome --> B{Eye movements normal?}:::decision B -->|Yes| C[Preseptal cellulitis]:::outcome B -->|No| D[Orbital cellulitis]:::outcome C --> E{Systemic toxicity?}:::decision E -->|Mild-moderate| F[Oral antibiotics, outpatient]:::action E -->|Severe| G[IV antibiotics, admit]:::action D --> H[IV ceftriaxone + vancomycin, admit]:::urgent F --> I[Amoxicillin-clavulanate or cephalexin PO]:::action I --> J[Follow-up in 48 hours]:::action J --> K{Improving?}:::decision K -->|Yes| L[Continue oral antibiotics 7-10 days]:::action K -->|No| M[Repeat imaging, escalate to IV]:::urgent ``` **Clinical Pearl:** Preseptal cellulitis is often self-limited and responds well to oral antibiotics. However, if there is no improvement after 48 hours, or if systemic toxicity worsens, escalate to IV therapy and imaging to exclude orbital extension. **Antibiotic Choice for Preseptal Cellulitis:** - **First-line:** Amoxicillin-clavulanate 500/125 mg TDS (or cephalexin 500 mg QID) - **Rationale:** Covers common skin pathogens (*S. aureus*, *S. pyogenes*, *H. influenzae*) - **Duration:** 7–10 days - **Follow-up:** Clinical review at 48 hours; if worsening, switch to IV and obtain imaging **Why NOT Option 4 (Corticosteroids)?** Orbital pseudotumor (idiopathic orbital inflammation) presents with: - Insidious onset (weeks to months), not acute (3 days) - Often unilateral eye pain + proptosis, but usually NO fever - Responds dramatically to corticosteroids - Diagnosis of exclusion after ruling out infection This patient has fever and recent URTI → infectious etiology is most likely. Steroids would be contraindicated without ruling out infection first. **Tip:** Always check eye movements first. If they are full and painless, you are dealing with preseptal disease — a much more benign condition manageable in the outpatient setting. [cite:Khurana Ophthalmology Ch 12] 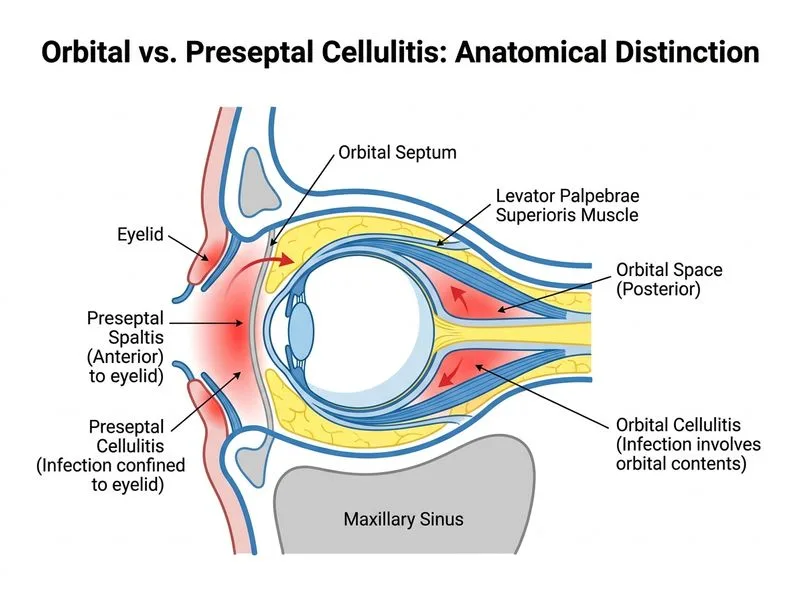
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.