## Pralidoxime (2-PAM) as an Oxime Reactivator **Key Point:** Pralidoxime is an oxime that reactivates phosphorylated acetylcholinesterase by nucleophilic attack on the phosphorus atom, but only if given **before "aging"** occurs (typically within 24–48 hours, depending on the agent). ### Mechanism of Pralidoxime 1. Oximes penetrate the blood-brain barrier poorly but reach peripheral sites effectively 2. They break the phosphorus-enzyme bond and restore AChE activity 3. Efficacy depends on timing — once the phosphate-enzyme complex "ages" (loses an alkyl group), reactivation is impossible 4. Most effective for nicotinic manifestations; less effective for muscarinic signs ### Comparison of Antidotes in Organophosphate Poisoning | Antidote | Mechanism | Onset | Efficacy | Notes | |----------|-----------|-------|----------|-------| | **Pralidoxime (2-PAM)** | Reactivates AChE | 5–15 min | High if early | Ineffective after aging | | **Atropine** | Muscarinic antagonist | Rapid | Muscarinic signs only | Does not reactivate enzyme | | **Physostigmine** | AChE inhibitor | Rapid | Worsens toxicity | Contraindicated | | **Neostigmine** | AChE inhibitor | Rapid | Worsens toxicity | Contraindicated | **High-Yield:** The combination of **atropine + pralidoxime** is the standard treatment: atropine for immediate symptomatic relief, pralidoxime for enzyme reactivation. **Clinical Pearl:** Pralidoxime is most effective for nicotinic symptoms (fasciculations, paralysis) and less effective for muscarinic symptoms (miosis, bronchospasm), which respond better to atropine. 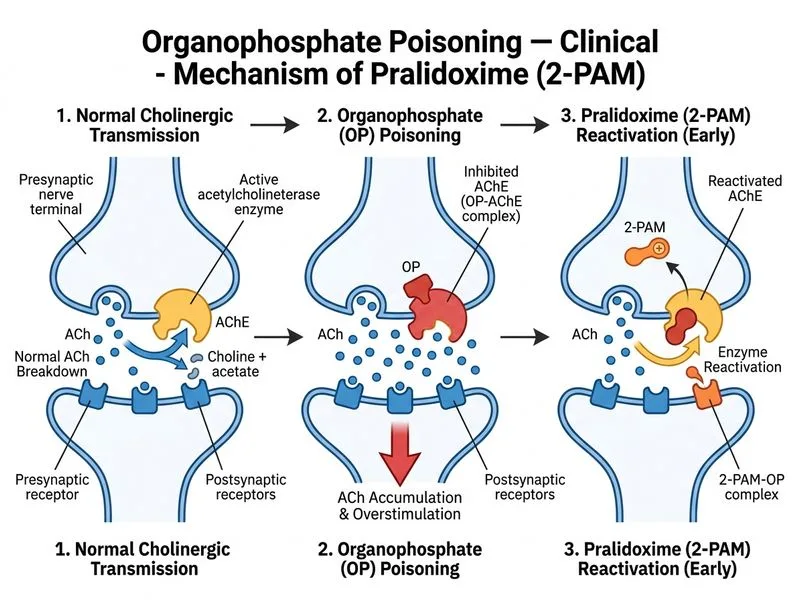
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.