## Nicotinic Phase Management in Organophosphate Poisoning ### Clinical Context: Nicotinic vs. Muscarinic Toxicity The patient has progressed to the **nicotinic phase** of organophosphate poisoning, characterized by: - Paralysis and weakness (nicotinic effect at neuromuscular junction) - Fasciculations (visible muscle twitching from uncontrolled ACh release) - Respiratory muscle paralysis requiring mechanical ventilation Muscarinic effects (bronchospasm, bradycardia) have been controlled with atropine and pralidoxime. **Key Point:** Nicotinic toxicity (paralysis) is reversed by pralidoxime reactivating acetylcholinesterase at the neuromuscular junction. This process takes time — continued pralidoxime infusion and supportive care are the standard approach. ### Why NOT Succinylcholine? | Aspect | Succinylcholine | Rocuronium | Pralidoxime + Time | |--------|-----------------|-----------|-------------------| | **Mechanism** | Depolarizing agent; mimics ACh | Non-depolarizing blocker | Reactivates AChE | | **In OP poisoning** | **CONTRAINDICATED** — causes prolonged apnea | **CONTRAINDICATED** — unpredictable metabolism | **INDICATED** | | **Why risky** | Cholinesterase is inhibited; succinylcholine cannot be metabolized → prolonged paralysis (hours to days) | Rocuronium is metabolized by Hofmann elimination; unpredictable in OP poisoning; may prolong paralysis | Restores normal neuromuscular transmission | | **Outcome** | Patient may remain paralyzed for 24–48 hrs despite reversal of OP toxicity | Unpredictable duration; risk of prolonged paralysis | Gradual recovery as AChE is reactivated | **Clinical Pearl:** Succinylcholine is absolutely contraindicated in organophosphate poisoning because the patient's pseudocholinesterase (plasma cholinesterase) is already inhibited by the organophosphate. Succinylcholine cannot be metabolized and causes **prolonged apnea** — the patient may remain paralyzed for 24–48 hours even after the organophosphate is cleared. ### Correct Management of Nicotinic Phase 1. **Continue pralidoxime infusion:** 0.5–1 g/hour IV (or repeat boluses 1 g every 4–6 hours) - Reactivates acetylcholinesterase at nicotinic sites - Restores neuromuscular transmission - Most effective if given early (within 24–48 hours before "aging" of the enzyme–organophosphate complex) 2. **Maintain mechanical ventilation** with sedation and analgesia (use agents that do NOT depend on pseudocholinesterase metabolism, e.g., propofol, midazolam, remifentanil) 3. **Await spontaneous recovery** of neuromuscular function as pralidoxime reactivates AChE - Recovery may take hours to days depending on the organophosphate and time to treatment - Serial assessment of neuromuscular function (train-of-four, head lift test) guides weaning 4. **Supportive care:** Maintain airway, oxygenation, and hemodynamic stability **High-Yield:** The phrase "unable to lift his head off the bed despite adequate sedation reversal" indicates **true neuromuscular paralysis** (nicotinic effect), not sedation. This is reversed by pralidoxime, not by additional neuromuscular blockers. ### Why Tracheostomy Is Not Indicated The patient is already intubated and stable on mechanical ventilation. Tracheostomy is considered only if prolonged ventilation (>7–10 days) is anticipated, which is not the case here with appropriate pralidoxime therapy. [cite:Harrison 21e Ch 473; Poisoning and Drug Overdose (Olson) Ch 10] 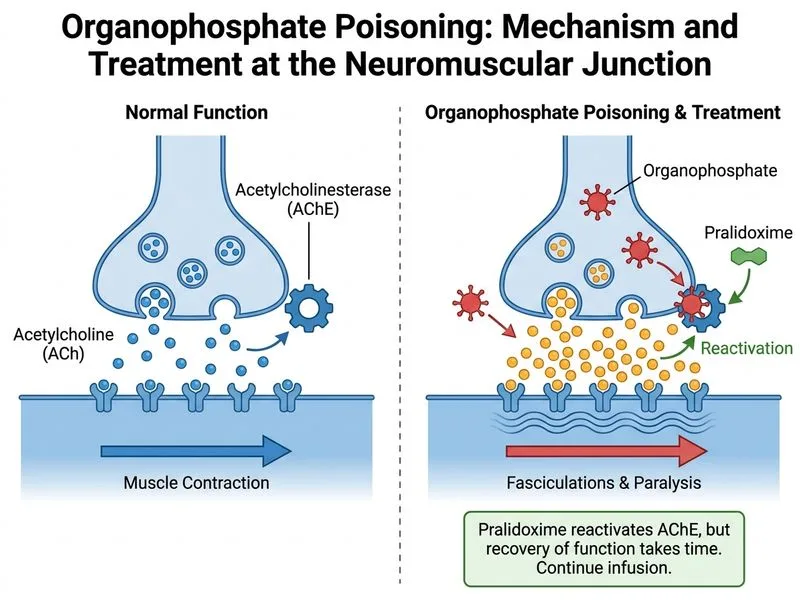
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.