## Diagnosis of Organophosphate Poisoning ### Specific Confirmatory Investigation **Key Point:** Serum cholinesterase (pseudocholinesterase/butyrylcholinesterase) activity is the gold standard and most specific investigation for organophosphate poisoning. Organophosphates irreversibly inhibit acetylcholinesterase and pseudocholinesterase, causing accumulation of acetylcholine. ### Interpretation of Cholinesterase Levels | Cholinesterase Activity | Clinical Correlation | |---|---| | > 75% of baseline | Minimal or no symptoms | | 50–75% of baseline | Mild symptoms | | 25–50% of baseline | Moderate symptoms | | < 25% of baseline | Severe poisoning | **High-Yield:** A reduction of >50% from baseline (or normal reference range) is diagnostic of organophosphate or carbamate poisoning. Serial measurements show progressive decline and later recovery, tracking clinical severity. ### Why Serum Cholinesterase? 1. **Specificity:** Directly reflects the mechanism of organophosphate toxicity (acetylcholinesterase inhibition). 2. **Quantifiable:** Provides a numerical value that correlates with severity. 3. **Prognostic:** Serial measurements guide duration of antidote therapy and predict recovery. 4. **Differentiates from other causes:** Cholinergic toxidromes from other causes (e.g., carbamates, nerve agents) show similar patterns but organophosphates cause irreversible inhibition. **Clinical Pearl:** Red blood cell (RBC) cholinesterase is more specific for acetylcholinesterase inhibition than plasma cholinesterase, but plasma cholinesterase is more readily available and sufficient for clinical diagnosis. ### Supportive Investigations - **ABG:** Shows hypoxemia and hypercarbia due to bronchospasm and respiratory muscle paralysis; not specific. - **ECG:** May show bradycardia, prolonged QT, ST changes; nonspecific findings. - **Electrolytes/renal function:** Assess secondary complications; not diagnostic. 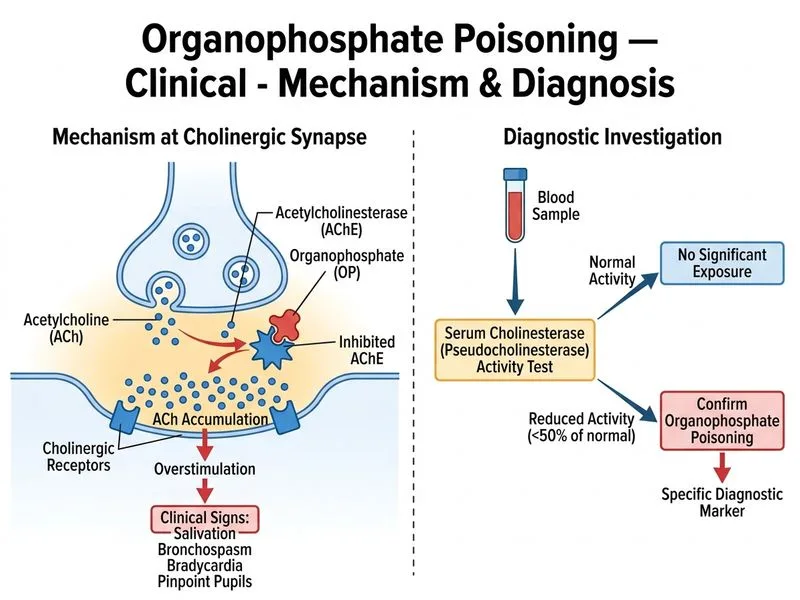
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.