## Clinical Context This patient has severe acute organophosphate poisoning with classic **muscarinic and nicotinic signs**: miosis, hypersalivation, bronchospasm, bradycardia, and muscle fasciculations. The respiratory acidosis (elevated PaCO₂) reflects ventilatory compromise from bronchospasm and muscle weakness. ## Immediate Management Priority **Key Point:** Atropine is the first-line antidote in organophosphate poisoning and must be given immediately, even before pralidoxime or airway management, to reverse life-threatening muscarinic effects. ### Why Atropine First? 1. **Muscarinic blockade** — Atropine antagonizes acetylcholine at muscarinic receptors, rapidly reversing: - Bronchospasm and bronchorrhea (allows better ventilation) - Bradycardia (improves cardiac output) - Miosis (restores vision) - Salivation and lacrimation 2. **Dose titration** — Start 2–5 mg IV and repeat every 5–10 minutes until signs of atropinization appear: - Dry mouth - Dilated pupils - Increased heart rate - Cessation of bronchospasm 3. **Timing** — Atropine works within seconds; pralidoxime (which addresses nicotinic effects) takes 30–40 minutes to reactivate acetylcholinesterase. ## Why This Patient Needs Atropine Now - Bronchospasm + hypersalivation → airway compromise - Bradycardia → reduced cerebral perfusion - Atropine will improve oxygenation and ventilation *before* intubation becomes necessary **Clinical Pearl:** Large doses of atropine (100+ mg/day) may be needed in severe poisoning; do not be afraid to escalate. The endpoint is clinical drying, not a fixed dose. **High-Yield:** Atropine does NOT reverse nicotinic effects (muscle weakness, fasciculations, paralysis) — that is why pralidoxime (oxime) is given *after* atropine to reactivate acetylcholinesterase and restore nicotinic function. 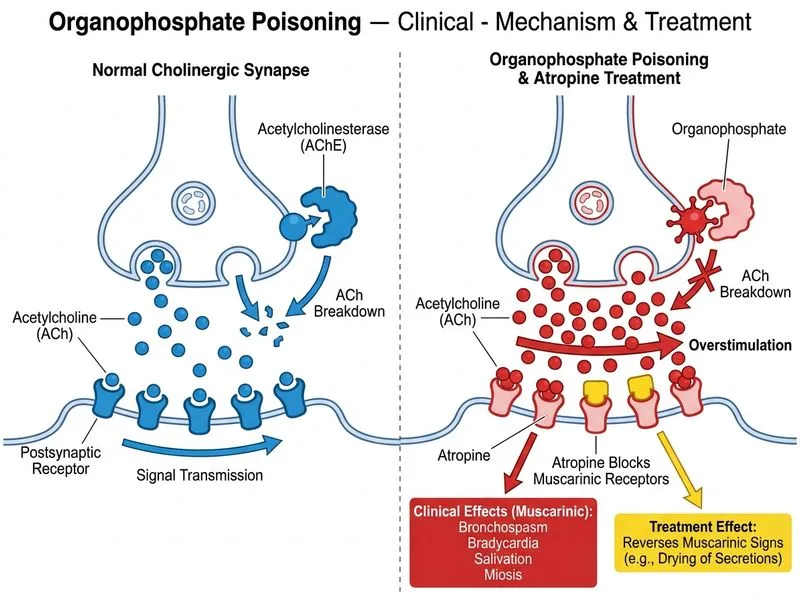
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.