## Distinguishing Acute Cholinergic Crisis from Intermediate Syndrome ### Timeline and Pathophysiology **Key Point:** The acute cholinergic phase (0–12 hours post-exposure) is defined by massive acetylcholine accumulation at both muscarinic and nicotinic synapses. The intermediate syndrome (24–96 hours) emerges after partial resolution of cholinergic excess and involves a distinct neuromuscular junction dysfunction. ### Clinical Comparison Table | Feature | Acute Cholinergic Phase | Intermediate Syndrome | |---------|------------------------|----------------------| | **Onset** | 0–12 hours | 24–96 hours | | **Miosis** | Present (prominent) | Absent or minimal | | **Fasciculations** | Present (nicotinic) | Absent or minimal | | **Salivation/Bronchorrhea** | Prominent | Largely resolved | | **Acetylcholinesterase Activity** | Severely depressed | Normal or near-normal | | **Respiratory Weakness** | Bronchospasm + CNS depression | True proximal/respiratory muscle paralysis | | **Response to Atropine** | Excellent | Poor | ### Why Option C is the Best Discriminator **High-Yield:** The question asks which feature **best distinguishes the acute cholinergic phase** from the intermediate syndrome. Muscle fasciculations (nicotinic receptor overstimulation) and miosis (muscarinic receptor overstimulation) are hallmark signs of the **acute cholinergic phase** and are characteristically **absent** in the intermediate syndrome. Their presence therefore reliably identifies the acute phase and distinguishes it from the intermediate syndrome. **Clinical Pearl:** The colleague presenting 6 hours later with dilated pupils, dry mouth, and no fasciculations illustrates the transition away from acute cholinergic excess — the very features that define the intermediate syndrome's clinical picture. The presence of miosis + fasciculations = acute phase; their absence = intermediate syndrome or recovery. ### Why Option B is Incorrect as the Best Discriminator Option B (respiratory muscle weakness with normal/elevated acetylcholinesterase) describes a feature of the **intermediate syndrome**, not a feature that distinguishes the **acute cholinergic phase** from it. The question stem asks which feature best distinguishes the acute cholinergic phase — meaning a feature characteristic of the acute phase that is absent in the intermediate syndrome. Option C (fasciculations and miosis) directly fulfills this criterion. ### Why Other Options Fail - **Option A (Nicotinic over muscarinic predominance):** Both phases involve both receptor types; this framing is inaccurate and tangential. - **Option B (Respiratory weakness with normal AChE):** This characterizes the intermediate syndrome, not the acute phase. - **Option D (Absent pupillary response to light):** Too vague and non-specific; not a reliable discriminator between the two phases. [cite:Harrison 21e Ch 475; KD Tripathi Essentials of Medical Pharmacology 8e, Organophosphate Poisoning] 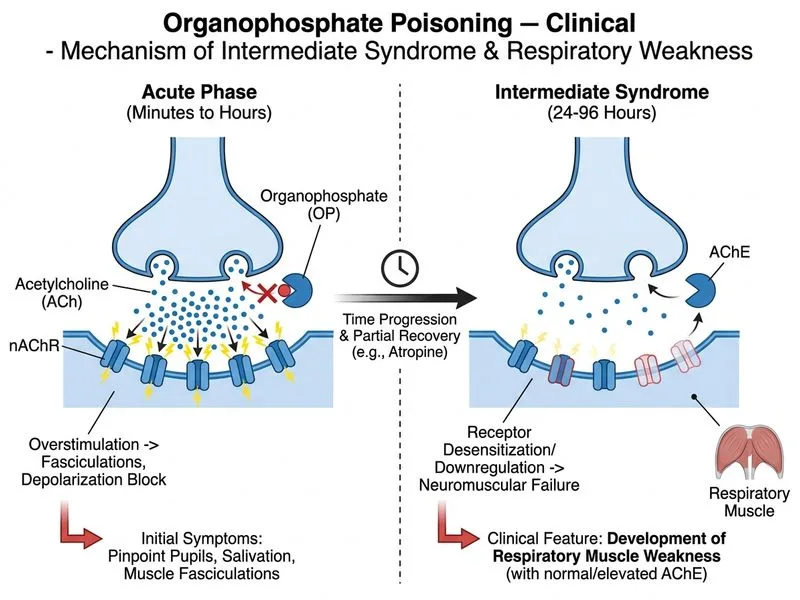
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.