## Pralidoxime (2-PAM) — Second-Line Therapy After Atropine Stabilization ### Clinical Context: Nicotinic vs. Muscarinic Manifestations Organophosphates cause toxicity at **both muscarinic and nicotinic receptors**: | Receptor Type | Manifestations | Agent | Timeline | |---------------|----------------|-------|----------| | **Muscarinic** | Bronchospasm, bradycardia, salivation, miosis, diarrhea | Atropine | Immediate relief | | **Nicotinic** | Muscle weakness, fasciculations, paralysis, respiratory failure | Pralidoxime (2-PAM) | Effective if <24–48 hrs | **Key Point:** In this patient, atropine has successfully reversed **muscarinic** signs (bronchospasm improved, HR normalized). However, **nicotinic** manifestations (muscle weakness, fasciculations, inability to stand) persist — these require pralidoxime. ### Why Pralidoxime Now? **High-Yield:** Pralidoxime is a nucleophilic oxime that **reactivates acetylcholinesterase** by removing the phosphoryl group from the enzyme's active site. This restores the enzyme's ability to hydrolyze acetylcholine at the neuromuscular junction. 1. **Timing is critical:** 2-PAM is most effective within 6 hours (ideally <2 hours), but can help up to 24–48 hours post-exposure. 2. **This patient is at 2 hours** — well within the therapeutic window. 3. **Nicotinic crisis is life-threatening:** Persistent muscle weakness can progress to respiratory failure if not reversed. ### Pralidoxime Dosing **Standard regimen:** - **Loading dose:** 1 g IV over 5–30 minutes - **Maintenance:** Continuous infusion of 200–500 mg/hour, OR repeat boluses of 1 g every 4–6 hours - **Duration:** Continue until signs of reactivation appear (improved muscle strength, resolution of fasciculations) or until 24–48 hours have elapsed **Clinical Pearl:** Pralidoxime must be given concurrently with atropine — it does NOT replace atropine. The combination addresses both muscarinic and nicotinic toxicity. ### Mechanism: Why Pralidoxime Works ```mermaid flowchart TD A[Organophosphate binds AChE]:::outcome --> B[Phosphorylation of serine residue]:::outcome B --> C{Time elapsed?}:::decision C -->|< 24-48 hrs: Phosphorylated AChE<br/>can be reactivated| D[Pralidoxime oxime group<br/>attacks phosphorus]:::action C -->|> 48 hrs: Aged complex<br/>irreversible| E[No reactivation possible]:::urgent D --> F[Phosphorus removed,<br/>AChE regenerated]:::outcome F --> G[ACh hydrolysis restored,<br/>neuromuscular function returns]:::outcome ``` **Mnemonic:** **2-PAM = "Too late After aging" (if >48 hrs) vs. **"Perfect if Prompt" (if <24 hrs)** ### Why NOT the Other Options? - **Repeat atropine:** The patient is already atropinized (HR 78, alert, bronchospasm resolved). Further atropine will not reverse nicotinic weakness — it only blocks muscarinic receptors. Overdosing atropine causes tachycardia, confusion, and anticholinergic toxicity. - **Plasma exchange:** Pseudocholinesterase is an enzyme; its low activity reflects organophosphate binding, not a deficiency that plasma exchange can correct. Plasma exchange does not reactivate the enzyme and wastes critical time. (Note: Pseudocholinesterase variants can predispose to prolonged succinylcholine apnea, but this is not the issue here.) - **Succinylcholine:** This is **absolutely contraindicated**. Succinylcholine is a depolarizing neuromuscular blocker that causes fasciculations and paralysis — it will WORSEN the patient's nicotinic crisis and cause respiratory failure. The patient already has uncontrolled acetylcholine at the neuromuscular junction; adding a cholinergic agent is dangerous. **Warning:** A common trap is confusing pseudocholinesterase deficiency (which affects drug metabolism, not toxin management) with the need for plasma exchange. Plasma exchange does not help organophosphate poisoning. ### Summary: Atropine → Pralidoxime Sequence **High-Yield:** The classic teaching is: 1. **Atropine first** → reverses muscarinic crisis (airway, breathing, circulation) 2. **Pralidoxime second** → reverses nicotinic crisis (muscle weakness, paralysis) 3. Both given together in moderate-to-severe poisoning 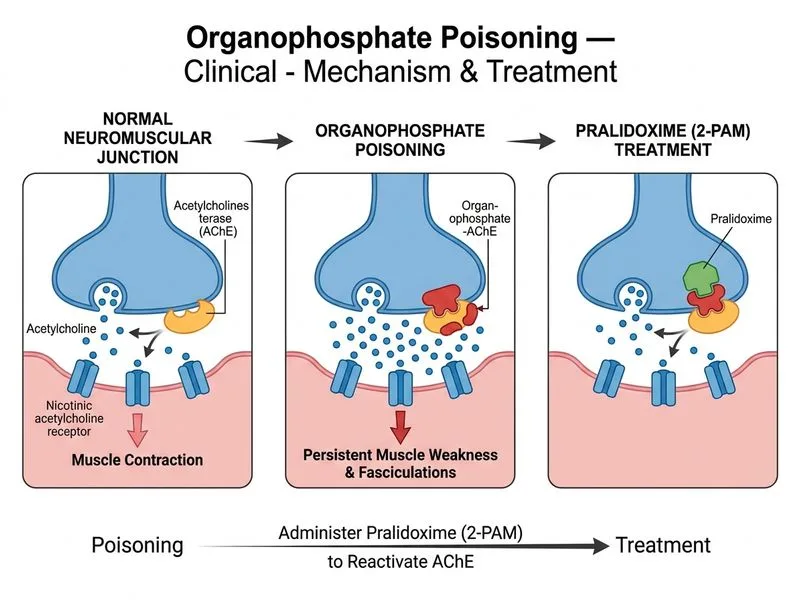
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.