## Immediate Management of Organophosphate Poisoning **Key Point:** Organophosphate poisoning causes irreversible inhibition of acetylcholinesterase, leading to accumulation of acetylcholine at cholinergic synapses. The clinical presentation reflects both muscarinic and nicotinic overstimulation. ### Clinical Presentation in This Case The patient exhibits classic **SLUDGE** (Salivation, Lacrimation, Urination, Defecation, GI upset, Emesis) plus nicotinic signs: - **Muscarinic signs:** pinpoint pupils, salivation, bronchospasm, bradycardia, hypertension (early phase) - **Nicotinic signs:** tremor, muscle fasciculations, weakness - **Respiratory compromise:** bronchospasm + pulmonary edema → hypoxemia and hypercapnia ### Treatment Algorithm ```mermaid flowchart TD A[Organophosphate Poisoning Confirmed]:::outcome --> B[Decontamination + Airway Management]:::action B --> C{Muscarinic Signs Present?}:::decision C -->|Yes| D[Atropine 5 mg IV bolus]:::action D --> E{Signs of Atropinization?}:::decision E -->|No| F[Repeat atropine 2-5 mg IV every 5-10 min]:::action E -->|Yes| G[Switch to maintenance infusion]:::action F --> H[Pralidoxime 1 g IV]:::action G --> H H --> I[Supportive care: O₂, ventilation, seizure prophylaxis]:::action I --> J[Monitor for recrudescence]:::outcome ``` ### Why Atropine First? 1. **Immediate life threat:** Bronchospasm + pulmonary edema + bradycardia require urgent muscarinic blockade 2. **Dosing:** Initial bolus of **5 mg IV**, then **2–5 mg every 5–10 minutes** until: - Pupils dilate - Salivation/bronchial secretions dry up - Heart rate increases to >80/min - This is called "atropinization" 3. **Pralidoxime timing:** Given **after** or **concurrent with** atropine (not before) - Pralidoxime reactivates acetylcholinesterase if given early (ideally within 24–48 hours, but efficacy decreases with time) - Dose: 1 g IV over 15–30 minutes, then 500 mg IV every 4–6 hours for 1–2 days **High-Yield:** Atropine does NOT reverse nicotinic effects (muscle weakness, fasciculations, paralysis) — only pralidoxime can do that by reactivating the enzyme. ### Supportive Measures - Oxygen and mechanical ventilation (as in this case: SpO₂ 88%, PaCO₂ 58) - Suction to manage excessive bronchial secretions - Seizure prophylaxis with benzodiazepines if needed (but NOT as first-line) - Avoid depolarizing muscle relaxants (succinylcholine) if intubation required **Clinical Pearl:** The patient's respiratory acidosis (pH 7.28, PaCO₂ 58) is due to bronchospasm and pulmonary edema, not metabolic derangement. Atropine + pralidoxime + ventilation are the cornerstones of management. [cite:Harrison 21e Ch 473] 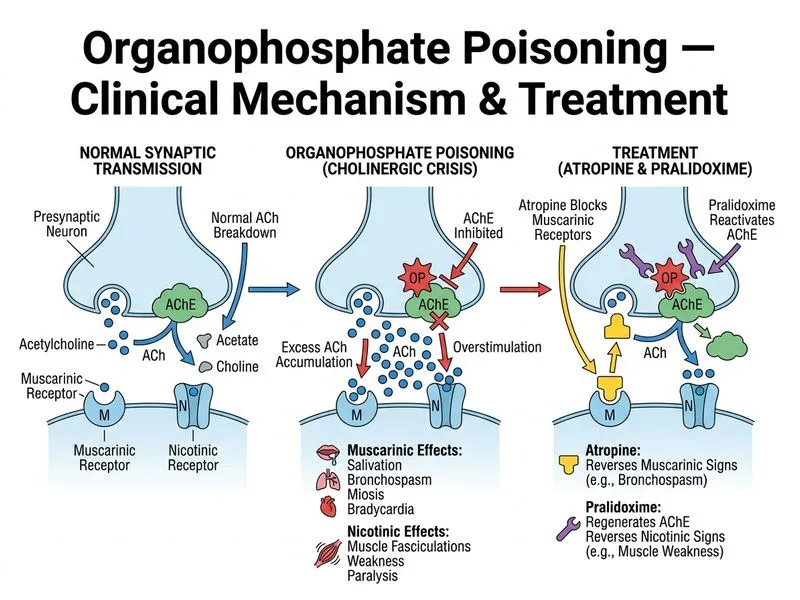
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.