## Immediate Management of Organophosphate Poisoning **Key Point:** Organophosphate compounds irreversibly inhibit acetylcholinesterase, causing accumulation of acetylcholine at synapses and neuromuscular junctions, resulting in a cholinergic crisis. ### Clinical Presentation in This Case - **Muscarinic signs:** Salivation, bronchospasm, pinpoint pupils, bradycardia - **Nicotinic signs:** Muscle fasciculations, weakness - **CNS effects:** Potential seizures, altered consciousness ### Pharmacological Management Algorithm ```mermaid flowchart TD A[Organophosphate Poisoning Confirmed]:::outcome --> B{Respiratory Compromise?}:::decision B -->|Yes| C[Secure airway, intubate if needed]:::action B -->|No| D[Proceed to antidote therapy] D --> E[Atropine 2-5 mg IV]:::action E --> F{Muscarinic signs resolved?}:::decision F -->|No| G[Repeat atropine every 5-10 min]:::action F -->|Yes| H[Add Pralidoxime 1 g IV over 15-30 min]:::action H --> I[Pralidoxime reactivates phosphorylated AChE]:::outcome G --> H ``` ### Dual-Agent Approach: Why Both Atropine AND Pralidoxime? | Agent | Mechanism | Target Symptoms | Timing | |-------|-----------|-----------------|--------| | **Atropine** | Muscarinic antagonist (blocks acetylcholine at M receptors) | Salivation, bronchospasm, bradycardia, miosis | Immediate; repeat every 5–10 min until atropinization | | **Pralidoxime (2-PAM)** | Nucleophilic oxime; reactivates phosphorylated AChE by removing phosphate group | Nicotinic signs (fasciculations, weakness); also supports muscarinic recovery | Within 24–48 hrs of exposure (efficacy decreases with time) | **High-Yield:** Atropine addresses **muscarinic** toxicity (SLUDGE: Salivation, Lacrimation, Urination, Defecation, GI upset, Emesis) immediately. Pralidoxime addresses **nicotinic** toxicity (muscle weakness, fasciculations) and reactivates the enzyme — but only if given early, before "aging" of the phosphorylated enzyme complex occurs. ### Why This Patient Needs Both 1. **Atropine first:** Relieves life-threatening bronchospasm and hypersecretion within minutes. 2. **Pralidoxime second:** Reactivates cholinesterase and addresses muscle weakness; must be given within 24–48 hours (ideally <6 hours) before the phosphate-enzyme bond becomes irreversible ("aging"). **Clinical Pearl:** Pinpoint pupils and bronchospasm are **muscarinic** effects — atropine is the immediate life-saving drug. Muscle fasciculations and weakness are **nicotinic** effects — pralidoxime is needed for complete recovery. **Mnemonic: SLUDGE** — Salivation, Lacrimation, Urination, Defecation, GI upset, Emesis (all muscarinic → treat with atropine). ### Supportive Measures - Secure airway; intubate if respiratory failure develops. - Decontamination: Remove clothing, wash skin thoroughly. - Seizure prophylaxis: Benzodiazepines (diazepam or lorazepam) if seizures occur, but NOT as sole therapy. - Monitor serum and RBC cholinesterase levels. **Warning:** Neostigmine (option B) is a cholinesterase **inhibitor** — it would worsen the crisis by further increasing acetylcholine. Propranolol (option C) addresses only heart rate, not the life-threatening respiratory and muscular manifestations. Diazepam alone (option D) does not address the underlying cholinergic excess. 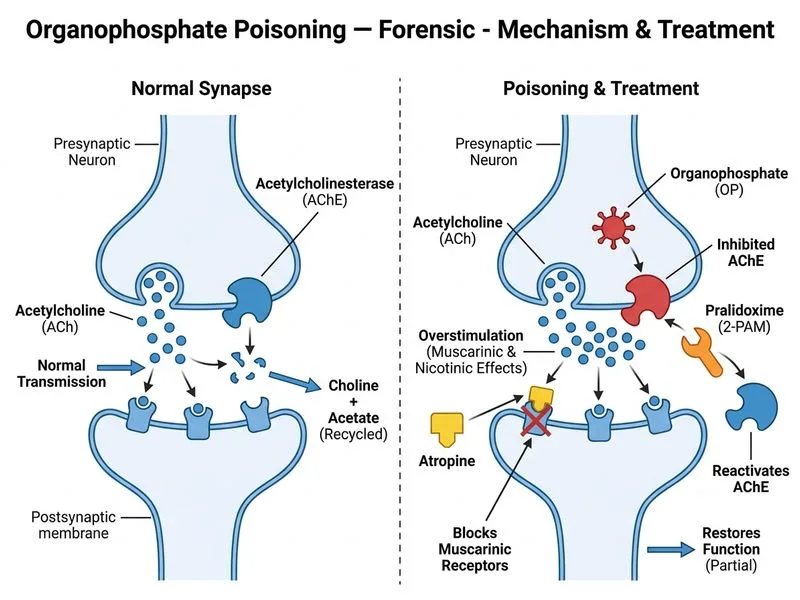
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.