## Seizure Mechanism in Organophosphate Poisoning ### Pathophysiology of CNS Involvement **Key Point:** Organophosphates inhibit acetylcholinesterase (AChE) throughout the central and peripheral nervous systems. Excessive acetylcholine accumulation in the brain disrupts the balance between excitatory (glutamate) and inhibitory (GABA) neurotransmission, leading to seizures. ### Mechanism of Seizure Generation ```mermaid flowchart TD A[Organophosphate Exposure]:::outcome --> B[Irreversible AChE Inhibition]:::outcome B --> C[Acetylcholine Accumulation in CNS]:::outcome C --> D[Excessive Cholinergic Stimulation]:::outcome D --> E{Neuronal Balance Disrupted}:::decision E -->|Excitatory overload| F[Glutamate hyperactivity]:::action E -->|Inhibitory suppression| G[GABA signalling impaired]:::action F --> H[Neuronal Hyperexcitability]:::urgent G --> H H --> I[Seizures, Status Epilepticus]:::urgent ``` ### Why Seizures Occur in Organophosphate Poisoning | Mechanism | Effect | Clinical Consequence | |-----------|--------|---------------------| | **Excessive ACh in CNS** | Overstimulation of cholinergic receptors (nicotinic and muscarinic) | Neuronal hyperexcitability | | **GABA inhibition impaired** | Reduced inhibitory tone in cortex and limbic structures | Loss of seizure threshold control | | **Glutamate dysregulation** | Excitatory neurotransmitter imbalance | Increased seizure propensity | | **Brainstem involvement** | Respiratory centers affected | Apnea, respiratory depression | **High-Yield:** Seizures in organophosphate poisoning are a **CNS cholinergic crisis**, not a metabolic derangement. The seizures reflect the same mechanism as the peripheral muscarinic and nicotinic signs — excessive acetylcholine. ### Clinical Timing of Seizures - **Early seizures (0–24 hours):** Due to acute cholinergic excess; respond to atropine and benzodiazepines. - **Intermediate syndrome seizures (24–96 hours):** May occur despite adequate atropine/pralidoxime therapy; related to prolonged cholinergic stimulation and organophosphate metabolism. - **Late seizures (>96 hours):** Rare; may reflect CNS penetration of organophosphate or residual cholinergic effects. **Clinical Pearl:** In this case, seizures developed 6 hours after exposure — within the acute cholinergic phase. The seizure is a manifestation of **CNS cholinergic toxicity**, not a separate complication. ### Management of Seizures in Organophosphate Poisoning 1. **Benzodiazepines** (diazepam 10 mg or lorazepam 4 mg IV) — first-line for seizure control. 2. **Continue atropine** — addresses underlying cholinergic excess. 3. **Pralidoxime** — reactivates AChE, reducing acetylcholine levels. 4. **Airway management** — intubation if status epilepticus or respiratory failure. 5. **Avoid** phenytoin or carbamazepine — these are less effective and may worsen cholinergic symptoms. **Mnemonic: CNS-ACh Crisis** — Central Nervous System Acetylcholine excess → Seizures, Coma, altered consciousness. **Warning:** Seizures in organophosphate poisoning are NOT due to hypoglycemia, electrolyte abnormalities, or direct cortical toxicity — they are a manifestation of cholinergic excess in the brain. Treating only the seizure (e.g., with phenytoin) without addressing the underlying cholinergic toxicity will fail. 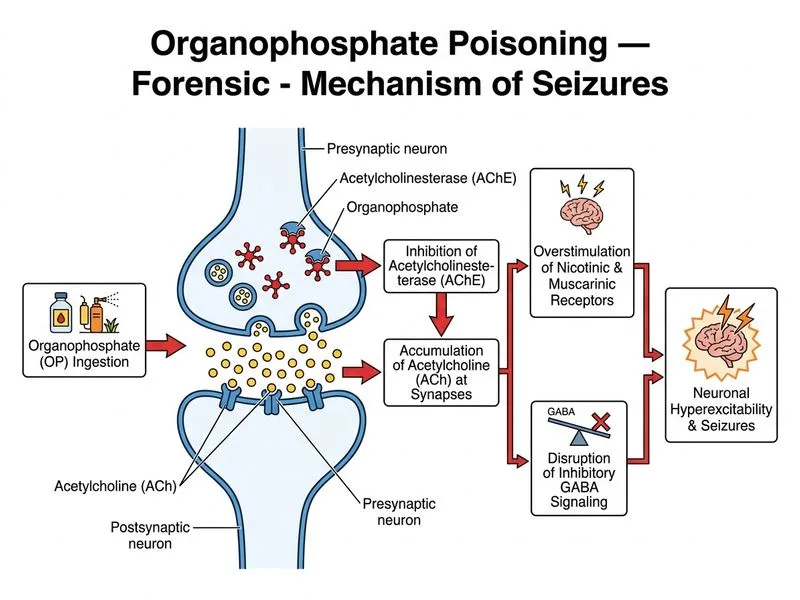
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.