## Immediate Management of Organophosphate Poisoning **Key Point:** In acute organophosphate poisoning with respiratory compromise, atropine is the first-line, life-saving antidote and must be given immediately — even before pralidoxime. ### Rationale for Atropine First Organophosphates irreversibly inhibit acetylcholinesterase, causing accumulation of acetylcholine at muscarinic and nicotinic receptors. This patient exhibits: - **Muscarinic signs:** excessive salivation, lacrimation, pinpoint pupils, respiratory distress - **Nicotinic signs:** muscle fasciculations Atropine is a **competitive antagonist at muscarinic receptors** and: 1. Rapidly reverses life-threatening muscarinic effects (bronchospasm, bronchorrhea, bradycardia) 2. Relieves respiratory distress by drying secretions and opening airways 3. Is the **only agent that works immediately** **High-Yield:** Atropine dosing in organophosphate poisoning: - Initial dose: 2–5 mg IV bolus - Repeat every 5–10 minutes until **signs of atropinization** appear: - Dry mouth - Dilated pupils - Increased heart rate - Cessation of muscle fasciculations - Total dose may reach 50–100 mg or more (no fixed ceiling) ### Role of Pralidoxime (2-PAM) Pralidoxime reactivates acetylcholinesterase by removing the phosphoryl group from the enzyme's active site. However: - It is **NOT a first-line agent** in acute crisis - It is **ineffective at muscarinic receptors** (does not dry secretions or open airways) - It is given **after atropine stabilizes the patient** (typically 1 g IV over 5–30 minutes) - It is most effective if given **within 24–48 hours** of exposure (before "aging" of the enzyme-inhibitor complex occurs) **Clinical Pearl:** The sequence is **ATROPINE FIRST → Supportive care (oxygen, airway management) → PRALIDOXIME SECOND**. ### Why Intubation Is Not the First Step While this patient needs oxygen and airway support, **atropine must be given immediately** because: - It will dry secretions and reduce bronchospasm within minutes - It may prevent the need for intubation if given promptly - Intubation is a secondary measure if atropine + oxygen do not improve respiratory status ### Why Gastric Lavage Is Not Appropriate Here This patient has acute systemic toxicity (respiratory distress, muscle fasciculations). Gastric lavage: - Is too slow and does not address life-threatening respiratory compromise - Is reserved for ingested organophosphates (not inhalation/dermal exposure) - Should never delay antidote administration **Mnemonic:** **SLUDGE** (organophosphate toxidrome) — **S**alivation, **L**acrimation, **U**rination, **D**efecation, **G**astric upset, **E**mesis. Atropine blocks all muscarinic components of SLUDGE. ## Management Algorithm ```mermaid flowchart TD A[Organophosphate exposure confirmed]:::outcome --> B{Respiratory distress or signs of acute toxicity?}:::decision B -->|Yes| C[Atropine 2-5 mg IV bolus immediately]:::action C --> D[Repeat every 5-10 min until atropinization]:::action D --> E[Supplemental oxygen, airway management]:::action E --> F{Stabilized?}:::decision F -->|Yes| G[Pralidoxime 1 g IV after atropine]:::action F -->|No| H[Intubate and ventilate]:::urgent G --> I[Supportive care, monitor for 24-48 hrs]:::outcome B -->|No, mild exposure| J[Observe, give atropine if symptoms develop]:::action ``` [cite:Park 26e Ch 13] 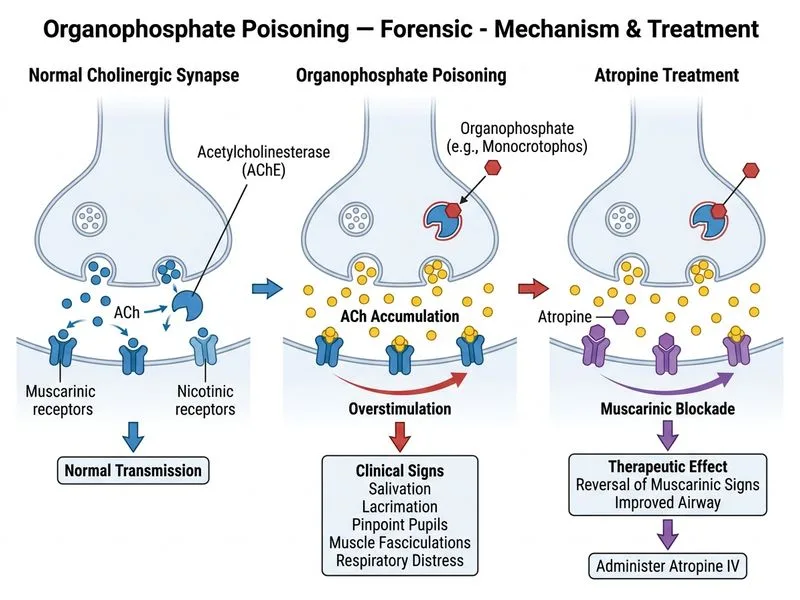
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.