## Post-Atropine Management: Role of Pralidoxime **Key Point:** Once atropine has achieved muscarinic stabilization (dilated pupils, dry mouth, improved respiration), pralidoxime must be given to address nicotinic effects (muscle fasciculations, weakness) and prevent complications like rhabdomyolysis and acute kidney injury. ### Clinical Context: Why Pralidoxime Now? This patient demonstrates: - **Muscarinic stabilization:** dilated pupils, dry mouth, improved respiration (atropine worked) - **Persistent nicotinic effects:** muscle fasciculations, weakness, elevated CK Atropine **does NOT block nicotinic receptors**. Therefore: - Nicotinic effects (fasciculations, weakness, paralysis) persist despite atropine - Pralidoxime reactivates acetylcholinesterase, which restores normal neuromuscular transmission - Pralidoxime is most effective if given **within 24–48 hours** of exposure (before enzyme "aging") **High-Yield:** Pralidoxime (2-PAM) mechanism: - Nucleophilic agent that removes the phosphoryl group from acetylcholinesterase - Restores enzyme activity at **both muscarinic AND nicotinic receptors** - Most effective in the **first 24–48 hours** (before phosphorylated enzyme becomes "aged" and irreversible) - After aging, pralidoxime is ineffective ### Dosing of Pralidoxime | Parameter | Details | |-----------|----------| | **Initial dose** | 1 g IV over 5–30 minutes | | **Maintenance** | 500 mg IV every 4–6 hours for 24–48 hours | | **Maximum daily dose** | 12 g | | **Route** | IV preferred; IM if IV not available | | **Timing** | Most effective within 24–48 hours; limited benefit after 48 hours | **Clinical Pearl:** The combination of **atropine + pralidoxime** is synergistic: - Atropine blocks muscarinic effects (respiratory crisis) - Pralidoxime reactivates the enzyme (resolves all effects if given early) - Together, they address both muscarinic and nicotinic toxicity ### Why Repeated Atropine Is Wrong Atropine: - Blocks muscarinic receptors only - Does NOT reactivate acetylcholinesterase - Does NOT reverse nicotinic effects (fasciculations, weakness) - Repeating atropine will not reduce CK or prevent rhabdomyolysis - Further atropine is contraindicated once atropinization is achieved (risk of atropine toxicity) ### Why Plasmapheresis and Succinylcholine Are Wrong **Plasmapheresis:** - No role in organophosphate poisoning - Organophosphates are lipophilic and bind tightly to acetylcholinesterase; they are not removed by plasma exchange - Not a standard treatment **Succinylcholine:** - **CONTRAINDICATED** in organophosphate poisoning - Succinylcholine is a depolarizing agent that causes muscle fasciculations - In the presence of organophosphate toxicity (already causing fasciculations), succinylcholine will: - Worsen fasciculations and muscle damage - Increase risk of rhabdomyolysis and hyperkalemia - Cause prolonged apnea (due to pseudocholinesterase inhibition by organophosphates) - If intubation is needed, use **non-depolarizing agents** (rocuronium, vecuronium) **Mnemonic:** **PRAM** (organophosphate antidotes) — **P**ralidoxime, **R**espiratory support, **A**tropine, **M**onitoring. Pralidoxime is given after atropine achieves muscarinic stabilization. ## Management Timeline ```mermaid flowchart TD A[Organophosphate poisoning diagnosed]:::outcome --> B[Atropine 2-5 mg IV bolus]:::action B --> C[Repeat atropine every 5-10 min]:::action C --> D{Atropinization achieved?}:::decision D -->|Yes: dilated pupils, dry mouth, improved respiration| E[Pralidoxime 1 g IV over 5-30 min]:::action D -->|No| C E --> F[Pralidoxime 500 mg IV every 4-6 hrs for 24-48 hrs]:::action F --> G[Monitor CK, urine myoglobin, renal function]:::action G --> H{Rhabdomyolysis or AKI?}:::decision H -->|Yes| I[Aggressive IV fluids, alkalinize urine]:::action H -->|No| J[Supportive care, discharge after 48 hrs]:::outcome ``` ### Monitoring for Complications **Rhabdomyolysis risk factors:** - Severe muscle fasciculations - Elevated CK (this patient: 800 U/L, borderline elevated) - Delayed pralidoxime administration - Inadequate hydration **Management of rhabdomyolysis:** - Aggressive IV hydration (target urine output 200–300 mL/hr) - Alkalinize urine (sodium bicarbonate) to prevent myoglobin precipitation in renal tubules - Monitor CK, creatinine, potassium, and urine myoglobin - Consider dialysis if acute kidney injury develops [cite:Park 26e Ch 13; Tripathi KD 8e Ch 35] 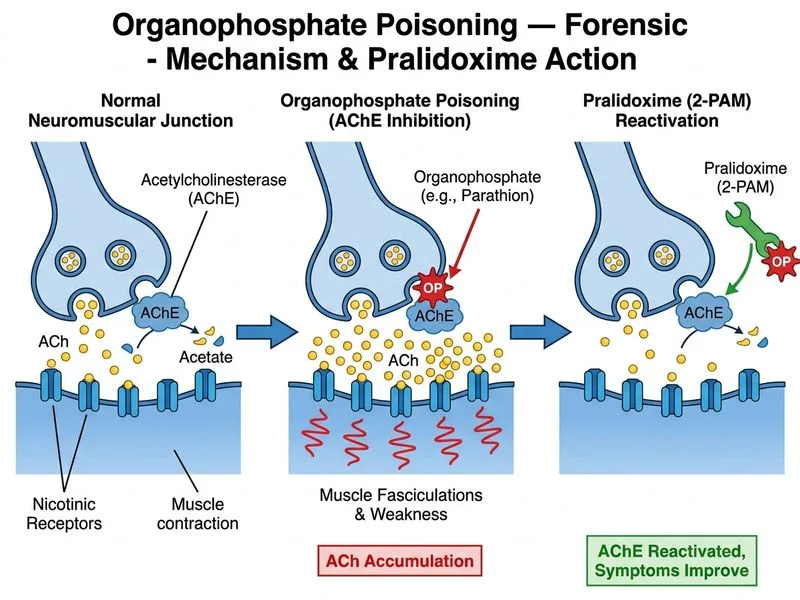
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.