## Pralidoxime (2-PAM) — The Critical Oxime Therapy **Key Point:** Pralidoxime is an **oxime** that reactivates phosphorylated acetylcholinesterase by nucleophilic attack on the phosphorus-enzyme bond. It must be given **early** (ideally within 24–48 hours, efficacy drops after 48 hours) to prevent "aging" of the enzyme-inhibitor complex. ### Mechanism of Pralidoxime Action ```mermaid flowchart TD A[Organophosphate + AChE]:::outcome --> B{Time elapsed?}:::decision B -->|Early < 48 hrs| C[Pralidoxime administered]:::action C --> D[Nucleophilic attack on P-enzyme bond]:::action D --> E[AChE reactivated]:::outcome E --> F[ACh hydrolysis restored]:::outcome B -->|Late > 48 hrs| G[Enzyme aging occurs]:::urgent G --> H[Pralidoxime ineffective]:::urgent H --> I[Permanent AChE inactivation]:::urgent ``` ### Why Pralidoxime Is Essential **High-Yield:** The organophosphate-enzyme complex undergoes **"aging"** — a process where the alkyl group attached to phosphorus is lost, making the bond irreversible even to oximes. This typically occurs within 24–48 hours (varies by agent; some age in hours). | Phase | Time | Reversibility | Treatment | |-------|------|---------------|----------| | **Acute phosphorylation** | 0–2 hrs | Fully reversible | Pralidoxime + atropine | | **Early aging** | 2–24 hrs | Partially reversible | Pralidoxime (still effective) | | **Late aging** | > 48 hrs | Irreversible | Supportive care only | **Clinical Pearl:** Atropine alone treats **muscarinic** symptoms (salivation, bronchospasm, bradycardia) but does **NOT** reactivate the enzyme or treat nicotinic signs (fasciculations, paralysis). Pralidoxime is required for true reversal of the underlying pathology. ### Dosing & Administration - **Initial dose:** 1–2 g IV over 5–10 minutes - **Repeat:** Every 5–10 minutes if signs of cholinergic excess persist - **Maximum:** 12 g/day - **Efficacy window:** Best within 24 hours; some benefit up to 48 hours ### Why Other Options Fail **Mnemonic:** **A-P-E** (Atropine, Pralidoxime, Ensure airway) — the three pillars of organophosphate management. - Atropine (already given) blocks muscarinic effects but does not reverse the enzyme inhibition. - Benzodiazepines and vasopressors are **supportive** measures; they do not address the fundamental enzyme defect. - Activated charcoal is ineffective after 4 hours and is contraindicated in unconscious patients without airway protection. **Warning:** Delayed or omitted pralidoxime therapy results in permanent neurological sequelae, including intermediate syndrome (paralysis of cranial and respiratory muscles 24–96 hours post-exposure) and organophosphate-induced delayed polyneuropathy (OPIDP). [cite:Harrison 21e Ch 473; Park 26e Ch 12] 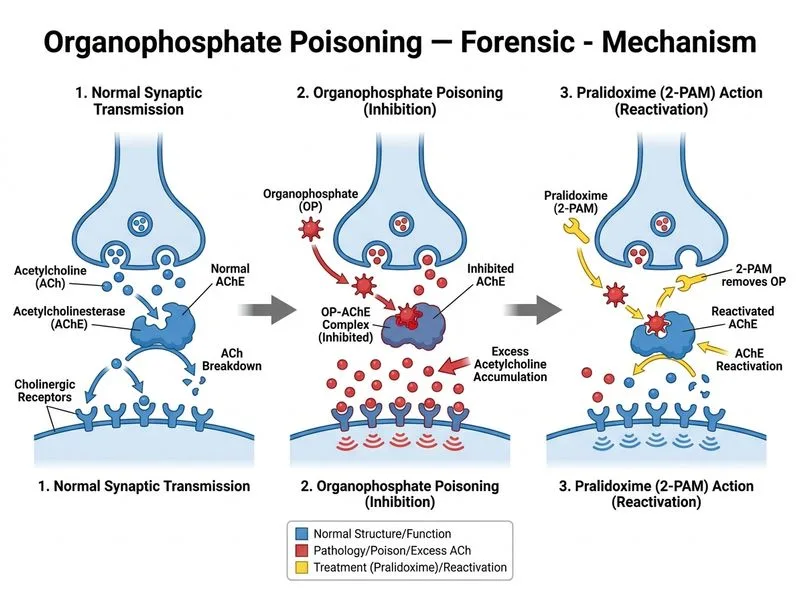
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.