## Clinical Presentation of Organophosphate Poisoning The patient exhibits classic **SLUDGE syndrome** (Salivation, Lacrimation, Urination, Defecation, Gastroenteritis, Emesis) with respiratory compromise — hallmark of acute organophosphate toxicity due to acetylcholinesterase inhibition and cholinergic excess. ## Immediate Management Algorithm ```mermaid flowchart TD A[Organophosphate exposure confirmed]:::outcome --> B{Respiratory distress or<br/>severe cholinergic signs?}:::decision B -->|Yes| C[Secure airway, O₂, suction]:::action C --> D[Atropine 2-5 mg IV bolus]:::action D --> E[Repeat every 5-10 min until<br/>atropinization signs]:::action E --> F[Add pralidoxime 1 g IV<br/>after atropine]:::action B -->|No| G[Atropine + pralidoxime<br/>in sequence]:::action F --> H[Supportive care, monitor]:::action G --> H ``` ## Why Atropine First? **Key Point:** Atropine is the **first-line antidote** in organophosphate poisoning. It is a **muscarinic antagonist** that rapidly reverses cholinergic overstimulation at muscarinic sites (salivation, bronchospasm, bradycardia, miosis). **High-Yield:** Atropine dosing in organophosphate poisoning: - Initial bolus: **2–5 mg IV** - Repeat every **5–10 minutes** until signs of atropinization appear (dry mouth, dilated pupils, increased heart rate, cessation of bronchospasm) - May require **large cumulative doses** (100+ mg over hours) — titrate to effect, not a fixed total **Clinical Pearl:** Atropine does **NOT** reverse nicotinic effects (muscle fasciculations, weakness, paralysis) — that is the role of pralidoxime (oxime), which reactivates acetylcholinesterase. However, **atropine is given first** because it immediately relieves life-threatening muscarinic symptoms (bronchospasm, respiratory failure). ## Sequence of Antidotes | Step | Agent | Mechanism | Timing | |------|-------|-----------|--------| | 1 | Atropine | Muscarinic antagonist | Immediate, repeat q5–10 min | | 2 | Pralidoxime (PAM) | Acetylcholinesterase reactivator | After atropine, 1 g IV bolus, then infusion | | 3 | Supportive care | Airway, O₂, seizure prophylaxis | Concurrent | **Mnemonic:** **ATROPINE FIRST** — Atropine Treats Respiratory Obstruction, Prevents INtubation Emergency. ## Why Not the Other Options? - **Gastric lavage + charcoal (Option B):** Useful for ingested organophosphates, but this is inhalational exposure with **acute respiratory distress** — airway and antidote take priority; decontamination is secondary. - **Cholinesterase levels (Option C):** Diagnostic confirmation, but **treatment must not be delayed** waiting for lab results. Clinical diagnosis is sufficient; levels confirm but do not guide acute dosing. - **Pralidoxime alone (Option D):** Pralidoxime is essential but **must follow atropine** in acute poisoning. Atropine addresses the immediate life threat (bronchospasm, respiratory failure); pralidoxime is added after atropinization to reverse nicotinic effects and prevent relapse. [cite:Park 26e Ch 16] 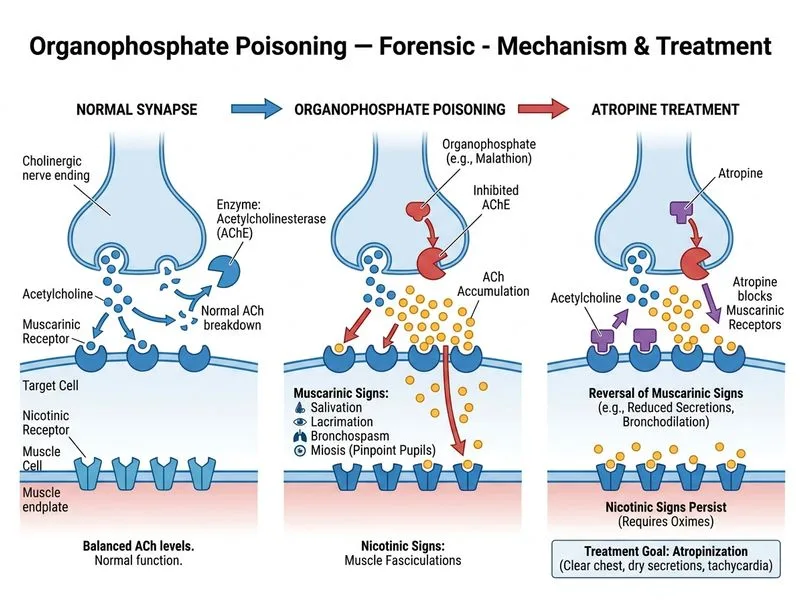
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.