## Investigation of Choice for Osteoarthritis Diagnosis **Key Point:** Plain radiographs are the gold standard first-line imaging for diagnosis and severity assessment of osteoarthritis. They are cost-effective, widely available, and sufficient for clinical decision-making in most cases. ### Why Plain Radiographs? 1. **Diagnostic criteria on X-ray:** - Joint space narrowing (loss of cartilage) - Osteophyte formation (bone spurs) - Subchondral sclerosis (increased bone density) - Subchondral cysts 2. **Kellgren-Lawrence grading system** (0–4) uses radiographs to stage OA severity and guide treatment escalation. 3. **Cost-effectiveness:** Minimal radiation, inexpensive, reproducible for follow-up. ### Radiographic Views for Knee OA | View | Purpose | |------|----------| | **AP (standing)** | Assess medial and lateral compartment joint space | | **Lateral** | Evaluate patellofemoral compartment and posterior osteophytes | | **Skyline (Merchant)** | Assess patellofemoral OA and patellar tracking | **Clinical Pearl:** Morning stiffness <30 minutes and crepitus are classic OA features; radiographs will confirm structural changes. **High-Yield:** Kellgren-Lawrence Grade 2 (minimal OA) may show only questionable osteophytes; Grade 3–4 shows definite joint space narrowing and osteophytes — this guides conservative vs. surgical management. ### When to Use Advanced Imaging - **MRI:** Reserved for atypical presentations, suspected meniscal or ligamentous injury, or when radiographs are inconclusive. - **Contrast-enhanced MRI:** Not routine for uncomplicated OA diagnosis. [cite:Robbins 10e Ch 26] 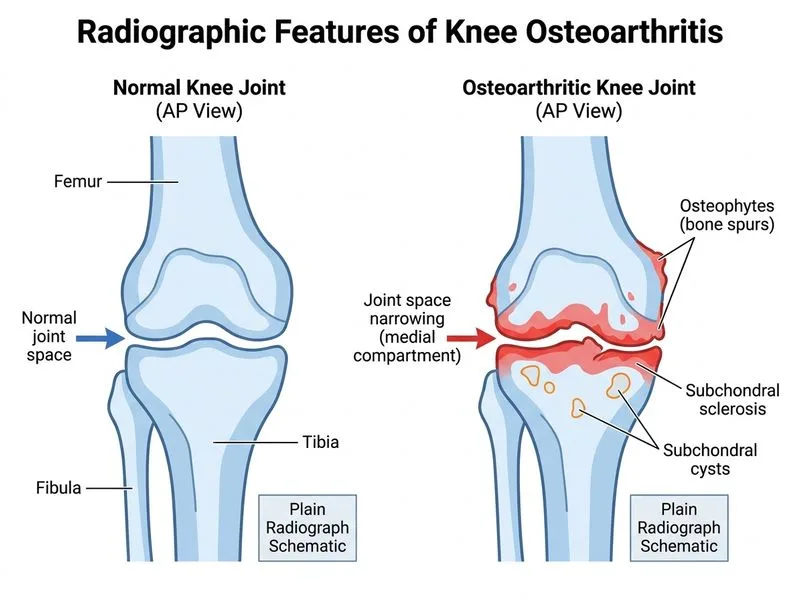
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.