## Primary vs Secondary Osteoarthritis: Radiologic Distinction **Key Point:** The **distribution pattern and anatomic relationship to prior trauma or structural abnormality** is the single most useful radiologic discriminator between primary OA (idiopathic) and secondary OA (post-traumatic, post-inflammatory, or associated with joint dysplasia). ### Comparative Table | Feature | Primary (Idiopathic) OA | Secondary OA | | --- | --- | --- | | **Distribution** | Symmetric, weight-bearing joints (knees, hips, lumbar spine) | Focal, in region of prior injury or abnormality | | **Age of onset** | >50 years | Any age (can occur in 20s–30s if severe trauma) | | **Risk factors** | Obesity, age, female sex, genetic predisposition | Prior fracture, meniscectomy, ligament injury, dysplasia, AVN | | **Pattern on imaging** | Bilateral, symmetric changes | Unilateral or asymmetric; confined to injury zone | | **Osteophytes** | Present in both | Present in both | | **Joint space narrowing** | Concentric (uniform) | Eccentric (focal, at injury site) | | **Associated findings** | None | Evidence of prior trauma (malunion, hardware, ligament laxity) | ### Clinical Significance **High-Yield:** In **primary OA**, the degenerative process is driven by age-related cartilage loss and affects multiple joints symmetrically over decades. In **secondary OA**, the process is accelerated by a specific mechanical insult (fracture, meniscectomy, chronic instability, or underlying joint dysplasia), and changes are **localized to the injury zone**. **Clinical Pearl:** A 35-year-old with severe OA in the medial compartment of the knee following a tibial plateau fracture 10 years earlier has **secondary OA**. The focal distribution in the weight-bearing zone of the fracture, combined with the young age and clear temporal relationship to trauma, distinguishes it from idiopathic OA. ### Radiologic Findings in Both **Warning:** Osteophytes, subchondral sclerosis, and cyst formation occur in **both primary and secondary OA**. These are features of OA itself, not discriminators between the two types. The key is the **pattern and distribution**, not the presence or absence of individual radiologic signs. ### Why Other Options Are Incorrect - **Osteophytes:** Present in both primary and secondary OA. This is a hallmark of OA pathology, not a discriminator. - **Asymmetric joint space narrowing and focal cartilage loss:** While secondary OA often shows focal changes, primary OA can also show asymmetric changes in early stages. This is not a reliable discriminator. - **Subchondral bone sclerosis and cyst formation:** These represent advanced OA changes and occur in both types. They reflect the severity of OA, not its etiology. [cite:Robbins 10e Ch 27; Harrison 21e Ch 326] 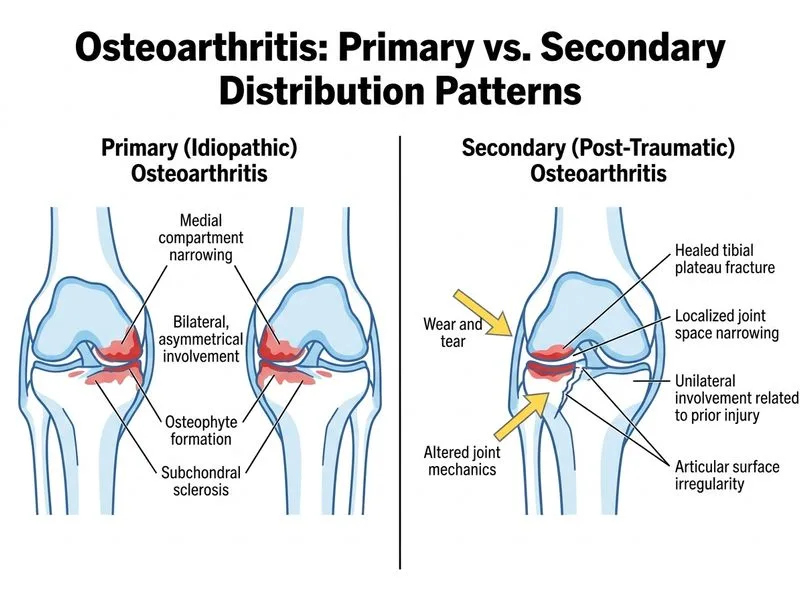
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.