## Clinical Diagnosis: Osteomalacia ### Key Clinical Features **Key Point:** Osteomalacia is defective mineralization of the bone matrix in adults, resulting from vitamin D deficiency, impaired metabolism, or phosphate depletion. This patient presents the classic triad: 1. **Biochemical abnormalities:** Low 25-OH vitamin D (12 ng/mL), hypocalcemia (7.2 mg/dL), elevated PTH (secondary hyperparathyroidism), and elevated alkaline phosphatase. 2. **Clinical manifestations:** Bone pain, muscle weakness (myopathy), and gait disturbance (Trendelenburg sign). 3. **Radiological findings:** Looser zones (pseudofractures) and loss of corticomedullary differentiation are pathognomonic for osteomalacia. ### Biochemical Pattern in Osteomalacia | Parameter | Osteomalacia | Osteoporosis | Renal Osteodystrophy | |-----------|--------------|--------------|----------------------| | 25-OH Vitamin D | **↓ (<20 ng/mL)** | Normal | Normal or ↓ | | Serum Calcium | ↓ or Normal | Normal | ↓ | | Serum Phosphate | ↓ or Normal | Normal | ↑ | | PTH | ↑ (secondary) | Normal | ↑↑ (severe) | | Alkaline Phosphatase | ↑ | Normal | ↑↑ | | Looser Zones | **Present** | Absent | May be present | **High-Yield:** The **low 25-OH vitamin D level (12 ng/mL)** is the diagnostic hallmark. This is the most specific marker of vitamin D deficiency. ### Pathophysiology ```mermaid flowchart TD A[Vitamin D Deficiency<br/>Low sun exposure/dietary intake]:::outcome --> B[↓ 25-OH Vitamin D]:::outcome B --> C[Impaired intestinal Ca absorption]:::outcome C --> D[Hypocalcemia]:::outcome D --> E[↑ PTH secretion<br/>Secondary hyperparathyroidism]:::action E --> F[↑ Alkaline phosphatase<br/>Increased bone turnover]:::action F --> G[Defective mineralization<br/>of osteoid]:::urgent G --> H[Looser zones<br/>Bone pain & weakness]:::outcome ``` ### Why Looser Zones Are Diagnostic **Clinical Pearl:** Looser zones (pseudofractures) are bands of radiolucency perpendicular to the bone cortex, representing areas of unmineralized osteoid. They are virtually pathognomonic for osteomalacia and are NOT seen in osteoporosis. **Mnemonic: LOOSER** — **L**ack of mineralization, **O**steoid accumulation, **O**steomalacia diagnosis, **S**earch for these zones, **E**arly radiological sign, **R**adiolucent bands. ### Clinical Pearl: Muscle Involvement Osteomalacia causes a **proximal myopathy** (type II fiber atrophy) independent of hypocalcemia, leading to muscle weakness and difficulty with hip flexion (Trendelenburg sign). This distinguishes it from simple hypocalcemia. [cite:Robbins 10e Ch 26] 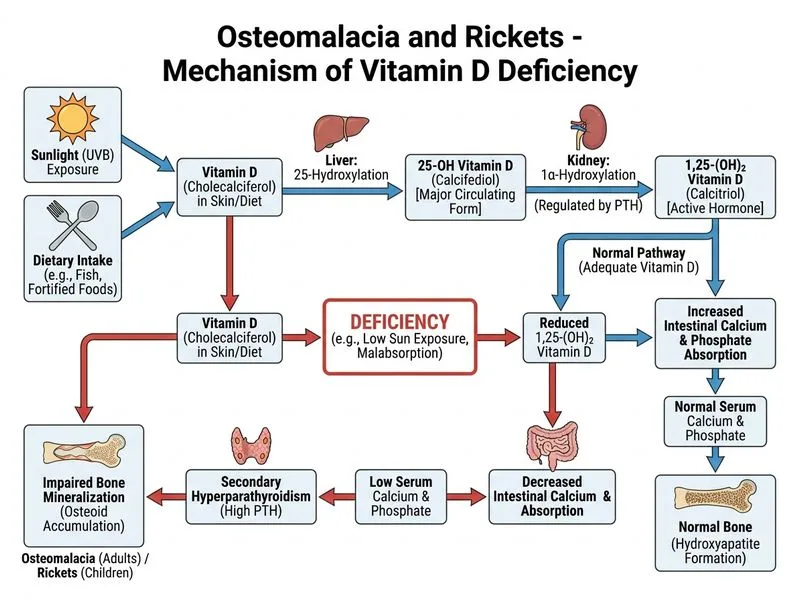
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.