## Diagnostic Approach to Osteomalacia **Key Point:** Serum 25-hydroxyvitamin D [25(OH)D] is the gold standard screening and confirmatory test for osteomalacia because it reflects total body vitamin D stores and has the longest half-life (~2–3 weeks). ### Why 25(OH)D is the Investigation of Choice **High-Yield:** 25(OH)D levels directly correlate with vitamin D status: - **< 20 ng/mL (50 nmol/L):** Deficiency (osteomalacia) - **20–29 ng/mL:** Insufficiency - **≥ 30 ng/mL:** Sufficient In this patient, the clinical presentation (bone pain, muscle weakness, fractures, hypocalcemia, hyperphosphatasia) is classic for osteomalacia, and 25(OH)D measurement will confirm vitamin D deficiency as the underlying cause. ### Comparison of Vitamin D Metabolites | Investigation | Purpose | Half-life | Clinical Use | |---|---|---|---| | **25(OH)D** | Screening & diagnosis | 2–3 weeks | Gold standard for osteomalacia | | **1,25(OH)₂D** | Assess renal conversion | 4–6 hours | Used in renal disease, hypercalcemia | | **PTH** | Secondary hyperparathyroidism | Variable | Elevated in osteomalacia but not diagnostic | | **Bone biopsy** | Histological confirmation | N/A | Reserved for diagnostic uncertainty | **Clinical Pearl:** In osteomalacia, 1,25(OH)₂D may be normal or even elevated because the parathyroid gland compensates by increasing PTH, which stimulates renal 1α-hydroxylase. Therefore, 1,25(OH)₂D alone is insufficient for diagnosis. ### Laboratory Pattern in Osteomalacia ```mermaid flowchart TD A[Vitamin D Deficiency]:::outcome --> B[↓ 25-OH Vitamin D]:::action B --> C[↓ Serum Calcium]:::outcome C --> D[↑ PTH]:::outcome D --> E[↑ 1,25-OH Vitamin D<br/>Compensatory]:::outcome D --> F[↑ Alkaline Phosphatase]:::outcome B --> G[Confirm Osteomalacia]:::action ``` **Mnemonic:** **"25 for Diagnosis, 1,25 for Pathology"** — Use 25(OH)D to diagnose vitamin D deficiency; use 1,25(OH)₂D to understand renal or metabolic complications. 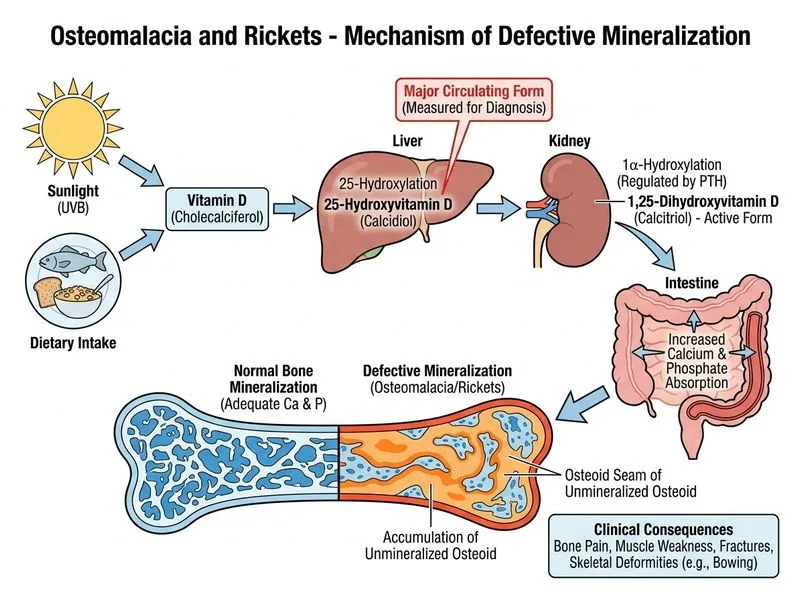
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.