## Nutritional Rickets Management — First-Line Approach ### Clinical and Biochemical Diagnosis **Key Point:** This child has **nutritional rickets** (vitamin D-deficient rickets), the most common form in India. The absence of malabsorption or renal disease, combined with severe 25-OH vitamin D deficiency (8 ng/mL) and secondary hyperparathyroidism, confirms the diagnosis. ### Why High-Dose Vitamin D (Cholecalciferol) Is the Gold Standard **High-Yield:** First-line treatment for nutritional rickets is **high-dose cholecalciferol (vitamin D₃)**: - **Dose:** 1–2 million IU daily OR 50,000 IU weekly for 6–12 weeks - **Mechanism:** Replenishes depleted 25-OH vitamin D stores; PTH suppression follows within 2–4 weeks - **Cost-effective:** Cholecalciferol is inexpensive and widely available in India - **Physiological:** Restores normal calcium–phosphate homeostasis without bypassing renal 1α-hydroxylase ### Concurrent Calcium Supplementation **Clinical Pearl:** Calcium (1–1.5 g/day elemental calcium) must accompany vitamin D because: - Vitamin D alone may cause severe hypocalcemia if dietary calcium is inadequate - Prevents tertiary hyperparathyroidism during repletion - Accelerates healing of metaphyseal changes ### Dietary Counseling Educate parents on: - Sun exposure (15–30 min/day, 3–4 times/week) - Dietary calcium sources (milk, fortified foods, leafy greens) - Vitamin D fortification programs ### Timeline of Improvement | Parameter | Timeline | |-----------|----------| | Biochemical (Ca, PO₄, ALP) | 2–4 weeks | | PTH normalization | 4–8 weeks | | Symptom relief (pain, weakness) | 2–4 weeks | | Radiological healing | 3–6 months | | Complete resolution | 6–12 months | ### Why Calcitriol Monotherapy Is Inadequate **Warning:** Active vitamin D (calcitriol) alone without calcium supplementation risks severe hypocalcemia and is not first-line. Calcitriol is reserved for: - Renal osteodystrophy (impaired renal 1α-hydroxylase) - Hypoparathyroidism - Severe hypocalcemia requiring rapid correction [cite:Park 26e Ch 3; Harrison 21e Ch 297] 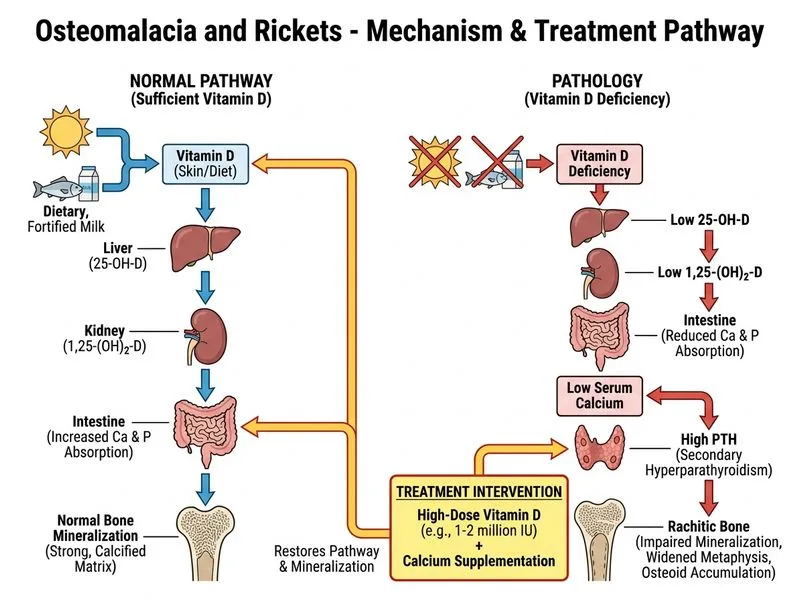
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.