## Clinical Diagnosis: Staphylococcus aureus Osteomyelitis ### Key Features of This Case **High-Yield:** While Pseudomonas aeruginosa is classically associated with osteomyelitis following puncture wounds through **rubber-soled shoes** (particularly in children/adolescents), **Staphylococcus aureus** remains the **single most common cause of osteomyelitis overall**, including post-traumatic osteomyelitis from contaminated wounds in adults. The clinical vignette here describes a construction worker with a contaminated nail puncture — a direct inoculation scenario where S. aureus (a ubiquitous skin and environmental commensal) is the predominant pathogen. ### Organism-Specific Epidemiology | Feature | S. aureus | Pseudomonas aeruginosa | S. pyogenes | M. tuberculosis | |---------|-----------|------------------------|-------------|------------------| | **Most common cause overall** | ✅ Yes (all age groups) | No | No | No | | **Puncture wound (rubber shoe)** | Less typical | Classic (children) | Rare | Rare | | **Post-traumatic (nail/soil)** | Most common | Less common | Rare | Rare | | **Sinus tract formation** | Common | Common | Uncommon | Common | | **Systemic toxicity** | Variable | Moderate–high | High | Low | | **Radiographic changes** | Early (2–3 weeks) | Early | Rare | Late (months) | ### Pathophysiology 1. **Inoculation route:** Direct implantation via contaminated nail puncture wound 2. **S. aureus ecology:** Gram-positive coccus, the most common skin/soft tissue pathogen; colonizes skin, nares, and environmental surfaces 3. **Virulence:** Produces coagulase, protein A, leukocidins, and biofilm — enabling rapid bone invasion and abscess/sinus tract formation 4. **Clinical course:** Acute presentation within 2–4 weeks with periosteal reaction, bone destruction, and draining sinus tract — exactly as described in this vignette **Key Point:** According to **Harrison's Principles of Internal Medicine** and **Robbins Pathologic Basis of Disease**, *S. aureus* accounts for **>50% of all osteomyelitis cases** across all age groups and etiologies, including post-traumatic and hematogenous forms. It is the default answer unless a highly specific epidemiological clue (e.g., rubber-soled shoe puncture in a child, IV drug use → Pseudomonas; sickle cell disease → Salmonella; immunocompromised → fungi) is present. ### Why NOT Pseudomonas Here? The Pseudomonas–puncture wound association is specifically tied to **nail puncture through rubber-soled shoes** (sneakers/tennis shoes), where Pseudomonas colonizes the inner foam/rubber. This vignette describes a **contaminated nail** in a **construction setting** — not a rubber-soled shoe scenario. In this context, S. aureus is the most likely pathogen. **Clinical Pearl:** The classic teaching mnemonic for osteomyelitis organisms: - **S. aureus** → Most common in ALL groups (default answer) - **Pseudomonas** → Puncture wound through rubber shoe; IV drug users - **Salmonella** → Sickle cell disease - **Group B Strep / E. coli** → Neonates - **M. tuberculosis** → Chronic, insidious; vertebral (Pott's disease) **High-Yield:** Always think **S. aureus** first in osteomyelitis unless a specific epidemiological clue points elsewhere. The presence of fever, elevated WBC, ESR, CRP, periosteal reaction, and draining sinus tract in an adult with a contaminated wound is the classic S. aureus osteomyelitis picture. [cite: Harrison's Principles of Internal Medicine, 21st Ed., Ch. 126; Robbins & Cotran Pathologic Basis of Disease, 10th Ed., Ch. 26] 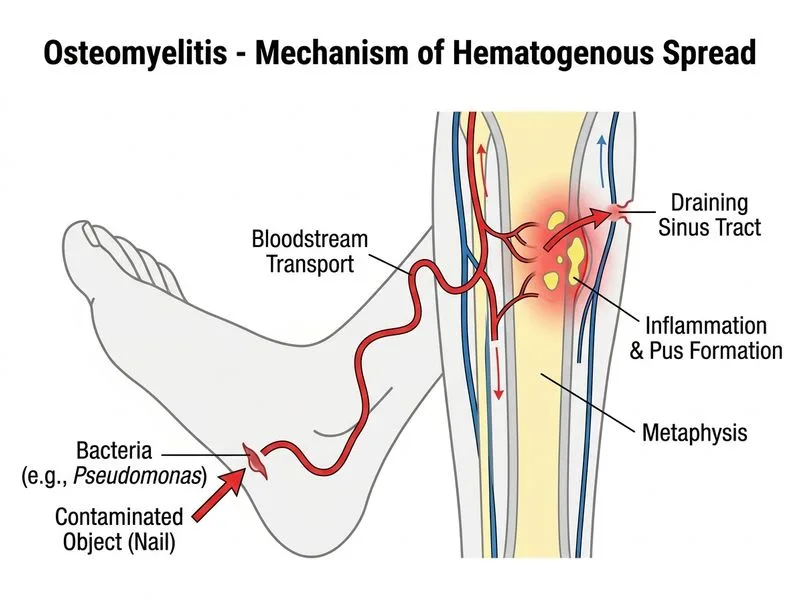
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.