## Clinical Diagnosis: Acute Hematogenous Osteomyelitis (Distal Femur) ### Key Diagnostic Features **High-Yield:** This is a classic presentation of **acute hematogenous osteomyelitis** in a child. The diagnosis rests on: 1. **Age:** 7 years old (peak incidence 5–15 years) 2. **Location:** Distal femur metaphysis (most common site in children) 3. **Acute onset:** Fever, severe pain, refusal to bear weight over 10 days 4. **Organism:** Staphylococcus aureus (accounts for 70–80% of acute hematogenous osteomyelitis in children) 5. **Imaging findings:** Metaphyseal lucency with marrow edema and periosteal reaction on MRI — hallmark of acute osteomyelitis ### Pathophysiology of Acute Hematogenous Osteomyelitis ```mermaid flowchart TD A[Minor trauma or bacteremia]:::outcome --> B[Bacteria lodge in metaphyseal capillary loops]:::outcome B --> C[Slowed blood flow in metaphyseal sinusoids]:::outcome C --> D[Bacterial proliferation & inflammation]:::action D --> E[Pus formation & increased intraosseous pressure]:::urgent E --> F[Ischemia of bone & periosteal lifting]:::urgent F --> G[Periosteal new bone formation]:::outcome G --> H[Radiographic changes visible]:::outcome ``` **Key Point:** The metaphysis is the primary site of infection in children because: - Capillary loops slow blood flow (ideal for bacterial seeding) - Lack of phagocytic activity in sinusoids - Metaphyseal vessels are end-arteries (poor collateral circulation) ### Why NOT Acute Suppurative Arthritis? | Feature | Acute Osteomyelitis | Acute Suppurative Arthritis | |---------|---------------------|-----------------------------| | **MRI finding** | Metaphyseal marrow edema, periosteal reaction | Joint effusion, synovial enhancement | | **Joint involvement** | No effusion (unless rupture through cortex) | Effusion present in >90% of cases | | **Radiographic lucency** | Metaphyseal (bone) | Cartilage space preserved initially | | **Prognosis** | Good with antibiotics + drainage | Risk of cartilage destruction | This patient's MRI explicitly states **"without joint effusion"** — a crucial finding that excludes suppurative arthritis and confirms osteomyelitis confined to bone. ### Clinical Presentation Pearls **High-Yield:** Classic "**toxic child**" presentation: - High fever (38–40°C) - Severe localized pain - Refusal to move the limb (pseudoparalysis) - Swelling and warmth over the metaphysis - Elevated inflammatory markers (WBC, ESR, CRP) **Clinical Pearl:** In children, the distal femur and proximal tibia are the **most common sites** because they are the fastest-growing metaphyses with the highest blood flow. The minor fall 2 weeks ago may have caused a small hematoma, providing a nidus for bacterial seeding during bacteremia. ### Imaging Interpretation 1. **Plain radiographs:** Early findings (soft-tissue swelling, subtle lucency) appear at 7–10 days 2. **MRI (gold standard for early diagnosis):** - Metaphyseal marrow edema (T2 hyperintensity) - Periosteal reaction - Absence of joint effusion (rules out arthritis) 3. **Blood culture:** Positive in 50–60% of cases; S. aureus is the most common isolate **Mnemonic: MOPS** — **M**etaphysis, **O**steomyelitis, **P**ediatric, **S**taphylococcus aureus ### Management Implications 1. **Antibiotics:** Anti-staphylococcal coverage (cephalosporin or anti-MRSA agent if risk factors) 2. **Surgical drainage:** Indicated if pus under tension or no clinical improvement in 48 hours 3. **Duration:** 4–6 weeks IV antibiotics, then oral step-down [cite:Tuli's Orthopedics 8e Ch 6; Robbins 10e Ch 26] 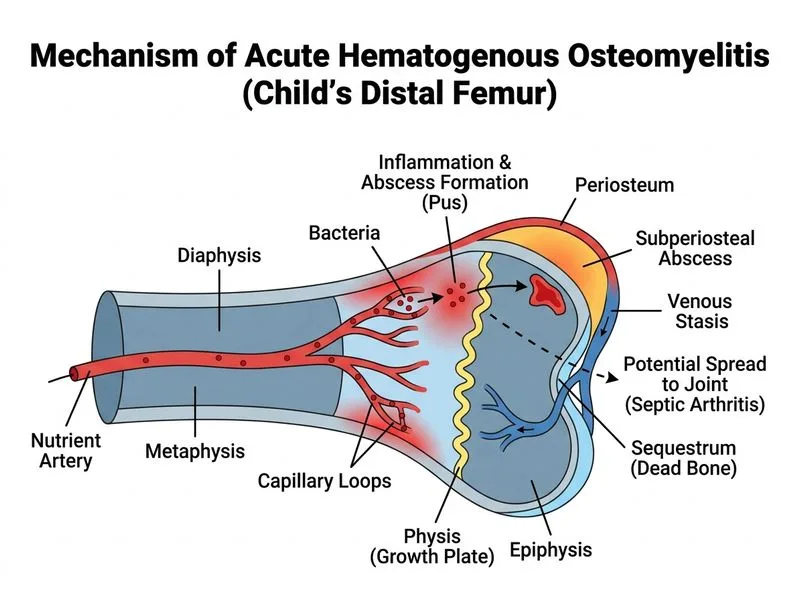
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.