## Clinical Context This patient has chronic osteomyelitis (6-week duration) with clinical and radiological evidence (periosteal reaction, cortical thickening, draining sinus). The presence of purulent discharge and systemic signs warrants immediate antimicrobial therapy. ## Why Empiric Antibiotics Are Correct **Key Point:** In osteomyelitis with positive clinical and radiological findings, empiric broad-spectrum antibiotics should NOT be delayed while awaiting culture results. Delayed therapy increases risk of treatment failure, abscess formation, and systemic complications. **High-Yield:** The standard empiric regimen for osteomyelitis in India (where *Staphylococcus aureus* and *Mycobacterium tuberculosis* are common) is: - IV ceftriaxone (3rd-generation cephalosporin for gram-negative coverage and bone penetration) - IV gentamicin (aminoglycoside for synergy and gram-negative coverage) - This combination provides coverage for most causative organisms while awaiting culture sensitivities ## Timeline of Management 1. **Immediate (Day 0):** Blood and pus cultures, empiric IV antibiotics 2. **Days 1–3:** Await culture and sensitivity results; adjust antibiotics accordingly 3. **Week 1–2:** Assess clinical response; if inadequate, proceed to surgical debridement 4. **Imaging:** MRI is reserved for surgical planning after initial antibiotic response assessment, not as a first step **Clinical Pearl:** Chronic osteomyelitis with a draining sinus is polymicrobial in ~40% of cases; empiric broad-spectrum coverage is essential until culture directs de-escalation. **Warning:** Do NOT delay antibiotics for imaging or further culture. Early aggressive therapy improves outcomes and reduces the need for extensive surgery. 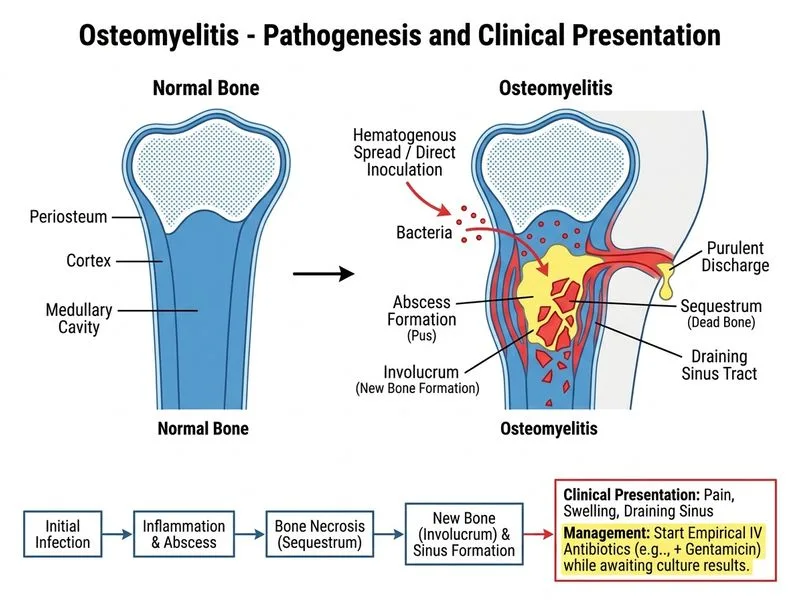
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.