## Clinical Diagnosis: Acute Hematogenous Osteomyelitis ### Case Analysis This child presents with the classic presentation of acute hematogenous osteomyelitis: - **Age:** 7 years old (peak incidence 5–15 years) - **Onset:** Acute fever and localized bone pain over 10 days - **Location:** Distal femur (metaphyseal region—classic site) - **Organism:** *Staphylococcus aureus* on blood culture - **Imaging:** Periosteal reaction and cortical thickening (hallmark of acute osteomyelitis) ### Pathophysiology of Acute Hematogenous Osteomyelitis ```mermaid flowchart TD A[Bacteremia<br/>S. aureus]:::outcome --> B[Lodges in bone<br/>metaphyseal capillaries]:::action B --> C[Inflammatory response<br/>pus accumulation]:::action C --> D{Pressure rises<br/>in medullary cavity}:::decision D -->|Ruptures cortex| E[Subperiosteal abscess]:::outcome D -->|Spreads along bone| F[Cortical destruction]:::outcome E --> G[Periosteal reaction<br/>new bone formation]:::outcome F --> G G --> H[X-ray findings:<br/>periosteal elevation]:::outcome ``` ### Key Distinguishing Features | Feature | Acute Hematogenous Osteomyelitis | Septic Arthritis | Chronic Osteomyelitis | |---------|----------------------------------|------------------|----------------------| | **Onset** | Acute (days) | Acute (hours–days) | Insidious (weeks–months) | | **Site** | Metaphysis of long bones | Joint space | Bone with sinus tract | | **Blood culture** | Positive (80–90%) | Positive (50%) | Often negative | | **Imaging** | Periosteal reaction, cortical thickening | Joint effusion, cartilage loss | Sequestra, involucra | | **Sinus tract** | Absent initially | Absent | Present | | **Duration** | < 2 weeks | < 1 week | > 4 weeks | **Key Point:** The presence of **positive blood culture with periosteal new bone formation** on X-ray is diagnostic of acute hematogenous osteomyelitis. This patient has NOT yet developed a sinus tract, ruling out chronic disease. ### Why the Distal Femur? **High-Yield:** In children, osteomyelitis preferentially affects the **metaphyseal regions** of long bones because: 1. Rich vascular supply with slow blood flow (capillary loops) 2. Bacteria lodge and proliferate in these areas 3. Distal femur, proximal tibia, proximal humerus are the "big three" sites ### Clinical Pearl The **2-week timeline** (fall → apparent healing → fever/swelling) is typical. The initial trauma may have caused a small breach in skin flora, but bacteremia occurred later, seeding the bone. The absence of a sinus tract at presentation indicates this is still in the acute phase. **Mnemonic: SOFT** — *S. aureus*, *Osteomyelitis*, *Fever*, *Trauma* (recent) ### Management 1. Blood culture before antibiotics (already done—positive) 2. Imaging: X-ray (done), MRI for soft tissue extent 3. Empiric antibiotics: Anti-staphylococcal agent (cloxacillin 50 mg/kg/day IV or cephalosporin) 4. Surgical drainage if abscess formation or no clinical improvement in 48 hrs 5. Duration: 4–6 weeks IV, then oral step-down [cite:Tuli's Tuberculosis of the Skeletal System 5e Ch 2; Rockwood & Green's Fractures in Adults 9e Ch 12] 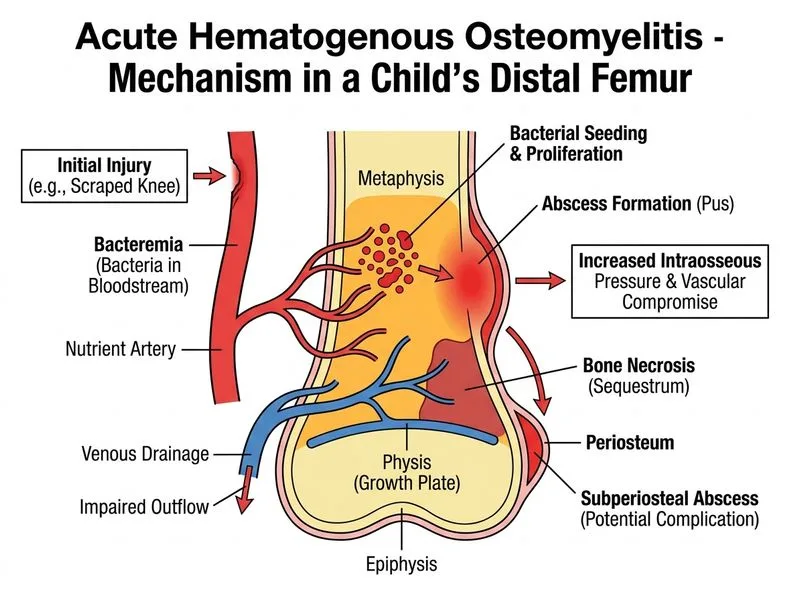
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.