## Clinical Diagnosis: Contiguous Osteomyelitis ### Key Features of This Case **Key Point:** The puncture wound to the plantar foot 6 weeks prior is the source of infection. Pseudomonas aeruginosa is the classic organism associated with puncture wounds, particularly those contaminated with soil or water. **High-Yield:** Puncture wounds to the foot (especially through rubber-soled shoes) are notorious for introducing Pseudomonas into deep tissues. The organism thrives in moist environments and can track along tissue planes to reach bone. ### Osteomyelitis Classification & Pathogenesis This case represents **contiguous osteomyelitis** (also called osteomyelitis secondary to soft tissue infection), not haematogenous spread. The infection originated from the puncture wound and spread locally to the tibia. ### Why Pseudomonas aeruginosa? | Feature | Pseudomonas aeruginosa | |---------|------------------------| | **Source** | Soil, water, moist environments | | **Common portal** | Puncture wounds, especially plantar foot | | **Virulence factor** | Produces exotoxins, biofilms; thrives in anaerobic environments | | **Bone tropism** | Not inherent; reaches bone via direct inoculation or contiguous spread | | **Antibiotic resistance** | Intrinsic resistance to many β-lactams; requires fluoroquinolones or anti-pseudomonal agents | **Clinical Pearl:** A plantar puncture wound with a small, often-overlooked scar is the classic presentation. The patient may not recall or report the injury if it was minor and painless initially. ### Diagnostic Confirmation 1. **Positive blood culture + bone culture** = confirms osteomyelitis (not just soft tissue infection) 2. **Imaging findings** (mixed lytic/sclerotic, periosteal reaction) = consistent with acute-to-subacute osteomyelitis 3. **Organism identification** (Pseudomonas) = confirms puncture wound source **Mnemonic: FOOT PUNCTURE PSEUDOMONAS** — Foot puncture wounds → Pseudomonas → Contiguous osteomyelitis ### Management Implications - **Antibiotic choice:** Fluoroquinolones (ciprofloxacin) or anti-pseudomonal penicillins (piperacillin-tazobactam) + aminoglycosides - **Duration:** 4–6 weeks IV, then oral step-down - **Surgical debridement:** May be needed if abscess or sequestrum present [cite:Rockwood & Green's Fractures in Adults Ch 37] 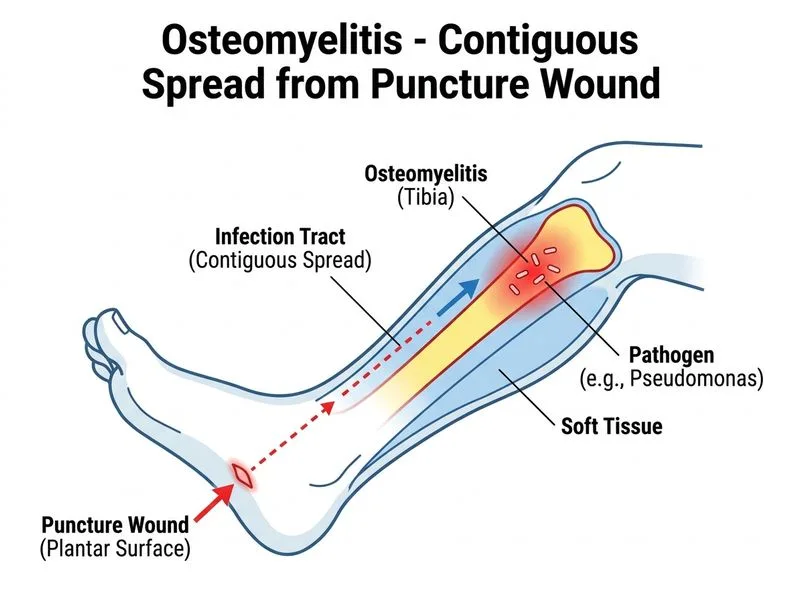
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.