## Clinical Diagnosis: Acute Haematogenous Osteomyelitis ### Key Clinical Features **High-Yield:** This is a classic presentation of acute haematogenous osteomyelitis in a child: - **Age:** 7 years old (peak incidence 5–15 years) - **Acute onset:** 10 days of fever and severe pain - **Site:** Metaphyseal region of long bone (distal femur) — the most common location in children - **No obvious portal of entry:** Haematogenous spread, not contiguous or traumatic inoculation - **Negative blood culture:** Does not exclude osteomyelitis; positive in only 40–50% of cases **Key Point:** The **metaphyseal location** is the diagnostic clue. In children, the metaphyseal blood vessels are end-arteries that slow blood flow, allowing bacterial seeding. This is why osteomyelitis in children almost always begins in the metaphysis of long bones. ### Why Not Septic Arthritis? | Feature | Septic Arthritis | Osteomyelitis | |---------|------------------|---------------| | **Joint fluid** | Purulent, positive culture | Not applicable | | **Imaging hallmark** | Joint effusion, cartilage erosion | Metaphyseal lucency, periosteal reaction | | **MRI finding** | Synovial enhancement, joint fluid signal | Bone marrow edema, intramedullary signal change | | **Blood culture** | Often positive (70–80%) | Often negative (40–50%) | | **Typical organism** | S. aureus, Gram-negatives | S. aureus (>80% in children) | **Clinical Pearl:** Although the knee is swollen and painful, the **MRI clearly shows a bone lesion (metaphyseal T2 hyperintensity with marrow edema)**, not just joint inflammation. This is osteomyelitis, not arthritis. ### Pathophysiology of Haematogenous Osteomyelitis in Children 1. **Bacteraemia** (often subclinical; source may be minor trauma, skin infection, or dental procedure) 2. **Seeding in metaphyseal vessels** (slow blood flow, end-arteries, minimal phagocytosis) 3. **Bacterial proliferation** → abscess formation → pus under pressure 4. **Periosteal reaction** and cortical perforation (if untreated) 5. **Systemic inflammation** (fever, elevated inflammatory markers) **Mnemonic: METAPHYSIS in KIDS** — Metaphysis is the haematogenous osteomyelitis site in children (not adults, where the diaphysis is more common). ### Diagnostic Confirmation - **Elevated inflammatory markers** (WBC 14,500, CRP 8.2, ESR 65) = acute infection - **Negative blood culture** = does not rule out osteomyelitis; bone culture or aspiration would be diagnostic - **MRI findings** = gold standard for early detection; shows bone marrow edema and periosteal reaction before X-ray changes appear - **No joint effusion** = argues against septic arthritis ### Most Likely Organism **Staphylococcus aureus** accounts for >80% of acute haematogenous osteomyelitis in children. MRSA prevalence varies by region but is increasing in India. ### Management 1. **Empiric antibiotics:** Anti-staphylococcal coverage (flucloxacillin or cephalosporin; add vancomycin if MRSA suspected) 2. **Bone aspiration/culture:** Definitive diagnosis and organism identification 3. **Duration:** 4–6 weeks IV, then oral step-down based on clinical response 4. **Surgical drainage:** If abscess formation or no clinical improvement in 48 hours [cite:Canale & Beaty Operative Orthopaedics 13e Ch 49; Tuli's Tuberculosis of the Skeletal System 6e Ch 2] 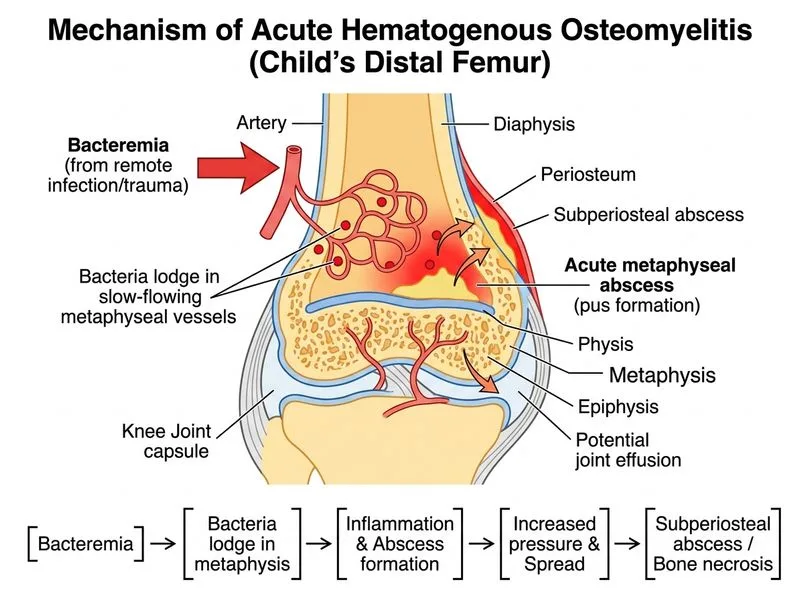
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.