## Diagnosis of Osteomyelitis: Investigation Hierarchy **Key Point:** Bone biopsy with culture and sensitivity is the gold standard for confirming osteomyelitis and identifying the causative organism, especially when blood cultures are negative. ### Why Bone Biopsy is Superior Bone biopsy provides: 1. **Microbiological confirmation** — direct culture of bone tissue yields the organism and antibiotic sensitivities 2. **Histopathological evidence** — inflammatory infiltrate, necrosis, and sequestra confirm bone infection 3. **Organism identification** — essential for targeted antimicrobial therapy, especially in culture-negative cases **Clinical Pearl:** In this patient, negative blood cultures do not exclude osteomyelitis. Bone biopsy is indicated when clinical suspicion is high and blood cultures are sterile. ### Investigation Comparison | Investigation | Sensitivity | Specificity | Diagnostic Value | Organism Identification | |---|---|---|---|---| | **Bone Biopsy** | 90–95% | 95–100% | Gold standard | Yes (culture) | | MRI | 90–100% | 75–90% | Excellent for imaging | No | | CT Scan | 70–80% | 75–85% | Good for cortical changes | No | | Tc-99m Bone Scan | 85–90% | 60–70% | Sensitive but non-specific | No | **High-Yield:** Blood cultures are positive in only 50% of acute osteomyelitis cases; bone biopsy is required for definitive diagnosis and organism identification when blood cultures are negative. ### Timing of Biopsy Biopsy should be performed: - **Before starting antibiotics** if possible (to preserve culture yield) - Via percutaneous needle aspiration or open surgical biopsy - Under image guidance (fluoroscopy, ultrasound, or CT) for accuracy **Mnemonic: BONE** — **B**iopsy for **O**rganism identification, **N**ecessary for **E**ffective therapy 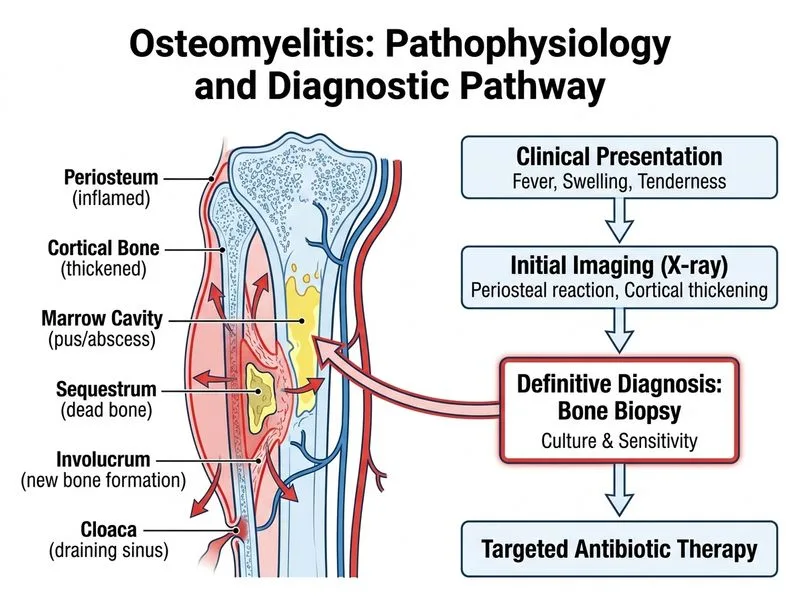
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.