## Clinical Diagnosis This patient has **renal osteodystrophy** secondary to chronic kidney disease, with biochemical and radiological evidence of **secondary hyperparathyroidism** and **high-turnover bone disease (osteitis fibrosa cystica)**. ## Pathophysiology of Renal Osteodystrophy **Key Point:** Renal osteodystrophy is a complex disorder of bone and mineral metabolism in CKD, characterized by abnormalities in calcium, phosphate, PTH, and vitamin D metabolism [cite:Harrison 21e Ch 273]. ### Mechanism in This Patient 1. **Phosphate retention** (eGFR 35): Declining GFR → ↓ phosphate excretion → hyperphosphatemia (5.8 mg/dL) 2. **Secondary hyperparathyroidism**: Hyperphosphatemia + ↓ 1,25(OH)~2~D → ↑ PTH (680 pg/mL, markedly elevated) 3. **High-turnover bone disease**: Excessive PTH stimulates osteoblasts and osteoclasts → increased bone remodeling 4. **Osteitis fibrosa cystica**: Severe PTH-mediated osteoclastic resorption → cystic lesions, marrow fibrosis, and subperiosteal resorption ### Radiological Finding: "Rugger Jersey Spine" **Clinical Pearl:** The "rugger jersey spine" (alternating bands of sclerosis and lucency in vertebral bodies) is pathognomonic for **secondary hyperparathyroidism** in CKD. It reflects: - **Sclerotic bands**: Increased bone density at vertebral endplates (osteosclerosis) - **Lucent bands**: Normal or decreased density in the vertebral body center - **Mechanism**: High PTH → increased osteoblastic activity at endplates + accelerated remodeling ## Histological Classification of Renal Osteodystrophy ```mermaid flowchart TD A[Renal Osteodystrophy]:::outcome A --> B{Bone Turnover Rate}:::decision B -->|High| C[Osteitis Fibrosa Cystica]:::action B -->|Low| D[Adynamic Bone Disease]:::action B -->|Mixed| E[Mixed Uremic Bone Disease]:::action C --> F[↑↑ PTH, ↑ Alkaline Phosphatase]:::outcome D --> G[↓ PTH, ↓ Alkaline Phosphatase]:::outcome E --> H[Variable PTH and Alk Phos]:::outcome ``` ## Biochemical Profile in This Patient | Parameter | Value | Interpretation | |-----------|-------|----------------| | Calcium | 7.2 mg/dL | Low (hypocalcemia) | | Phosphate | 5.8 mg/dL | High (hyperphosphatemia) | | Alkaline Phosphatase | 95 U/L | Normal-to-low (note: bone-specific ALP may be elevated) | | Intact PTH | 680 pg/mL | **Markedly elevated** (normal 15–65) | | eGFR | 35 mL/min | Stage 3b CKD | | DEXA T-score | −2.8 | Osteoporosis by BMD criteria | **High-Yield:** In renal osteodystrophy, **BMD paradox** occurs: DEXA shows low bone density (osteoporosis), but bone turnover is actually **high** (osteitis fibrosa). This is because high PTH causes rapid remodeling with net bone loss, not true osteoporosis. ## Why This Is Osteitis Fibrosa Cystica (Not Simple Osteoporosis) 1. **PTH is markedly elevated (680 pg/mL)**: In primary osteoporosis, PTH is normal or low. 2. **Rugger jersey spine**: Pathognomonic for secondary hyperparathyroidism; absent in primary osteoporosis. 3. **High bone turnover**: Alkaline phosphatase and bone-specific markers would be elevated (reflecting increased osteoblastic activity). 4. **Hypocalcemia + hyperphosphatemia**: Characteristic of CKD-mineral bone disorder, not primary osteoporosis. **Warning:** Do NOT confuse renal osteodystrophy with primary osteoporosis. The presence of secondary hyperparathyroidism (↑ PTH) and high bone turnover distinguishes osteitis fibrosa cystica from osteoporosis. ## Management Principles 1. **Phosphate control**: Dietary restriction, phosphate binders (calcium carbonate, sevelamer, lanthanum) 2. **Vitamin D supplementation**: Calcitriol (active form) or calcifediol to suppress PTH 3. **Calcium supplementation**: Cautiously, to avoid hypercalcemia and vascular calcification 4. **Parathyroid surgery**: If PTH remains >800 pg/mL despite medical therapy 5. **Cinacalcet**: Calcimimetic agent to reduce PTH secretion (if available) **Clinical Pearl:** The goal is to normalize PTH (target 150–300 pg/mL in CKD stage 3–4) to prevent both high-turnover (osteitis fibrosa) and low-turnover (adynamic bone) disease. 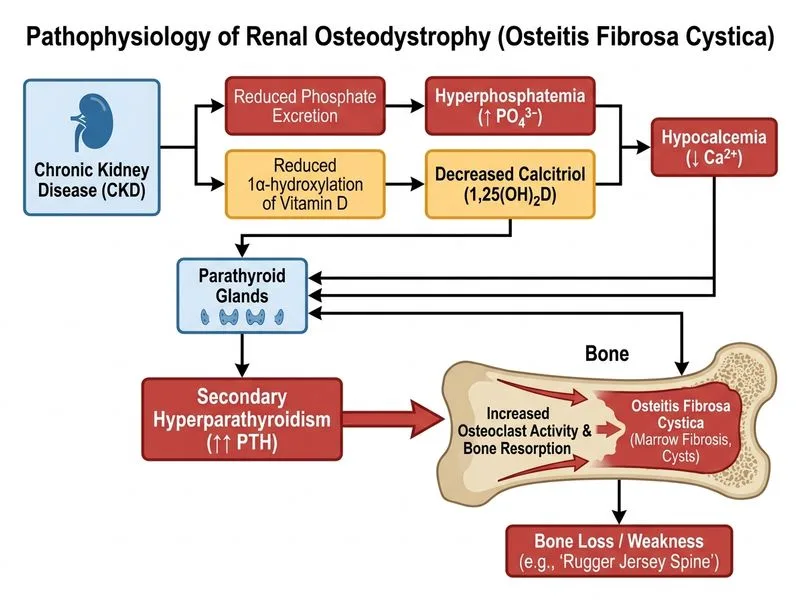
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.