## Investigation of Choice for Osteoporosis Diagnosis **Key Point:** DXA (dual-energy X-ray absorptiometry) is the gold standard investigation for diagnosing osteoporosis and quantifying bone mineral density (BMD). It is the only investigation that provides a T-score, which is used to classify bone health and assess fracture risk. ## Why DXA is the Gold Standard 1. **Diagnostic criterion:** Osteoporosis is defined as a T-score ≤ −2.5 SD at the lumbar spine, femoral neck, or total hip [cite:Park 26e Ch 5] 2. **Sites assessed:** Lumbar spine and femoral neck are the standard measurement sites for fracture risk prediction 3. **Non-invasive and low-radiation:** Minimal radiation exposure compared to CT 4. **Reproducible:** Excellent precision for monitoring treatment response over time 5. **Fracture risk assessment:** FRAX algorithm uses DXA T-score to calculate 10-year fracture probability ## DXA T-Score Classification | T-Score | Classification | 10-Year Fracture Risk | | --- | --- | --- | | > −1.0 | Normal | Low | | −1.0 to −2.5 | Osteopenia | Intermediate | | ≤ −2.5 | Osteoporosis | High | | ≤ −2.5 + fragility fracture | Severe osteoporosis | Very high | **High-Yield:** In postmenopausal women with height loss and kyphosis (clinical vertebral deformity), DXA is mandatory to confirm diagnosis and quantify severity before initiating treatment. **Clinical Pearl:** Height loss >4 cm suggests possible vertebral fracture; DXA should be combined with vertebral fracture assessment (VFA) or spine imaging to detect morphometric fractures. 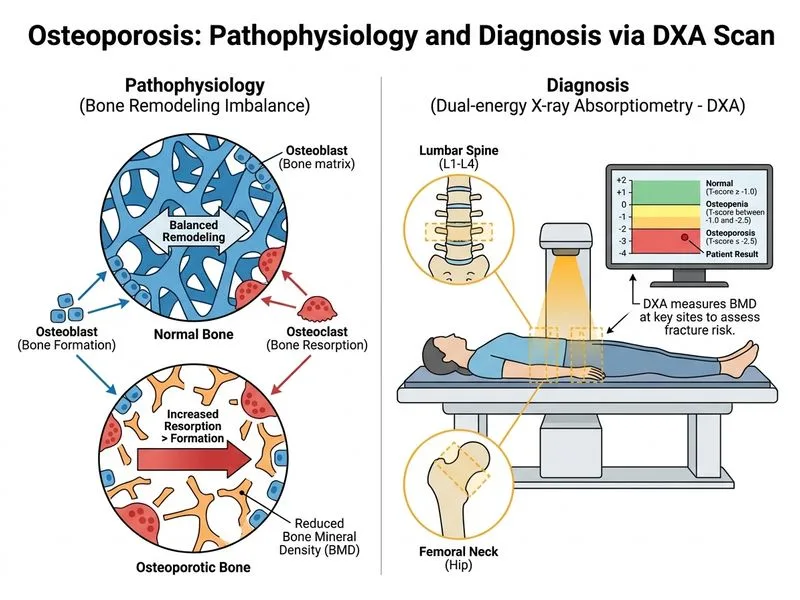
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.