## Differentiating Osteoporosis from Renal Osteodystrophy **Key Point:** In patients with chronic kidney disease (CKD), low bone mineral density on DXA does not distinguish between osteoporosis and renal osteodystrophy (a high-turnover or low-turnover bone disease). Biochemical markers—specifically PTH, calcium, phosphate, and alkaline phosphatase—are essential to differentiate the underlying pathophysiology. ## Pathophysiology of Renal Osteodystrophy Renal osteodystrophy encompasses: 1. **High-turnover disease** (secondary hyperparathyroidism): elevated PTH, high bone turnover 2. **Low-turnover disease** (adynamic bone disease): suppressed PTH, low bone turnover 3. **Mixed uremic osteodystrophy:** intermediate PTH and turnover ## Biochemical Markers in CKD | Parameter | Normal | High-Turnover (2° HPT) | Low-Turnover (Adynamic) | | --- | --- | --- | --- | | PTH | 10–65 pg/mL | **Markedly elevated** (>300 pg/mL) | **Suppressed** (<10 pg/mL) | | Alkaline phosphatase | 30–120 IU/L | **Elevated** | Normal/low | | Serum calcium | 8.5–10.5 mg/dL | Low (due to hyperphosphatemia) | Normal/high | | Serum phosphate | 2.5–4.5 mg/dL | **Elevated** | Elevated | | Bone-specific ALP | <20 µg/L | **Elevated** | Low | **High-Yield:** KDIGO guidelines recommend measuring PTH, calcium, phosphate, and alkaline phosphatase in all CKD patients with low BMD to classify the type of renal osteodystrophy and guide treatment (e.g., vitamin D, calcimimetics, phosphate binders) [cite:KDIGO 2017]. **Mnemonic:** **CAPH** — Calcium, Alkaline Phosphatase, Phosphate, and PTH (Hormone) — the four key biochemical markers in renal bone disease. **Clinical Pearl:** A PTH level >300 pg/mL in a CKD patient with low BMD suggests high-turnover disease requiring PTH suppression; a PTH <10 pg/mL suggests adynamic disease, where aggressive PTH suppression is harmful. 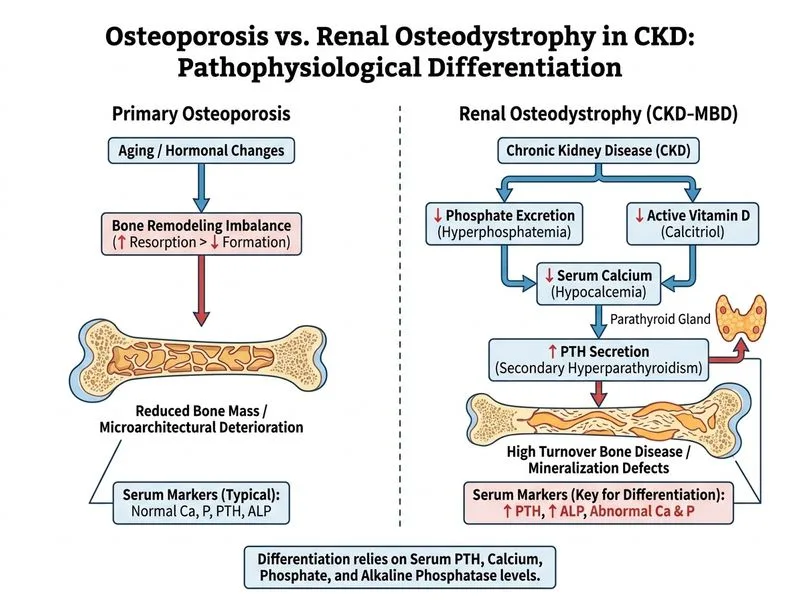
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.