## Clinical Scenario Analysis This patient has: - **Osteoporosis** (T-score ≤ −2.5) - **Prior fragility fracture** (distal radius) — indicates high fracture risk - **Elevated FRAX scores** (major fracture 18%, hip fracture 8%) — above treatment thresholds - **Vitamin D deficiency** (28 ng/mL) — modifiable risk factor ## Management Hierarchy **Key Point:** The presence of a prior fragility fracture is the single strongest indicator for pharmacotherapy. Combined with osteoporosis on DEXA, this patient meets criteria for anti-osteoporotic drug therapy regardless of FRAX score. ## Treatment Algorithm ```mermaid flowchart TD A[Osteoporosis + prior fragility fracture]:::outcome --> B{Vitamin D adequate?}:::decision B -->|No| C[Supplement vitamin D₃ 1000-2000 IU daily]:::action B -->|Yes| D[Proceed to pharmacotherapy] C --> E[Recheck 25-OH vitamin D in 6-8 weeks]:::action E --> D D --> F{First-line agent?}:::decision F -->|Bisphosphonate| G[Alendronate 70 mg weekly or Risedronate 35 mg weekly]:::action F -->|Contraindication to BP| H[Consider teriparatide or denosumab]:::action G --> I[Counsel on adherence and side effects]:::action H --> I ``` ## Why Alendronate (Bisphosphonate) is First-Line | Feature | Bisphosphonate | Teriparatide | Denosumab | |---------|---|---|---| | **First-line status** | Yes | No (reserved for severe/refractory cases) | No (second-line) | | **Mechanism** | Inhibits osteoclast-mediated resorption | Stimulates osteoblast-mediated formation | RANKL inhibitor; reduces osteoclasts | | **Fracture reduction** | 50% reduction in vertebral, 25–30% in hip | 65% reduction in vertebral | 40% reduction in vertebral | | **Cost** | Low; generic available | Very high | High | | **Renal function requirement** | GFR ≥ 35 mL/min | GFR ≥ 30 mL/min | GFR ≥ 30 mL/min | | **Use in prior fracture** | Yes, standard | Yes, if severe/refractory | Yes, if intolerant to BP | **High-Yield:** Bisphosphonates are the **gold standard first-line agents** for osteoporosis with prior fragility fracture. Teriparatide is reserved for: - Severe osteoporosis with multiple vertebral fractures - Failure or intolerance to bisphosphonates - Glucocorticoid-induced osteoporosis **Clinical Pearl:** Vitamin D deficiency (< 30 ng/mL) must be corrected **before** or **concurrent with** bisphosphonate initiation. Delaying pharmacotherapy while correcting vitamin D is acceptable only if the patient is at very low fracture risk; this patient is NOT low-risk (prior fracture + elevated FRAX). ## Correct Management Sequence 1. **Immediately:** Start vitamin D₃ 1000–2000 IU daily + elemental calcium 1000–1200 mg daily 2. **Concurrent or within 6–8 weeks:** Initiate alendronate 70 mg weekly (or risedronate 35 mg weekly) 3. **Counseling:** Upright posture for 30 minutes post-dose, avoid lying down, take on empty stomach 4. **Follow-up:** Repeat DEXA in 2 years; assess adherence and side effects at 6–12 months [cite:Harrison 21e Ch 397; Park 26e Ch 7] 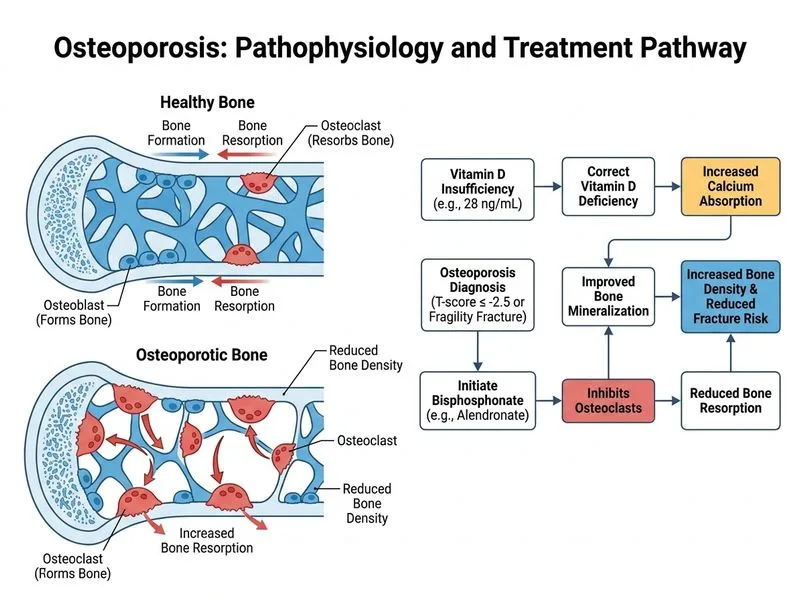
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.