## Distinguishing Postmenopausal from Senile (Age-Related) Osteoporosis ### Classification and Epidemiology **Key Point:** Osteoporosis is classified into **Type I (postmenopausal)** and **Type II (senile/age-related)**. The primary discriminator is the **rate and pattern of bone loss**, not just the final T-score. ### Comparative Features Table | Feature | Postmenopausal (Type I) | Senile/Age-Related (Type II) | |---------|------------------------|------------------------------| | **Age of onset** | 50–65 years (within 5–10 yrs of menopause) | >70 years | | **Rate of bone loss** | Rapid (2–3% per year in first 5–10 yrs) | Slow and steady (0.3–0.5% per year) | | **Primary site** | Trabecular bone (vertebrae, distal radius) | Both trabecular and cortical | | **Fracture pattern** | Vertebral compression, Colles' fracture | Hip (femoral neck), vertebral, pelvis | | **Pathophysiology** | Estrogen deficiency → ↑ osteoclast activity | Decreased osteoblast function + secondary hyperparathyroidism | | **PTH level** | Normal | Often elevated (secondary) | | **Calcium absorption** | Normal | Decreased (age-related) | | **Sex ratio** | Female >> Male | Female:Male ≈ 2:1 (less female-predominant) | ### Why Rate of Bone Loss Is the Best Discriminator **High-Yield:** The **accelerated bone loss in the first 5–10 years after menopause** is pathognomonic for Type I osteoporosis. This rapid phase is driven by estrogen withdrawal and increased osteoclast activity. Senile osteoporosis, by contrast, shows a gradual, linear decline in bone mass over decades, reflecting cumulative effects of aging, decreased osteoblast function, and secondary hyperparathyroidism. **Clinical Pearl:** A woman who develops a vertebral fracture at age 55 (5 years post-menopause) with rapid T-score decline is Type I. A woman with gradual bone loss presenting at age 75 is Type II. The **temporal pattern** matters as much as the absolute T-score. **Mnemonic:** **FAST Type I, SLOW Type II** — Postmenopausal (Type I) bone loss is **FAST** in the first decade; Senile (Type II) bone loss is **SLOW** and steady throughout life. ### Pathophysiological Basis 1. **Postmenopausal:** Estrogen ↓ → RANKL ↑ → osteoclast activation → rapid trabecular bone resorption. 2. **Senile:** Osteoblast dysfunction (age-related) + secondary hyperparathyroidism (due to decreased intestinal calcium absorption and renal 1,25-diOH D production) → slow, progressive loss of both trabecular and cortical bone. ### Clinical Implications - **Postmenopausal women:** Benefit most from **antiresorptive agents** (bisphosphonates, HRT, denosumab) during the rapid-loss phase. - **Elderly (senile):** May need **anabolic agents** (teriparatide) or combination therapy due to osteoblast dysfunction. 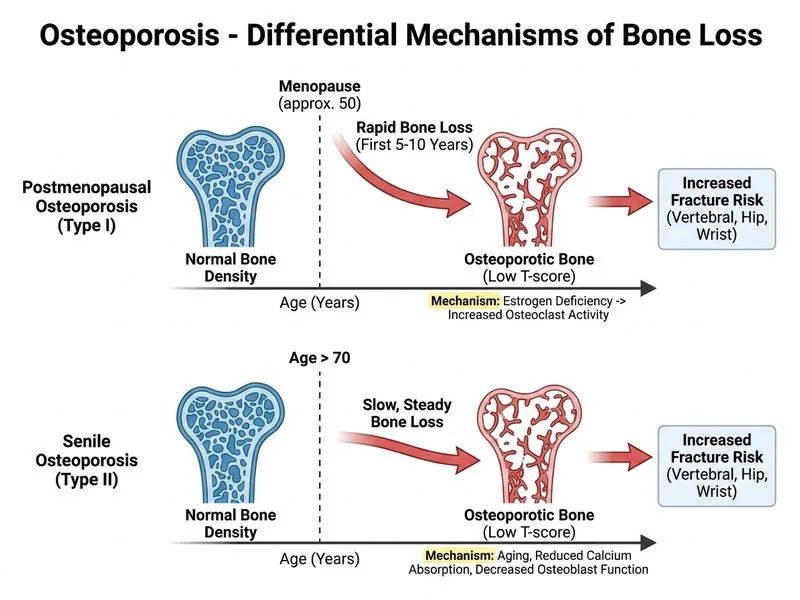
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.