## Pathophysiology of Postmenopausal Osteoporosis **Key Point:** Estrogen is a potent inhibitor of osteoclast activity. When estrogen levels drop sharply after menopause, osteoclasts become hyperactive, leading to accelerated bone resorption that outpaces bone formation. ### Mechanism Estrogen normally: - Inhibits production of pro-resorptive cytokines (IL-6, TNF-α, RANKL) by osteoblasts and immune cells - Enhances osteoclast apoptosis - Promotes osteoprotegerin (OPG) expression, which blocks RANKL signaling When estrogen is withdrawn: 1. Osteoclast precursors differentiate more readily 2. Osteoclast lifespan increases 3. Bone resorption accelerates (especially in trabecular bone) 4. Osteoblast activity remains relatively unchanged or decreases slightly **High-Yield:** The bone loss in postmenopausal osteoporosis is **resorption-driven**, not formation-driven. This is why antiresorptive agents (bisphosphonates, denosumab) are first-line therapy. ### Why This Differs from Other Causes | Cause | Primary Defect | |-------|----------------| | Postmenopausal | ↑ Osteoclast activity (estrogen loss) | | Hypogonadism (male) | ↑ Osteoclast activity (androgen loss) | | Vitamin D deficiency | ↓ Mineralization + secondary hyperparathyroidism | | Growth hormone deficiency | ↓ Osteoblast activity | | Hyperparathyroidism | ↑ Osteoclast activity + ↓ renal phosphate reabsorption | **Clinical Pearl:** Postmenopausal bone loss is most rapid in the first 5–10 years after menopause, when the resorption-to-formation imbalance is greatest. This window is critical for intervention. [cite:Harrison 21e Ch 397] 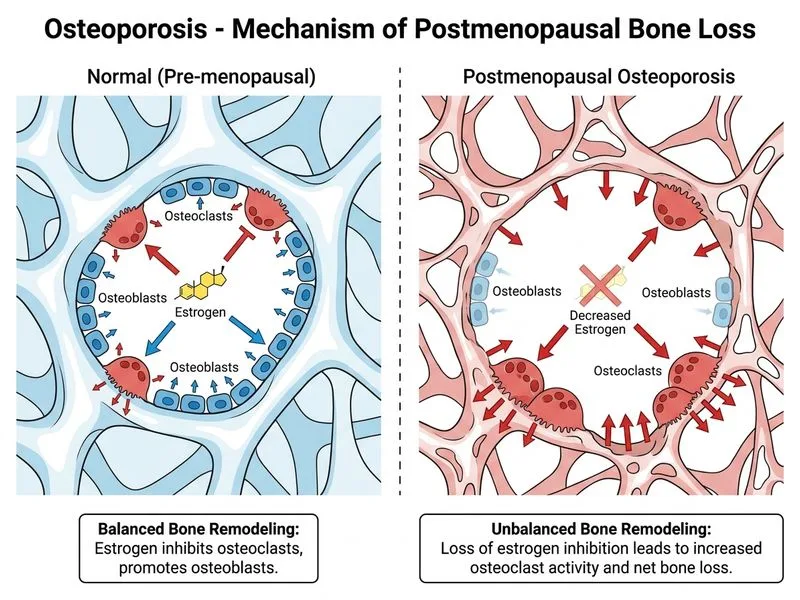
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.