## Diagnosis: Osteoporosis with Pathological Fracture ### Clinical Presentation This patient presents with classic features of postmenopausal osteoporosis: - **Age and sex:** 62-year-old postmenopausal woman (peak bone loss occurs in first 5–10 years after menopause) - **Progressive height loss and kyphosis:** hallmark of multiple vertebral fractures - **Fragility fracture:** compression fracture from minor trauma (fall from standing height) - **Vertebral location:** thoracolumbar spine is the most common site for osteoporotic fractures ### Biochemical Profile | Parameter | Value | Interpretation | |-----------|-------|----------------| | Serum calcium | 8.8 mg/dL | Normal (8.5–10.5) | | Phosphate | 3.5 mg/dL | Normal (2.5–4.5) | | Alkaline phosphatase | 68 U/L | Normal (30–120) | | 25-OH vitamin D | 28 ng/mL | Insufficient (20–29 ng/mL) | | PTH | Not mentioned but likely normal | Rules out secondary osteoporosis | **Key Point:** Normal serum calcium, phosphate, and alkaline phosphatase rule out osteomalacia (which shows hypocalcemia, hyperphosphatemia, and elevated alkaline phosphatase) and metabolic bone disease. ### DEXA Scan Interpretation **High-Yield:** WHO diagnostic criteria for bone mineral density: - **Normal:** T-score ≥ −1.0 - **Osteopenia:** T-score between −1.0 and −2.5 - **Osteoporosis:** T-score ≤ −2.5 (with or without fracture) - **Severe osteoporosis:** T-score ≤ −2.5 + fragility fracture This patient's T-scores (−2.8 lumbar spine, −2.5 femoral neck) meet diagnostic criteria for osteoporosis. The presence of a fragility fracture confirms **severe osteoporosis**. ### Radiographic Features **Clinical Pearl:** Osteoporotic vertebral fractures typically show: - Wedge-shaped deformity (anterior height loss > posterior) - Biconcave ("codfish") vertebrae from disc herniation - Loss of trabecular density - No sclerotic margins (unlike metastatic disease) ### Pathophysiology 1. **Estrogen deficiency** → ↑ osteoclast activity and ↓ osteoblast function 2. **Accelerated bone resorption** > bone formation 3. **Net loss of bone mineral density** → ↓ mechanical strength 4. **Fragility fractures** from minimal trauma --- ## Why Other Options Are Incorrect ### Osteomalacia (Option 1 — WRONG) - Would show **hypocalcemia** (this patient has normal calcium) - Would show **elevated alkaline phosphatase** (this patient's is normal) - Would show **elevated PTH** (secondary hyperparathyroidism) - 25-OH vitamin D is low-normal (28 ng/mL), not severely deficient (<20 ng/mL) - Biochemical profile is inconsistent with osteomalacia ### Multiple Myeloma (Option 2 — WRONG) - Presents with **lytic lesions** (punched-out, round lesions), not compression fractures - Would show **hypercalcemia** (from osteoclast-activating factors) - Would have **elevated serum/urine protein** and **Bence Jones proteinuria** - Would show **anemia, renal dysfunction, elevated creatinine** - No mention of constitutional symptoms (fever, fatigue, recurrent infections) ### Paget's Disease of Bone (Option 3 — WRONG) - Typically presents with **elevated alkaline phosphatase** (often markedly elevated, >500 U/L) - Shows **mixed lytic and sclerotic lesions** on radiographs, not simple compression fractures - Usually **monostotic or oligostotic** (affects 1–2 bones), not generalized - More common in elderly males (>70 years) - DEXA findings would show **increased bone density** in affected areas, not generalized osteoporosis --- ## Management Approach **Mnemonic: ABCDE of Osteoporosis Management** - **A**ssess risk factors and fracture risk (FRAX score) - **B**one density monitoring (DEXA baseline, repeat every 2 years) - **C**alcium and vitamin D supplementation (1200 mg/day calcium, 800–1000 IU/day vitamin D) - **D**rug therapy: bisphosphonates (alendronate), HRT, SERM (raloxifene), denosumab - **E**xercise and lifestyle modification (weight-bearing activity, smoking cessation, fall prevention) **High-Yield:** First-line pharmacotherapy is **alendronate 70 mg weekly** or **risedronate 35 mg weekly** (bisphosphonates inhibit osteoclast-mediated bone resorption). 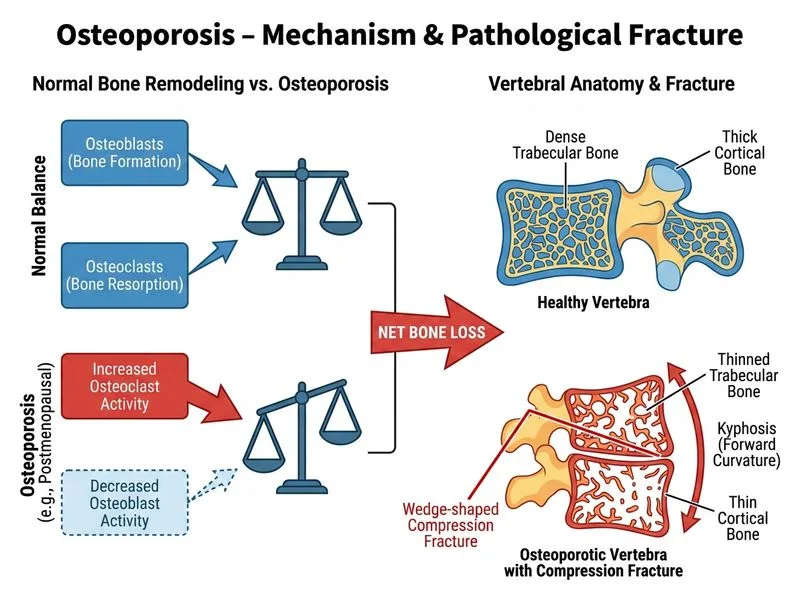
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.