## Clinical Scenario: Osteoporotic Vertebral Fracture with Spinal Cord Compression ### Diagnosis and Pathophysiology **High-Yield:** This patient has **secondary osteoporosis** due to: 1. **Chronic corticosteroid use** (prednisolone 7.5 mg/day × 8 years) - Suppresses osteoblast function - Increases osteoclast activity - Impairs intestinal calcium absorption - Causes rapid bone loss (1–3% per year) 2. **Chronic inflammatory disease** (RA) - Inflammatory cytokines (TNF-α, IL-6) promote osteoclastogenesis - Systemic inflammation accelerates bone resorption 3. **Malnutrition** (low albumin 3.2 g/dL, low BMI 19 kg/m²) - Reduced protein substrate for bone matrix synthesis - Poor nutritional reserve ### Critical Finding: Spinal Cord Compression **Key Point:** The presence of **cord compression on MRI** is the decisive factor that mandates **surgical intervention**. This is NOT a simple osteoporotic fracture — it is a **surgical emergency**. #### Why Cord Compression Changes Management | Feature | Non-Compressive Fracture | Compressive Fracture | |---------|--------------------------|---------------------| | **Neurological deficit** | Absent | Present (pain, paresthesia, weakness, paralysis) | | **Imaging finding** | Fracture only | Fracture + cord compression/myelopathy | | **Management** | Conservative (rest, analgesia, bone-protective drugs) | **Surgical decompression** | | **Urgency** | Routine | **EMERGENT** | | **Goal** | Prevent further fractures | Prevent permanent neurological damage | **Clinical Pearl:** Retropulsion of bone into the spinal canal (as described in this case) causes mechanical compression of the spinal cord. Delayed decompression risks permanent paraplegia. ### Surgical Management Algorithm ```mermaid flowchart TD A[Osteoporotic vertebral fracture]:::outcome --> B{Spinal cord compression?}:::decision B -->|No| C[Conservative management]:::action C --> D[Rest, analgesia, bisphosphonates]:::action B -->|Yes| E{Neurological deficit?}:::decision E -->|Mild/moderate| F[Consider decompression]:::action E -->|Severe/progressive| G[URGENT surgical decompression]:::urgent G --> H[Laminectomy ± anterior vertebrectomy]:::action H --> I[Spinal stabilization]:::action I --> J[Prevent permanent neurological damage]:::outcome ``` ### Why Vertebroplasty Is Inappropriate Here **Warning:** Vertebroplasty (Option 3) is contraindicated when: - **Cord compression is present** — cement injection can worsen compression - **Neurological deficit exists** — risk of permanent paralysis - **Retropulsion of bone** — mechanical obstruction requires removal, not cement filling Vertebroplasty is reserved for **painful osteoporotic fractures WITHOUT neurological compromise**. --- ## Why Each Option Is Correct or Wrong ### Option 0: Immediate Spinal Decompression and Stabilization Surgery — **CORRECT** **Reasoning:** 1. **Cord compression on MRI** is the absolute indication for surgery 2. **Retropulsion of bone** requires mechanical removal via laminectomy or corpectomy 3. **Severe loss of vertebral body height** necessitates anterior stabilization (cage, graft, or instrumentation) 4. **Urgency:** Delayed decompression risks irreversible neurological damage (paraplegia) 5. **Surgical approach:** Posterior laminectomy for decompression + anterior vertebrectomy and fusion for stability **Key Point:** In osteoporotic fractures with cord compression, **surgery is NOT optional** — it is the standard of care to prevent permanent disability. --- ### Option 1: High-Dose Intravenous Bisphosphonate Therapy — **WRONG** **Why this is incorrect:** - Bisphosphonates (e.g., zoledronic acid) are **bone-protective agents** that slow further bone loss - They do **NOT reverse existing fractures** or decompress the spinal cord - They do **NOT address the acute mechanical compression** of the cord - **Timeline:** Bisphosphonates take weeks to months to show effect; cord compression is an immediate threat - **Mechanism:** Bisphosphonates inhibit osteoclasts → they prevent future fractures, not current neurological emergency - **Appropriate role:** Bisphosphonates are **adjunctive therapy AFTER surgical stabilization** to prevent recurrent fractures **Clinical Pearl:** Bisphosphonates are for **prevention and treatment of uncomplicated osteoporosis**, not for surgical emergencies. --- ### Option 2: Increase Prednisolone Dose and Start Calcium + Vitamin D — **WRONG** **Why this is incorrect:** - **Increasing corticosteroids** would **worsen osteoporosis** (accelerate bone loss further) - **Calcium + vitamin D alone** cannot decompress the spinal cord or stabilize the fracture - **No neurological benefit:** These are preventive measures, not acute interventions - **Dangerous:** Delaying surgery while starting medical therapy risks permanent paraplegia - **Appropriate role:** Calcium + vitamin D are **adjunctive** after surgery, not primary treatment **Warning:** Increasing corticosteroid dose in a patient with corticosteroid-induced osteoporosis is contraindicated and harmful. --- ### Option 3: Percutaneous Vertebroplasty — **WRONG** **Why this is incorrect:** - **Absolute contraindication:** Cord compression is a contraindication to vertebroplasty - **Mechanism of harm:** Cement injection can: - Worsen mechanical compression - Cause thermal injury to cord - Increase intradiscal pressure - Exacerbate neurological deficit - **Inadequate decompression:** Vertebroplasty does NOT remove retropulsed bone; it only fills the fracture cavity - **Appropriate use:** Vertebroplasty is for **painful osteoporotic fractures WITHOUT neurological signs** **Clinical Pearl:** Vertebroplasty is a **pain-relief procedure**, not a decompression procedure. When cord compression exists, **open surgical decompression is mandatory**. --- ## Post-Operative Management **High-Yield:** After surgical decompression and stabilization: 1. **Bone-protective therapy:** - Bisphosphonate (alendronate 70 mg weekly or zoledronic acid 5 mg IV annually) - Denosumab (60 mg SC every 6 months) — alternative if bisphosphonate intolerant 2. **Calcium and vitamin D supplementation:** - Calcium 1200 mg/day - Vitamin D 800–1000 IU/day (higher doses if deficient) 3. **Corticosteroid optimization:** - Taper prednisolone to lowest effective dose for RA control - Consider alternative immunosuppressants (methotrexate, biologics) to reduce steroid dependence 4. **Nutritional support:** - Protein supplementation (target 1.2–1.5 g/kg/day) - Address malnutrition to optimize fracture healing 5. **Physical rehabilitation:** - Early mobilization post-operatively - Spinal stabilization exercises - Fall prevention strategies **Mnemonic: CADS for Secondary Osteoporosis Management** - **C**orticosteroid minimization - **A**ddress underlying disease (RA control) - **D**rug therapy (bisphosphonates, denosumab) - **S**urgery (when neurological compromise exists) 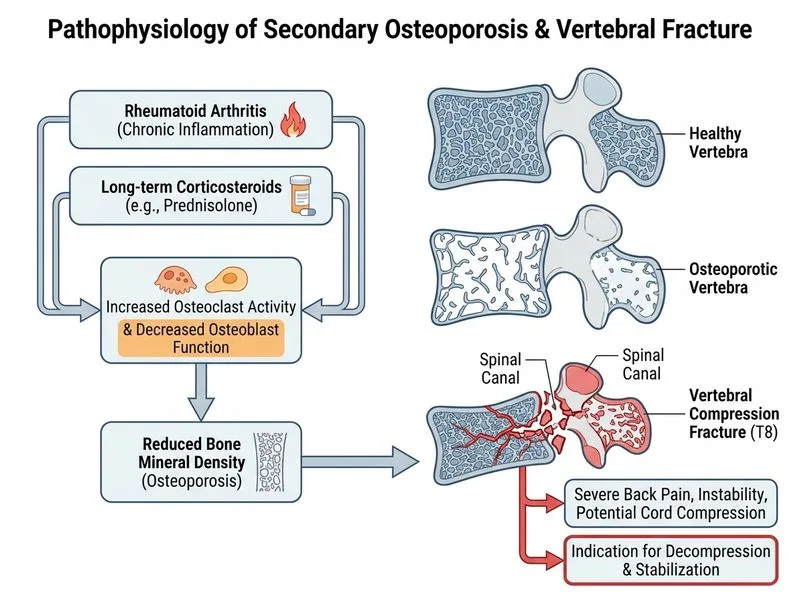
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.