## Clinical Context This patient has **concurrent osteoporosis and chronic kidney disease (CKD) stage 3b with secondary hyperparathyroidism (sHPT)**. The elevated PTH (120 pg/mL) and hyperphosphatemia indicate mineral-bone disorder (MBD), which alters the management approach to osteoporosis. ## Key Distinction: Osteoporosis vs. CKD-MBD | Feature | Osteoporosis (Non-CKD) | CKD-MBD with sHPT | |---------|------------------------|-------------------| | Bone pathology | Low bone mass | Mixed: low turnover + high turnover | | PTH level | Normal | Elevated | | Phosphate | Normal | Elevated | | Bisphosphonate safety | Safe (eGFR ≥ 30) | Contraindicated in sHPT | | Denosumab safety | Safe | **Contraindicated** (risk of severe hypocalcemia) | | First step | Pharmacotherapy | Manage MBD first | ## High-Yield: Why Bisphosphonates Are Contraindicated Here **Key Point:** **Bisphosphonates suppress bone turnover and are contraindicated in secondary hyperparathyroidism** because they worsen the imbalance and increase risk of adynamic bone disease (low-turnover osteoporosis). ## High-Yield: Why Denosumab Is Contraindicated **Key Point:** **Denosumab (RANKL inhibitor) is contraindicated in CKD stage 4–5 and in patients with sHPT** due to: - Risk of severe, refractory hypocalcemia - Suppression of bone turnover in an already dysregulated system - Limited safety data in this population ## Management Algorithm for CKD-MBD with Osteoporosis ```mermaid flowchart TD A[CKD stage 3-5 + Osteoporosis]:::outcome --> B{PTH elevated?}:::decision B -->|Yes, sHPT present| C[Manage mineral-bone disorder FIRST]:::action B -->|No, PTH normal| D[Proceed with bisphosphonate if eGFR ≥ 30]:::action C --> E[Optimize phosphate, calcium, vitamin D/calcitriol]:::action E --> F[Refer to nephrology]:::action F --> G{MBD controlled?}:::decision G -->|Yes| H[Then consider osteoporosis therapy cautiously]:::action G -->|No| I[Continue MBD management]:::action ``` ## Clinical Pearl: **Calcitriol (active vitamin D) is the appropriate first step** in this patient because: - Suppresses PTH (addresses sHPT) - Improves calcium absorption - Corrects hypocalcemia (Ca 8.2) - Allows optimization of phosphate control before osteoporosis-specific agents ## Why Deferring Osteoporosis Therapy Is Correct 1. **Mineral-bone disorder must be controlled first** to avoid worsening bone turnover dysregulation 2. **Nephrology referral is essential** for coordinated management of CKD-MBD 3. **Once MBD is stabilized**, osteoporosis therapy (if still indicated) can be reconsidered with caution 4. **This patient's fracture risk is lower than his MBD risk** — preventing adynamic bone disease takes priority ## Monitoring Parameters - Serum calcium, phosphate, PTH every 3 months during MBD optimization - Repeat DEXA and reassess osteoporosis therapy once PTH and phosphate are in target range - Target PTH for CKD stage 3b: 35–70 pg/mL (higher than non-CKD osteoporosis) [cite:KDIGO 2017 Clinical Practice Guideline for CKD-MBD; Harrison 21e Ch 405] 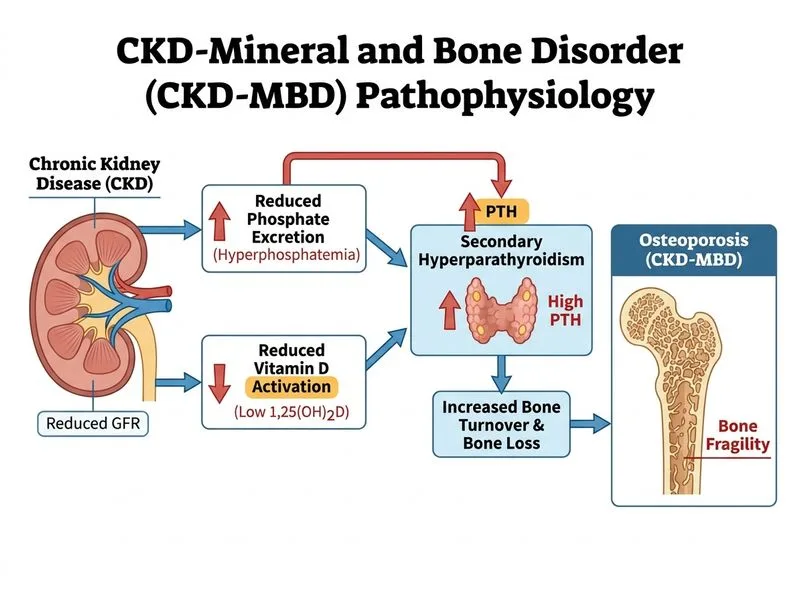
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.