## Distinguishing Osteoporosis from Osteomalacia ### Biochemical Profile Comparison | Feature | Osteoporosis | Osteomalacia | |---------|--------------|---------------| | **Serum Calcium** | Normal or slightly low | Low (hypocalcemia) | | **Serum Phosphate** | Normal | Low (hypophosphatemia) | | **Alkaline Phosphatase** | Normal | Elevated | | **25-OH Vitamin D** | Normal (>20 ng/mL) | Low (<20 ng/mL) | | **Bone Density (T-score)** | ≤−2.5 | Often normal or mild decrease | | **Histology** | Normal mineralization, reduced bone mass | Defective mineralization | ### Key Discriminating Feature **Key Point:** The combination of **elevated alkaline phosphatase with hypophosphatemia and hypocalcemia** is the hallmark biochemical signature of osteomalacia and distinguishes it from osteoporosis, where these values remain normal. **High-Yield:** In osteomalacia, defective mineralization triggers secondary hyperparathyroidism, leading to: 1. Increased bone turnover (↑ alkaline phosphatase) 2. Phosphate wasting by kidneys (↓ phosphate) 3. Compensatory calcium mobilization (but still low due to malabsorption) **Clinical Pearl:** A postmenopausal woman with osteoporosis typically has normal serum calcium, phosphate, and alkaline phosphatase — the bone loss is purely quantitative (reduced mass), not qualitative (normal mineralization). The man in this vignette with low calcium, low phosphate, and elevated alkaline phosphatase has osteomalacia (likely vitamin D deficiency). **Mnemonic:** **CAMP** = **C**alcium low, **A**lkaline phosphatase elevated, **M**ineralization defective, **P**hosphate low — osteomalacia signature. ### Why This Matters Osteoporosis requires calcium/vitamin D supplementation and antiresorptive agents (bisphosphonates, denosumab). Osteomalacia requires **vitamin D repletion** — treating osteomalacia as osteoporosis alone will not correct the mineralization defect and may worsen secondary hyperparathyroidism. 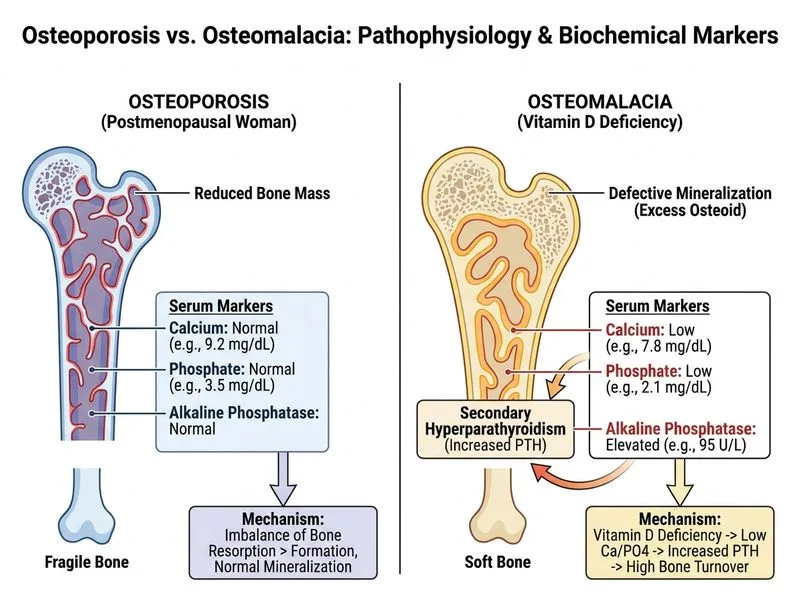
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.