## Primary vs. Secondary Osteoporosis (Steroid-Induced) ### Pathophysiological Differences | Feature | Primary Osteoporosis | Steroid-Induced Osteoporosis | |---------|---------------------|------------------------------| | **Bone Loss Pattern** | Trabecular > cortical (but both affected) | **Trabecular >> cortical** (preferential) | | **Onset** | Gradual (years) | Rapid (months) | | **Bone Turnover** | Low-to-normal | **Suppressed (low)** | | **Alkaline Phosphatase** | Normal | Low-normal | | **Fracture Type** | Vertebral, hip, wrist | **Vertebral (early & severe)** | | **Mechanism** | Estrogen deficiency (postmenopausal) | Glucocorticoid-induced osteoblast apoptosis | ### Key Discriminating Feature **Key Point:** Steroid-induced osteoporosis causes **preferential loss of trabecular bone with relative preservation of cortical bone**, whereas primary osteoporosis affects both compartments more uniformly. This pattern is visible on high-resolution CT and is a hallmark radiological discriminator. **High-Yield:** Glucocorticoids suppress osteoblast function and increase osteocyte apoptosis, leading to: - Rapid bone loss in the first 3–6 months of therapy - Predominantly trabecular involvement (trabecular bone is more metabolically active) - Low bone turnover state (not high turnover like postmenopausal osteoporosis) **Clinical Pearl:** A patient on chronic corticosteroids who develops vertebral compression fractures within months of starting therapy should raise suspicion for steroid-induced osteoporosis. The fractures are often multiple and severe despite modest T-score reductions. **Mnemonic:** **STAB** = **S**teroid-induced, **T**rabecular loss (preferential), **A**cute onset, **B**one turnover suppressed. 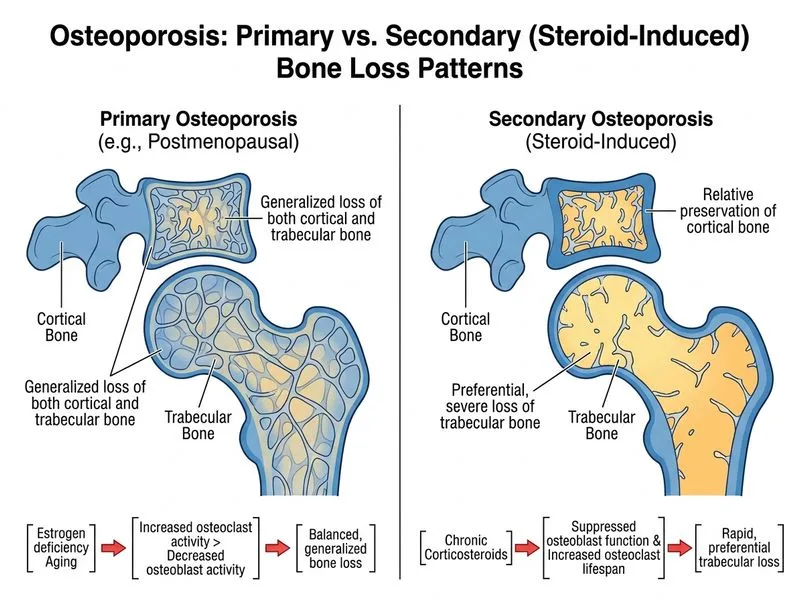
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.