## Diagnostic Workup for Suspected Osteosarcoma **Key Point:** Once osteosarcoma is suspected on plain radiographs (mixed lytic-sclerotic lesion, cortical destruction, Codman triangle), the next step is **MRI for local staging** followed by **core needle biopsy for tissue diagnosis**—NOT incisional biopsy, and NOT immediate surgery. ### Why MRI + Core Needle Biopsy? 1. **MRI provides:** - Precise soft tissue extension - Intramedullary extent - Relationship to neurovascular structures - Essential for surgical planning (wide margins) 2. **Core needle biopsy (CNB):** - Minimally invasive - Diagnostic accuracy >95% - Avoids seeding tumor along biopsy tract (unlike open incisional biopsy) - Can be performed under image guidance (US or CT) ### Staging Sequence ```mermaid flowchart TD A[Suspected osteosarcoma on plain X-ray]:::outcome --> B[MRI of primary site]:::action B --> C[Core needle biopsy]:::action C --> D{Histology confirms osteosarcoma?}:::decision D -->|Yes| E[Chest CT + whole-body PET-CT]:::action D -->|No| F[Reassess diagnosis]:::outcome E --> G[Neoadjuvant chemotherapy]:::action ``` **High-Yield:** The sequence is **MRI → CNB → systemic staging (CT chest + PET-CT) → chemotherapy → surgery**. Incisional biopsy risks tumor seeding and is contraindicated. Immediate surgery without staging or histology is malpractice. **Clinical Pearl:** Elevated alkaline phosphatase in a young patient with metaphyseal bone pain and radiographic features of osteosarcoma is highly suggestive; it reflects osteoid production by tumor cells. [cite:Rockwood and Green's Fractures in Adults 9e Ch 32] 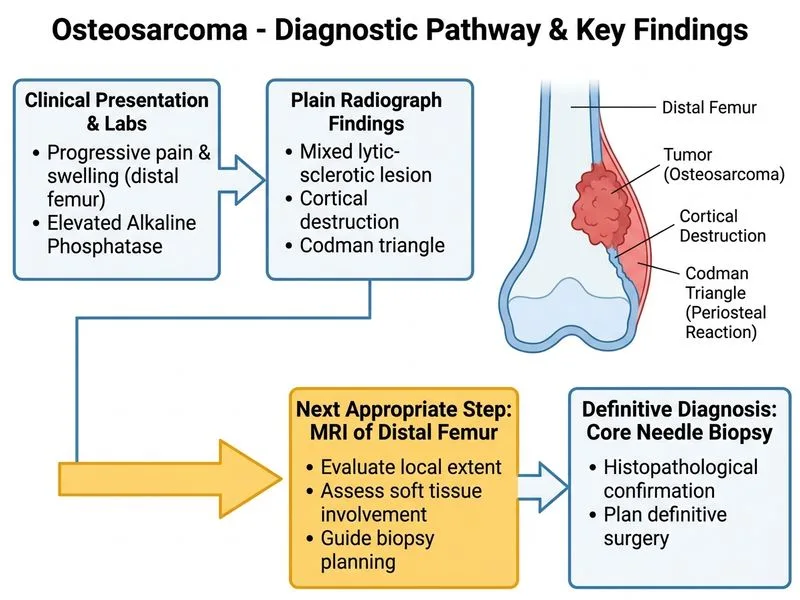
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.