## Management of Osteosarcoma: Neoadjuvant Approach ### Current Standard of Care **Key Point:** The modern treatment paradigm for osteosarcoma is **neoadjuvant chemotherapy followed by wide surgical resection and adjuvant chemotherapy**. This approach has revolutionized outcomes, improving 5-year survival from ~10% (surgery alone) to ~60–70% (multimodal therapy). **High-Yield:** Neoadjuvant chemotherapy serves three critical functions: 1. **Systemic control** — targets occult micrometastases (present in ~80% of patients at diagnosis). 2. **Tumor downsizing** — may convert an unresectable lesion to resectable. 3. **Prognostic assessment** — histologic response to chemotherapy predicts overall survival (good responders: >90% necrosis have better prognosis). ### Rationale for Neoadjuvant Approach ```mermaid flowchart TD A[Newly diagnosed osteosarcoma]:::outcome --> B[Staging: Chest CT, MRI primary]:::action B --> C[Resectable tumor?]:::decision C -->|Yes| D[Neoadjuvant chemotherapy<br/>8-12 weeks]:::action C -->|No| E[Consider neoadjuvant therapy<br/>to downsize]:::action D --> F[Reassess with MRI]:::action E --> F F --> G[Wide surgical resection]:::action G --> H[Histologic response assessment]:::outcome H --> I[Adjuvant chemotherapy<br/>based on response]:::action I --> J[Long-term surveillance]:::action ``` ### Chemotherapy Regimens | Agent | Mechanism | Role | Notes | |-------|-----------|------|-------| | **Doxorubicin** | Topoisomerase II inhibitor | Neoadjuvant + adjuvant | Cardiotoxicity monitoring required | | **Cisplatin** | DNA cross-linking | Neoadjuvant + adjuvant | Nephrotoxicity, ototoxicity | | **Methotrexate** (high-dose) | DHFR inhibitor | Neoadjuvant + adjuvant | Requires leucovorin rescue | | **Ifosfamide** | Alkylating agent | Salvage therapy | Used in poor responders | **Mnemonic:** **MAP** = **M**ethotrexate, **A**driaymycin (doxorubicin), **P**latin (cisplatin) — the classic backbone regimen. ### Surgical Resection **Key Point:** Wide surgical resection with adequate margins (typically 5–10 cm) is mandatory. Limb-salvage surgery is preferred over amputation when feasible and achieves equivalent survival. **Clinical Pearl:** The extent of surgical margins and histologic response to neoadjuvant therapy are the strongest predictors of local recurrence and overall survival. ### Prognostic Factors | Factor | Good Prognosis | Poor Prognosis | |--------|----------------|----------------| | **Chemotherapy response** | >90% necrosis | <90% necrosis | | **Tumor size** | <8 cm | >8 cm | | **Site** | Distal femur, proximal tibia | Pelvis, spine, proximal humerus | | **Metastases at diagnosis** | Absent | Present (especially >3 pulmonary nodules) | | **Age** | Younger | Older | ### Why NOT Other Options **High-Yield:** Surgery alone (without chemotherapy) results in ~90% mortality within 5 years due to early micrometastatic disease. Chemotherapy is non-negotiable. **Warning:** Amputation without chemotherapy is obsolete and unethical in the modern era. Limb-salvage with chemotherapy achieves equivalent or superior survival compared to amputation. ### Surveillance After Treatment - **Chest imaging** (CT or X-ray) every 3 months for 2 years, then every 6 months. - **Local site imaging** (X-ray or MRI) every 6 months. - **Serum alkaline phosphatase and LDH** — may indicate recurrence if elevated. [cite:Robbins 10e Ch 27] 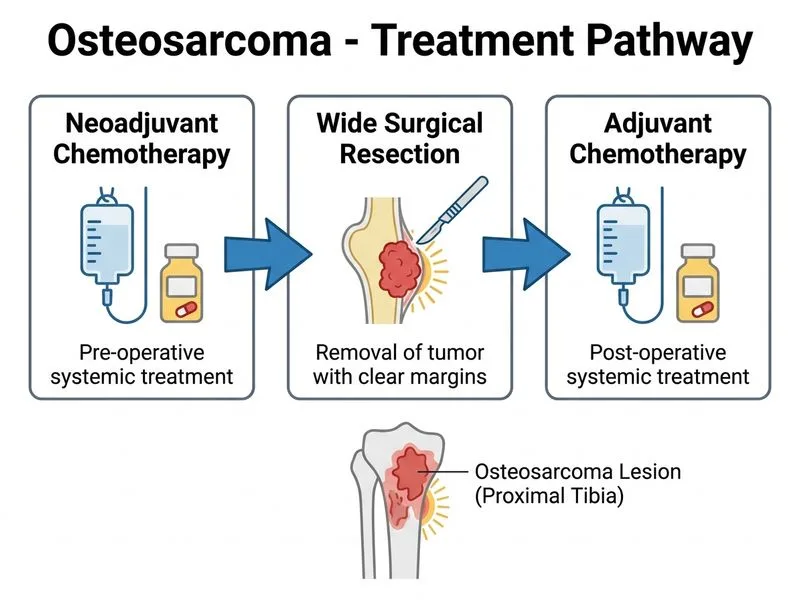
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.