## Clinical Context This is a classic presentation of osteosarcoma in an adolescent: distal femur location, mixed radiographic pattern, Codman's triangle, and elevated alkaline phosphatase. The question asks for the **next step** after clinical suspicion is high. ## Correct Approach: MRI + Chest CT + Core Needle Biopsy **Key Point:** Before any definitive treatment (surgery or chemotherapy), osteosarcoma requires: 1. **Staging imaging** to assess local extent and distant metastases 2. **Tissue diagnosis** via minimally invasive biopsy ### Why This Sequence? **High-Yield:** The modern management algorithm for osteosarcoma is: - **MRI of primary site** → assesses soft tissue involvement, marrow edema, and surgical margins - **Chest CT** → detects pulmonary metastases (present in ~20% at diagnosis) - **Core needle biopsy** → obtains tissue diagnosis with minimal contamination of surgical planes (unlike incisional biopsy, which risks tumor seeding) **Clinical Pearl:** Core needle biopsy is preferred over incisional biopsy because: - Lower risk of tumor cell spillage into surrounding tissues - Preserves surgical margins for limb-salvage planning - Adequate tissue for histology and molecular studies ### Treatment Timeline Once staging and diagnosis are complete: 1. Neoadjuvant chemotherapy (typically 10–12 weeks) 2. Surgical resection (wide excision or amputation based on margin assessment) 3. Adjuvant chemotherapy **Mnemonic:** **SCAT** — **S**taging, **C**ore biopsy, **A**ssess margins, **T**reatment ## Why Staging Before Biopsy? MRI and chest CT are non-invasive and define the surgical plan. Biopsy is the final confirmatory step and should not delay staging imaging. ## Citation [cite:Robbins 10e Ch 26], [cite:Orthopaedic Surgery: Principles and Practice 6e Ch Bone Tumors] 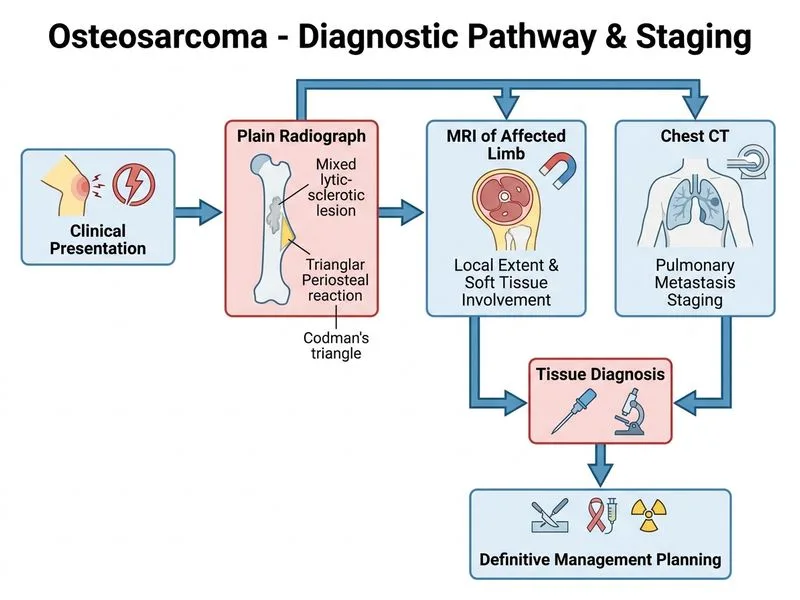
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.