## Explanation: Hormonal Acceleration of Otosclerosis in Pregnancy ### Clinical Context **Key Point:** Otosclerosis shows a well-documented association with pregnancy, with acceleration of hearing loss in 60–70% of affected women during gestation. This patient demonstrates: - **Pre-existing otosclerosis** (progressive hearing loss over 3 years with Carhart notch) - **Acceleration during first pregnancy** (hearing worsened post-partum) - **Further worsening in current pregnancy** (at 6 months gestation) - **Mixed hearing loss** (conductive from stapes fixation + sensorineural from cochlear involvement) ### Pathophysiology of Pregnancy-Related Worsening **High-Yield:** The mechanism involves estrogen-mediated bone remodeling: | Mechanism | Effect | Clinical Outcome | |-----------|--------|------------------| | **Estrogen surge** | Increases osteoclast activity | Accelerated bone turnover | | **Otic capsule** | Enhanced spongiotic remodeling | Faster stapes fixation | | **Cochlear bone** | Increased vascular compromise | Sensorineural component worsens | | **Perilymph** | Altered osmotic pressure | Tinnitus, vertigo exacerbation | **Mnemonic — Why Pregnancy Worsens Otosclerosis: ESTROGENIC** - **E**strogen surge - **S**tapes fixation accelerated - **T**urbulent bone remodeling - **R**esorption of otic capsule - **O**steoclast activation - **G**enetic predisposition unmasked - **E**ndocrine milieu shifts - **N**ew bone formation (pathologic) - **I**ncreased cochlear involvement - **C**onductive + sensorineural loss ### Hormonal Basis **Clinical Pearl:** - **Estrogen receptors** are expressed in osteoblasts and osteoclasts of the otic capsule - **Pregnancy-related estrogen surge** (10–100× baseline) drives osteoclastic bone resorption - **Progesterone** may have a protective effect (less well-defined) - **Post-partum period:** Hearing loss may stabilize or partially improve as hormone levels normalize ### Timing and Progression ```mermaid flowchart TD A[Otosclerosis + Pregnancy]:::outcome --> B{Trimester}:::decision B -->|1st-2nd| C[Estrogen levels rising]:::action B -->|3rd| D[Peak estrogen levels]:::action C --> E[Gradual acceleration of bone remodeling]:::action D --> E E --> F[Hearing loss worsens]:::outcome F --> G{Post-partum}:::decision G -->|Weeks 1-4| H[Hormone levels drop]:::action H --> I[Hearing may plateau or improve slightly]:::outcome G -->|Subsequent pregnancies| J[Further acceleration expected]:::urgent ``` ### Differential Exclusion **Why other options are incorrect:** 1. **Gestational diabetes** → Would cause metabolic cochlear dysfunction, NOT a Carhart notch; diabetes is not a known risk factor for otosclerosis acceleration 2. **Pregnancy-induced endolymphatic hydrops** → Presents with episodic vertigo and fluctuating hearing loss (Ménière-like), not progressive mixed loss with stapes fixation 3. **Perilymphatic fistula from labor Valsalva** → Would present acutely with sudden hearing loss during labor, not gradually during pregnancy; tympanometry would be normal (as it is here), but imaging would show fistula (not mentioned) ### Clinical Management in Pregnancy **High-Yield:** - **Observation** is standard; do NOT perform surgery during pregnancy - **Hearing aids** can be fitted if functional loss is significant - **Sodium fluoride** (controversial; some data suggest benefit, but safety in pregnancy not established) - **Post-partum stapedotomy** is optimal timing (after hormone normalization, typically 3–6 months post-delivery) - **Counsel:** Subsequent pregnancies will likely cause further worsening **Key Point:** The patient should be reassured that while pregnancy accelerates otosclerosis, the condition is not life-threatening and is surgically correctable post-partum. 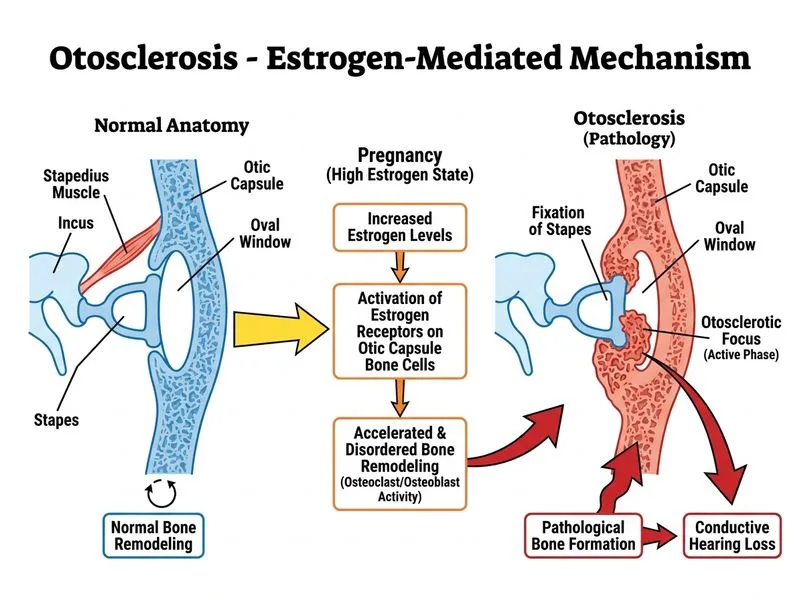
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.