## Prognostic Factors in Ovarian Cancer **Key Point:** In epithelial ovarian cancer, the most powerful independent prognostic factor is the **residual disease status after primary cytoreductive surgery**, not the initial tumor burden or CA-125 level. ### Why Residual Disease Dominates Prognosis **High-Yield:** Patients with **no residual disease (R0)** or **optimal residual disease (<1 cm)** have significantly better 5-year overall survival (60–70%) compared to those with suboptimal residual disease (>1 cm), who have 5-year survival <30%, regardless of stage or grade [cite:Berek & Hacker's Gynecologic Oncology 6e Ch 11]. ### Comparison of Prognostic Factors in Ovarian Cancer | Factor | Impact on Prognosis | Modifiability | |--------|-------------------|----------------| | **Residual disease after surgery** | **Strongest independent predictor** | **Modifiable by surgical skill** | | CA-125 level (preoperative) | Moderate; correlates with burden but not outcome | Not directly modifiable | | Histological grade (G1–G3) | Moderate; G3 worse than G1–G2 | Not modifiable | | Age at diagnosis | Weak to moderate; older age = worse | Not modifiable | | FIGO stage | Moderate; higher stage = worse | Not modifiable | | Platinum sensitivity | Strong predictor of recurrence risk | Depends on chemotherapy response | **Clinical Pearl:** The paradigm shift in ovarian cancer management is that **aggressive cytoreduction to achieve R0 or R1 status is the single most modifiable factor** that surgeons can control to improve survival. This is why neoadjuvant chemotherapy followed by interval debulking is offered if primary optimal cytoreduction is not feasible. ### Treatment Implications **Key Point:** Patients with optimal residual disease (like this case) receive: 1. Platinum–taxane combination chemotherapy (6 cycles) 2. Consideration for bevacizumab (anti-VEGF) maintenance in high-risk disease 3. PARP inhibitor maintenance if BRCA-mutated or homologous recombination deficient Patients with suboptimal residual disease have worse outcomes and may benefit from neoadjuvant chemotherapy in future presentations. **Mnemonic:** **PROS** for optimal cytoreduction: - **P**latinum sensitivity maintained - **R**esidual <1 cm = best survival - **O**verall survival doubled vs. suboptimal - **S**urgical expertise is the key 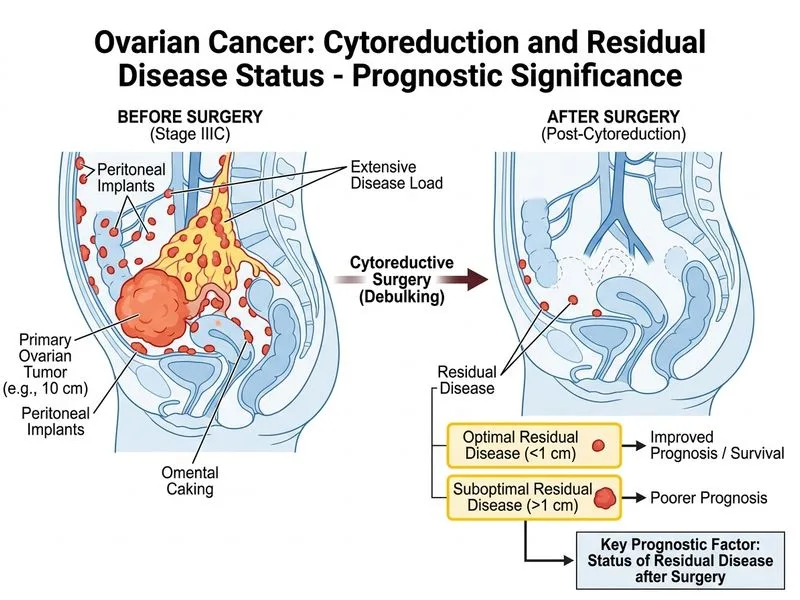
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.