## FIGO Staging for Early Ovarian Cancer **Key Point:** This patient has a unilateral ovarian tumor confined to the ovary (no surface epithelial involvement, no capsular rupture) with no ascites or metastatic disease — this is **FIGO Stage IA**. ### Staging Criteria Breakdown | FIGO Stage | Criteria | | --- | --- | | **IA** | Tumor limited to one ovary; no ascites; intact capsule; no surface epithelial involvement | | **IB** | Tumor limited to both ovaries; otherwise same criteria as IA | | **IC** | Stage IA or IB with any of: capsular rupture, surface epithelial involvement, malignant ascites, or positive peritoneal washings | | **II** | Tumor involves one or both ovaries with pelvic extension | | **III** | Peritoneal metastases beyond pelvis and/or positive retroperitoneal lymph nodes | | **IV** | Distant metastases (pleural effusion with malignant cells, liver parenchymal metastases) | **Clinical Pearl:** In this case, the tumor is **confined to the ovarian stroma** with no surface involvement or capsular breach — all criteria for Stage IA are met. ## Most Important Prognostic Factor in Early Ovarian Cancer **High-Yield:** **Tumor grade (histological differentiation)** is the single most important prognostic factor in early-stage (Stage IA–IC) ovarian cancer. ### Prognostic Hierarchy in Early EOC 1. **Grade (most important)** - Grade 1 (well-differentiated): 5-year OS ~95% - Grade 2 (moderately differentiated): 5-year OS ~75–85% - Grade 3 (poorly differentiated): 5-year OS ~50–65% 2. **Stage** (within early disease, Stage IA > IB > IC) 3. **Histological type** (secondary factor) - Clear-cell and mucinous types are chemotherapy-resistant and have worse outcomes than serous/endometrioid - However, **grade is still more predictive than histology alone** 4. **Age, tumor size, ascites** (tertiary factors) ### Why Histological Type Is Secondary **Warning:** While clear-cell carcinoma is known to be chemotherapy-resistant and carries worse prognosis than serous subtypes, **grade remains the most powerful independent predictor** in multivariate analysis. A Grade 1 clear-cell tumor has better prognosis than a Grade 3 serous tumor. ### Clinical Management Implications **Key Point:** This patient (Stage IA, Grade 3) is at **high risk for recurrence** despite early stage. Treatment recommendations: - **Observation alone:** NOT recommended for Grade 3 tumors - **Adjuvant chemotherapy:** Carboplatin + Paclitaxel × 3–6 cycles is typically offered (ICON1, ACTION trials support adjuvant therapy in high-risk Stage IA–IC) - **Histological type (clear-cell):** Reinforces the need for chemotherapy, as clear-cell tumors are platinum-resistant; some centers consider alternative regimens or clinical trials [cite:FIGO Staging 2014; NCCN Ovarian Cancer Guidelines 2023; Harrison 21e Ch 106] ## Summary: Prognostic Factors in Early Ovarian Cancer ```mermaid flowchart TD A[Early-Stage Ovarian Cancer<br/>Stage IA-IC]:::outcome --> B{Grade?}:::decision B -->|Grade 1| C[Low risk<br/>5-yr OS ~95%]:::outcome B -->|Grade 2| D[Intermediate risk<br/>5-yr OS ~75-85%]:::outcome B -->|Grade 3| E[High risk<br/>5-yr OS ~50-65%]:::urgent C --> F[Observation or<br/>Adjuvant therapy]:::action D --> G[Adjuvant Carboplatin<br/>+ Paclitaxel]:::action E --> H[Adjuvant Carboplatin<br/>+ Paclitaxel ±<br/>Clinical trial]:::action E --> I[Consider histology<br/>Clear-cell/mucinous:<br/>platinum-resistant]:::action ``` 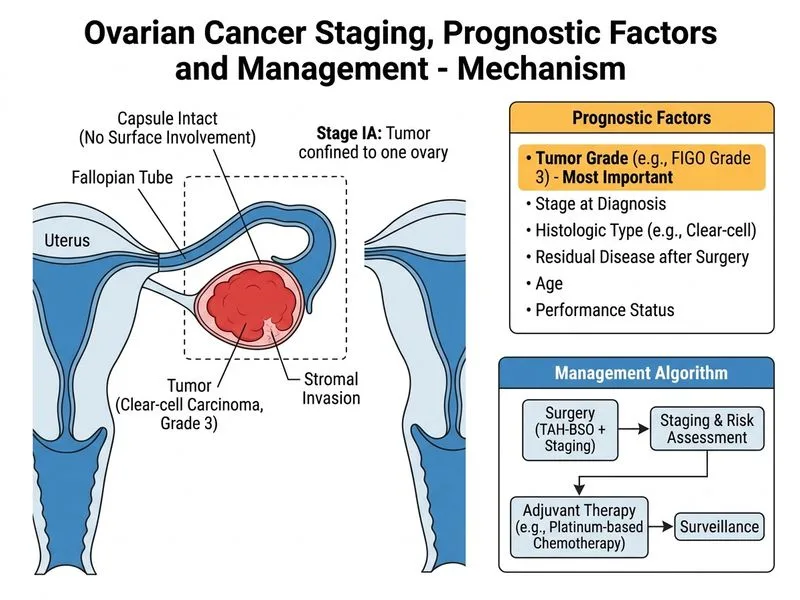
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.